Immunology
HEAD
NISHIKAWA Hiroyoshi
Professor
LAB MEMBER
| Faculty | Position | Researchers |
|---|---|---|
| ITO Sachiko | Senior Lecture | Researchers |
| KOCHIN Vitaly | Designated assistant professor | Researchers |
OUTLINE
The immune system discriminates between self and non-self components and eliminates non-self such as bacteria and virus. Recently, it has been shown that the immune system also plays critical roles in a wide variety of biological activities including cancers, metabolism and pregnancy. Hyper- and hypo-activation of the immune responses, however, induce allergy and autoimmune diseases and chronic infection and cancers, respectively. In cancers, while the immune system controls the development of cancer (immune surveillance), cancer cells survive in the hosts by adapting to the immune-competent environment by reducing their immunogenicity and recruiting immune suppressive cells (immune escape). In our department, we aim at clarifying the detailed mechanisms governing immune surveillance and immune escape through investigating immune homeostasis and immune-associated diseases with basic and translational researches. Then, the entire picture of immune system as a dynamic biological activity would be illuminated.
RESEARCH PROJECTS
1. New cancer immunotherapy approaches focusing on the diversity of T cells.
Actions of various immune cells in tumor environment involve both elimination and survival of cancer cells. In particular, there are cells in the immune system called CD8-positive (CD8 +) T cells that function to eliminate cancer cells. CD8 + T cells are able to selectively attack tumor cells upon proper activation. This involves recognition of the cancer antigen on tumor cells by T cell receptor (TCR) and co-stimulation of its concomitant receptors. On the other hand, tumors create an immunosuppressive environment employing immune checkpoint molecules signaling (such as CTLA-4 and PD1), immune suppressor cells (such as regulatory T cells and tumor associated macrophages), and various cytokines, concerted actions of which result in the tumor's escape from being attacked by the CD8 + T cells. It is believed that the attenuation of immune responses is one of the cancer’s immunosurveillance escape mechanisms. Another factor affecting immune responses could be low diversity of the repertoires of the tumor infiltrating CD8+ T cells. Each CD8+ T cell expresses a single type of TCR. Thus the diversity of CD8+ T cells is determined by the variety of the TCRs. Because each TCR recognizes only a specific part (epitope) of an antigen, the wider the diversity of TCRs, the more epitopes they could target. Therefore, CD8+ T cells with wider TCR repertoires have higher chances to respond to a particular antigen. We have been focusing on the development of new approaches in cancer immunotherapy based on the diversity of CD8+ T cell repertoires. One of our research targets is the process for the generation of TCR diversity in thymus where T cells develop. Studying low diversity TCR repertoires in aging mice is one of the experimental approaches. We are searching for new molecules that control the variability of TCRs and thus could finally affect the numbers of specific CD8+ T cells capable of attacking a tumor. By comparing them to the existing immunotherapy methods, we can assess whether new candidates molecules have therapeutical advantages. Such molecules may further become candidate drugs to restore / control TCR repertoires.
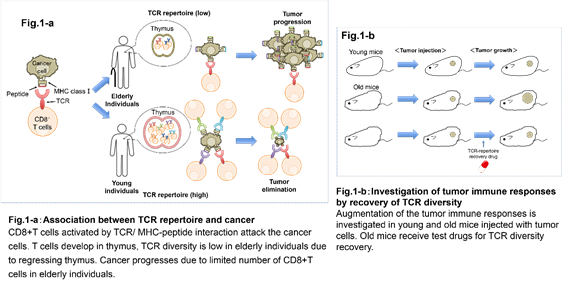
2. Development of new cancer immunotherapy approaches that utilize immune checkpoint inhibitors.
Immune checkpoint inhibitors are expressed when T cell activates. Thus they negatively regulate T cell functions. Normally this system is aimed to suppress autoimmune responses caused by hyperactivation of T cells. On the other hand, tumor environment acts to decrease the host's immune responses by suppressing the activation of T cells using immune checkpoint signaling. Recently, anti-PD-1 antibody has become a central topic in cancer immunotherapy research as it has been shown to enhance the host's immune responses to the tumor by blocking inhibitory PD-1 signaling and thus activating CD8+ T cells. Anti-PD-1 antibody therapy has shown efficacy in refractory cancers. However, due to restrictions in therapeutic effects of the antibody alone, the combination therapy with other drugs seems to be more beneficial. Current clinical trials show that the combination therapy of the antibody with standard regimen anti-cancer drugs has overall survival advantages. We use mouse models in the search for prospective substances which could be effective in the combination therapy. Our research is focused on the development of substances of a viral origin that could be effective in the PD-1 combination therapy.
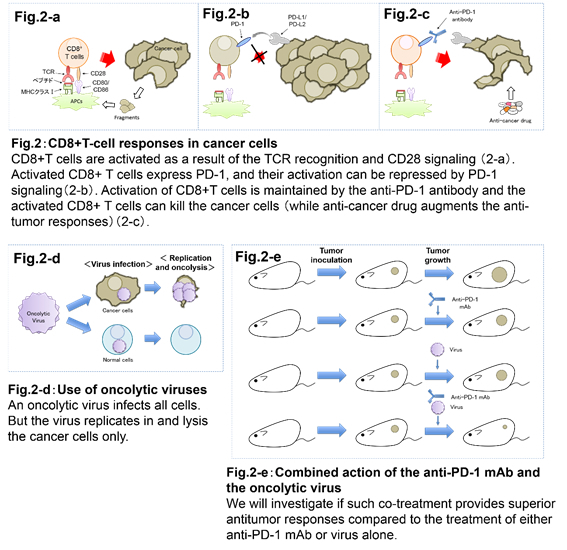
3. Mechanisms of the regulation of transcription factors in immune cells.
Transcription factors regulate expression of genes that control immune cell differentiation, functional properties, migration, etc. For example, FOXP3 is a master regulatory transcription factor in CD4+ regulatory T cells which are immune suppressor cells. T-bet and Eomesodermin (Eomes) are known as master transcription factors which are important in the maintenance of CD8+ T cell functions. Expression of these transcription factors regulates cell's activation and viability. We are analyzing the mechanisms how the expression of these transcription factors is regulated in T cells. Especially in the context of a tumor environment or in response to an antigen stimulation. Using immunoprecipitation and mass spectrometry techniques we are trying to identify new binding partner proteins that interact with and affect functions of these master transcription factors.
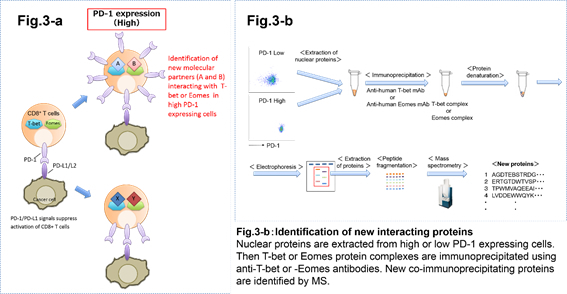
4. Immunotherapy clinical studies involving cancer patients.
It is important to analyze immune responses in cancer patient in order to improve and develop safe and effective immunotherapy regimens. We collaborate with Surgery and Internal medicine departments to analyze tumor tissues and/or blood from cancer patients. In cancer patients the state of immune cells differs between the peripheral blood and the tumor tissue. Thus, comparing immune cells from the peripheral blood and the tumor tissues will allow for new insights in our understanding how the immune response to a tumor develops. We have been collecting samples from cancer patients injected with anti-CTLA-4 and anti-PD-1 antibodies. By comparing the immune responses before and after the antibody therapy, we are aiming to establish the criteria for the effectiveness of the treatment, as well as to establish the causes of autoimmune reactions. In addition, we are analyzing intestinal and oral bacteria to establish new correlations between the microflora and immune responses upon immunotherapy.
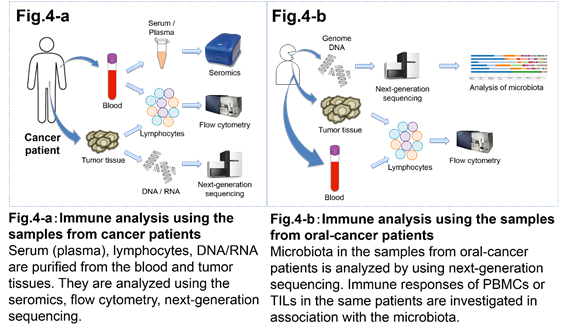
5. Associate Professor Suzuki's group’s research work is based on the immunology of CD8+CD122+ cells.
CD122, the b subunit of the receptor for IL-2, is expressed on around 10% of the total murine CD8+ cells. CD4+ cells that express CD25, the a subunit of the receptor for IL-2, are regulatory T cells, which were identified by Dr. Shimon Sakaguchi. In 2004, I (Suzuki) published that CD8+ cells that express CD122 are also regulatory T cells. In 1995, I had established CD122-KO mice, and since then, I have been working on CD122 and CD8+CD122+ cells.
My research theme has been changing gradually compared to that when CD8+CD122+ cells were first discovered, and has been divided and expanded as follows.
i) CD8+CD122+ cells as regulatory T cells
a) We aimed to focus on some special cell population to isolate pure regulatory T cells. We found CD49d, which seemed rather good, but we are still investigating other candidates by using micro-array methods to find a master gene for CD8+ regulatory T cells that corresponds to foxp3 for CD4+Treg, if possible.
b) The main mechanism of regulation is thought to be the induction of cell death in activated T cells using the Fas/FasL pathway whereas other mechanisms, including cytokines such as IL-10, cannot be excluded.
c) Human CD8+ regulatory T cells
Human CD8+ cells appear somewhat different from that of mice. Apart from CD8+ cells, CD8dim cells exist, which must be NK cells because they are TCR-CD122high. Among CD8+ cells, there are no CD122high cells. Therefore, micro-array analysis was performed to compare between CD8+CD122+ cells and CD8+CD122- cells. We selected one gene, CXCR3, and the antibody against human CXCR3 stained 10~20% of CD8+ cells in human peripheral blood. In mice, only Cxcr3 is expressed in the CD8+CD122+ population. These data suggest that CXCR3 can be used for the marker of CD8+ regulatory T cells in humans instead of CD122 in mice.
d) T cells that prevent or suppress immune disorders after bone marrow transplantation
Although transplantation between individuals that have identical genetic background (syngeneic transplantation) is thought to result in no immune response, the real effects are severe dermatitis occasionally or death by pneumonia when mice that lack Fas or FasL (lpr mice or gld mice) are used (our original experimental results, unpublished yet.) These phenomena do not seem to be caused by the response of the immune system against the graft or host tissue but by some insufficient regulation of immune response against exogenous antigens. We plan to expand the experimental system of bone marrow transplantation and clarify which cells work to prevent and suppress dermatitis and pneumonia (CD8+CD122+CD49dlow cells are highly likely). In the experiment of mixed bone marrow transplantation, it is possible to focus on the target cells by selecting wild-type first, CD8KO or CD4KO next, and so on as the partner of mixed bone marrow transplantation for gld and lpr. (In the preliminary experiment so far, the result showed that the target cells were CD8+). The adaptation of cellular therapy using CD8+ regulatory T cells to immunological disorders after bone marrow transplantation, which could be diagnosed as GVHD (graft versus host disease) without any scientific evidence of response of graft versus host, should become more realistic by analyses that show which cells are responsible for the control of effector T cells.
ii) CD8+CD122+ cells as memory cells
Central memory T cells have almost the same cell surface character as CD8+ regulatory T cells. CD8+CD122+CD62L+ (mouse) and CD8+CXCR3+CD45RO+CCR7+ (human) cells are some examples. They (regulatory and memory) could be the same cells, and sometimes they may show regulatory cell activity or sometimes they may behave like memory cells (at least they are not naive cells). Nevertheless, we plan to examine whether CD8+CD122+CD49dlow cells have memory T cell activity.
iii) Relation to tumor immunity
With regards to the adaptation of CD8+CD122+CD49dlow cells to the clinical field, it is important to know the cells that the regulatory cells affect. It is thought that CD4+Treg directly regulates CD4+ cells and the target for the CD8+ regulatory T cells, that is, the CD8+ cells. (CD4+ cells are also regulated by CD8+ regulatory cells but mainly by CD4+ regulatory cells.) CD8+ cytotoxic T cells are importantly known as the final effector in the rejection of transplanted graft or response to cancer cells, and the recent advance of antibody drugs that aim to enhance the immune response against tumors is remarkable. CD8+ regulatory T cells that directly regulate CD8+ cytotoxic effector T cells must be essentially important players of tumor immunity.
BIBLIOGRAPHY
2025
- Lin N Y-T, Fukuoka S, Koyama S, Motooka D, Tourlousse DM, Shigeno Y, Matsumoto Y, Yamano H, Murotomi K, Tamaki H, Irie T, Sugiyama E, Kumagai S, Itahashi K, Tanegashima T, Fujimaki K, Ito S, Shindo M, Tsuji T, Wake H, Watanabe K, Maeda Y, Enokida T, Tahara M, Yamashita R, Fujisawa T, Nomura M, Kawazoe A, Goto K, Doi T, Shitara K, Mano H, Sekiguchi Y, Nakamura S, Benno Y, Nishikawa H: Microbiota-driven antitumour immunity mediated by dendritic cell migration. Nature. 644(8078):1058-1068 2025.
- Kumagai S, Momoi Y, Nishikawa H: Immunogenomic Cancer Evolution: A framework to understand cancer immunosuppression. Sci Immunol. 10(105):eabo5570 2025 .
- Nishinakamura H, Shinya S, Irie T, Sakihama S, Naito T, Watanabe K, Sugiyama D, Tamiya M, Yoshida T, Hase T, Yoshida T, Karube K, Koyama S, Nishikawa H: Coactivation of innate immune suppressive cells induces acquired resistance against combined TLR agonism and PD-1 blockade. Sci Trans Med 17(785):eadk3160 2025.
- Sato T, Sugiyama D, Koseki J, Kojima Y, Hattori S, Sone K, Nishinakamura H, Ishikawa T, Ishikawa Y, Kato T, Kiyoi H, Nishikawa H: Sustained inhibition of CSF1R signaling augments antitumor immunity through inhibiting tumor-associated macrophages. JCI Insight 10(1):e178146 2025.
- Tsuge A, Watanabe S, Kawazoe A, Togashi Y, Itahashi K, Masuda M, Sai A, Takei S, Muraoka H, Ohkubo S, Sugiyama D, Yan Y, Fukuoka S, Doi T, Shitara K, Koyama S, Nishikawa H: The HSP90 Inhibitor Pimitespib Targets Regulatory T Cells in the Tumor Microenvironment. Cancer Immunol Res. 13(2):273-285 2025.
- Terasaki F, Kumagai S, Fukuda A, Tanaka Y, Irie T, Ito S, Yamada M, Onoe S, Mizuno T, Kokuryo T, Koyama S, Karube K, Nishikawa H, Ebata T: KRAS mutations disrupt interactions between CD8+ T cells and antigen-presenting cells in the tumor microenvironment of biliary tract cancer. Int Immunol. Nov. 4: dxaf065. 2025
- Takahashi J, Tanaka Y, Sato Y, Hashimoto H, Ueno T, Kojima S, Kuroda R, Kondo A, Okumura G, Fukagawa A, Tsuru I, Yamada Y, Takahashi S, Kojima Y, Koyama S, Ushiku T, Nishikawa H, Kume H, Mano H: Spatial multiomic analyses reveal carcinogenic pathways in end-stage renal disease. Cancer Discov. Nov. 20. 2025.
- Nukaga S, Shiraishi K, Hamabe K, Mochizuki A, Hamaguchi Y, Ogawa E, Le NT, Shimada Y, Ono H, Nishinakamura H, Kobayashi Y, Hamamoto J, Ui A, Araki M, Sagae Y, Ohgino K, Sugihara K, Endo S, Miyakoshi J, Shiraishi Y, Yasuda H, Okuno Y, Yoshida T, Goto Y, Ohe Y, Watanabe SI, Yatabe Y, Nishikawa H, Hamamoto R, Kohno T, Nakaoku T: Mutation of CMTR2 in Lung Adenocarcinoma Alters RNA Alternative Splicing and Reveals Therapeutic Vulnerabilities. Nat Commun. 16(1):9754. 2025.
- Matsuura A, Shindo Y, Sugiyama D, Nakagawa T, Hayashi Y, Sano M, Goto Y, Kato S, Nishikawa H, Ogawa K, Ishii M: Association between immunity and antimicrobial treatment resistance in patients with Mycobacterium avium complex pulmonary disease: a multicenter observational study. BMC Infect Dis. 25(1):1394 2025.
- Lin N Y-T, Fukuoka S, Koyama S, Motooka D, Tourlousse DM, Shigeno Y, Matsumoto Y, Yamano H, Murotomi K, Tamaki H, Irie T, Sugiyama E, Kumagai S, Itahashi K, Tanegashima T, Fujimaki K, Ito S, Shindo M, Tsuji T, Wake H, Watanabe K, Maeda Y, Enokida T, Tahara M, Yamashita R, Fujisawa T, Nomura M, Kawazoe A, Goto K, Doi T, Shitara K, Mano H, Sekiguchi Y, Nakamura S, Benno Y, Nishikawa H: Microbiota-driven antitumour immunity mediated by dendritic cell migration. Nature. 644(8078):1058-1068 2025.
- Momoi Y, Kumagai S, Nishikawa H: Immunogenomic precision medicine: a personalized approach based on immunogenomic cancer evolution. Int Immunol. 37(9):517-537 2025.
- Bando H, Kumagai S, Kotani D, Mishima S, Irie T, Itahashi K, Tanaka Y, Habu T, Fukaya S, Kondo M, Tsushima T, Hara H, Kadowaki S, Kato K, Chin K, Yamaguchi K, Kageyama SI, Hojo H, Nakamura M, Tachibana H, Wakabayashi M, Fukui M, Fuse N, Koyama S, Mano H, Nishikawa H, Shitara K, Yoshino T, Kojima T: Atezolizumab following definitive chemoradiotherapy in patients with unresectable locally advanced esophageal squamous cell carcinoma - a multicenter phase 2 trial (EPOC1802). Nat Cancer. 6(3):445-459 2025.
- Jinushi K, Saito T, Kurose K, Suzuki S, Kojima T, Takahara T, Makino T, Ogawa T, Nishikawa H, Kakimi K, Iida S, Nakajima J, Doki Y, Oka M, Ueda R, Wada H: Phase I study on neoadjuvant combination immunotherapy with mogamulizumab and nivolumab for solid tumors. J Immunother Cancer. 13(4):e010634 2025.
- Kumagai S, Momoi Y, Nishikawa H: Immunogenomic Cancer Evolution: A framework to understand cancer immunosuppression. Sci Immunol. 10(105):eabo5570 2025
- Nishinakamura H, Shinya S, Irie T, Sakihama S, Naito T, Watanabe K, Sugiyama D, Tamiya M, Yoshida T, Hase T, Yoshida T, Karube K, Koyama S, Nishikawa H: Coactivation of innate immune suppressive cells induces acquired resistance against combined TLR agonism and PD-1 blockade. Sci Trans Med 17(785):eadk3160 2025.
- Sato T, Sugiyama D, Koseki J, Kojima Y, Hattori S, Sone K, Nishinakamura H, Ishikawa T, Ishikawa Y, Kato T, Kiyoi H, Nishikawa H: Sustained inhibition of CSF1R signaling augments antitumor immunity through inhibiting tumor-associated macrophages. JCI Insight 10(1):e178146 2025 ).
- Tsuge A, Watanabe S, Kawazoe A, Togashi Y, Itahashi K, Masuda M, Sai A, Takei S, Muraoka H, Ohkubo S, Sugiyama D, Yan Y, Fukuoka S, Doi T, Shitara K, Koyama S, Nishikawa H: The HSP90 Inhibitor Pimitespib Targets Regulatory T Cells in the Tumor Microenvironment. Cancer Immunol Res. 13(2):273-285 2025 .
- Wagner M, Nishikawa H, Koyasu S: Reinventing type 2 immunity in cancer. Nature 637(8045):296-303. 2025.
- Koganemaru S, Koyama S, Suto F, Koga M, Inaki K, Kuwahara Y, Arita T, Hirata T, Goto H, Wada N, Kobayashi M, Shibutani T, Okabayashi T, Nakamaru K, Kawazoe A, Togashi Y, Nishikawa H, Shitara K: The Tumor Immune Microenvironment and Therapeutic Efficacy of Trastuzumab Deruxtecan in Gastric Cancer. Cancer Res Commun. 5(1):84-93 2025.
2024
- Kumagai S, Itahashi K, Nishikawa H: Regulatory T cell-mediated immunosuppression orchestrated by cancer: towards an immuno-genomic paradigm for precision medicine. Nat Rev Clin Oncol. 21(5):337-353. 2024.
- Nishikawa H: Establishment of immune suppression by cancer cells in the tumor microenvironment. Proc Jpn Acad Ser B Phys Biol Sci. 100(2):114-122. 2024.
- Kondo M, Kumagai S, Nishikawa H: Metabolic advantages of regulatory T cells dictated by cancer cells. Int Immunol 36(2):75-86 2024 .
- Liu M, Akahori Y, Imai N, Wang L, Negishi K, Kato T, Fujiwara H, Miwa H, Shiku H, Miyahara Y. MAGE-A4 pMHC-targeted CAR-T cells exploiting TCR machinery exhibit significantly improved in vivo function while retaining antigen specificity. J Immunother Cancer. 2024 Nov 20;12(11):e010248. doi: 10.1136/jitc-2024-010248. PMID: 39572159; PMCID: PMC11580264.
- Zhou W, Kawashima S, Ishino T, Kawase K, Ueda Y, Yamashita K, Watanabe T, Kawazu M, Dansako H, Suzuki Y, Nishikawa H, Inozume T, Nagasaki J, Togashi Y: Stem-like progenitor and terminally differentiated TFH-like CD4+ T cell exhaustion in the tumor microenvironment. Cell Rep. 43(2):113797 2024.
- Takei S, Tanaka Y, Lin YT, Koyama S, Fukuoka S, Hara H, Nakamura Y, Kuboki Y, Kotani D, Kojima T, Bando H, Mishima S, Ueno T, Kojima S, Wakabayashi M, Sakamoto N, Kojima M, Kuwata T, Yoshino T, Nishikawa H, Mano H, Endo I, Shitara K, Kawazoe A: Multiomic molecular characterization of the response to combination immunotherapy in MSS/pMMR metastatic colorectal cancer. J Immunother Cancer. 12(2):e008210 2024.
- Naoi Y, Morinaga T, Nagasaki J, Ariyasu R, Ueda Y, Yamashita K, Zhou W, Kawashima S, Kawase K, Honobe-Tabuchi A, Ohnuma T, Kawamura T, Umeda Y, Kawahara Y, Nakamura Y, Kiniwa Y, Yamasaki O, Fukushima S, Kawazu M, Suzuki Y, Nishikawa H, Hanazawa T, Ando M, Inozume T, Togashi Y: CD106 in tumor-specific exhausted CD8+ T cells mediates immunosuppression by inhibiting TCR signaling. Cancer Res. 84(13):2109-2122 2024.
- Habu T, Kumagai S, Bando H, Fujisawa T, Mishima S, Kotani D, Nakamura M, Hojo H, Sakashita S, Kinoshita T, Yano T, Mitsunaga S, Nishikawa H, Koyama S, Kojima T: Definitive chemoradiotherapy induces T-cell-inflamed tumor microenvironment in unresectable locally advanced esophageal squamous cell carcinoma. J Gastroenterol. May 31 2024.
- Tsukada Y, Bando H, Inamori K, Wakabayashi M, Togashi Y, Koyama S, Kotani D, Yuki S, Komatsu Y, Homma S, Taketomi A, Uemura M, Kato T, Fukui M, Nakamura N, Kojima M, Kawachi H, Kirsch R, Yoshida T, Sato A, Nishikawa H, Ito M, Yoshino T: Three-year outcomes of preoperative chemoradiotherapy plus nivolumab in microsatellite stable and microsatellite instability-high locally advanced rectal cancer. Br J Cancer. 131(2):283-289 2024.
- Zhang M, Ono M, Kawaguchi S, Iida M, Chattrairat K, Zhu Z, Nagashima K, Yanagida T, Yamaguchi J, Nishikawa H, Natsume A, Baba Y, Yasui T: On-Site Stimulation of Dendritic Cells by Cancer-Derived Extracellular Vesicles on a Core-Shell Nanowire Platform. ACS Appl Mater Interfaces. 16(23):29570-29580 2024.
- Hisashi Nagase, Takuma Kato, Takayuki Yoshimoto,State-of-the-Art Cancer Immunotherapies,Int J Mol Sci.2024 Feb 22;25(5):2532.
- Yuta Takeuchi, Yizheng Wang, Katsunori Sasaki, Osamu Sato, Takahiro Tsuchikawa, Linan Wang, Yasunori Amaishi, Sachiko Okamoto, Junichi Mineno, Yoshifumi Hirokawa, Kanako C Hatanaka, Yutaka Hatanaka, Takuma Kato, Hiroshi Shiku, Satoshi Hirano,Exhaustion, rather than lack of infiltration and persistence, of CAR-T cells hampers the efficacy of CAR-T therapy in an orthotopic PDAC xenograft model,Biomed Pharmacother. 2024 Jan: 170:116052. Epub 2023 Dec 22.
- Yoshiaki Shimada, Yoshiki Akatsuka, Kazuya Nokura,Bilateral reversible optic neuropathy as the first sign of Waldenström macroglobulinema,Case Reports /GMS Ophthalmol Cases. 2024 Jun 25.
- Wang L, Matsumoto M, Akahori Y, Seo N, Shirakura K, Kato T, Katsumoto Y, Miyahara Y, Shiku H. Preclinical evaluation of a novel CAR-T therapy utilizing a scFv antibody highly specific to MAGE-A4p230-239/HLA-A∗02:01 complex. Mol Ther. 2024 Mar 6;32(3):734-748. doi: 10.1016/j.ymthe.2024.01.018. Epub 2024 Jan 18. PMID: 38243600; PMCID: PMC10928314.
2023
- Kondo M, Kumagai S, Nishikawa H: Metabolic advantages of regulatory T cells dictated by cancer cells. Int Immunol Oct. 14 2023 .
- Sugiyama D, Hinohara K, Nishikawa H: Significance of regulatory T cells in cancer immunology and immunotherapy. Exp Dermatol. 32(3):256-263 2023 .
- Shinichiro K, Maeda Y, Sugiyama D, Watanabe K, Nishikawa H, Hinohara K: The cancer epigenome: non-cell autonomous player in tumor immunity. Cancer Sci. 114(3):730-740 2023 .
- Shiraishi K, Takahashi A, Momozawa Y, Daigo Y, Kaneko S, Kawaguchi T, Kunitoh H, Matsumoto S, Horinouchi H, Goto A, Honda T, Shimizu K, Torasawa M, Takayanagi D, Saito M, Saito A, Ohe Y, Watanabe SI, Goto K, Tsuboi M, Tsuchihara K, Takata S, Aoi T, Takano A, Kobayashi M, Miyagi Y, Tanaka K, Suzuki H, Maeda D, Yamaura T, Matsuda M, Shimada Y, Mizuno T, Sakamoto H, Yoshida T, Goto Y, Yoshida T, Yamaji T, Sonobe M, Toyooka S, Yoneda K, Masago K, Tanaka F, Hara M, Fuse N, Nishizuka SS, Motoi N, Sawada N, Nishida Y, Kumada K, Takeuchi K, Tanno K, Yatabe Y, Sunami K, Hishida T, Miyazaki Y, Ito H, Amemiya M, Totsuka H, Nakayama H, Yokose T, Ishigaki K, Nagashima T, Ohtaki Y, Imai K, Takasawa K, Minamiya Y, Kobayashi K, Okubo K, Wakai K, Shimizu A, Yamamoto M, Iwasaki M, Matsuda K, Inazawa J, Shiraishi Y, Nishikawa H, Murakami Y, Kubo M, Matsuda F, Kamatani Y, Hamamoto R, Matsuo K, Kohno T: Identification of telomere maintenance gene variations related to lung adenocarcinoma risk by genome-wide association and whole genome sequencing analyses. Cancer Commun (Lond). Oct. 26 2023.
- Harusato A, Seo W, Abo H, Nakanishi Y, Nishikawa H, Itoh Y: Protocol for acquiring samples to assess the impact of microplastics on immune microenvironments in the mouse intestine. STAR Protoc. 4(4):102648 2023.
- Hiramatsu H, Yokomori R, Shengyi L, Tanaka N, Mori S, Kiyotani K, Gotoh O, Kusumoto S, Nakano N, Suehiro Y, Ito A, Choi I, Ohtsuka E, Hidaka M, Nosaka K, Yoshimitsu M, Imaizumi Y, Iida S, Utsunomiya A, Noda T, Nishikawa H, Ueda R, Sanda T, Ishida T: Clinical landscape of TP73 structural variants in ATL patients. Leukemia. Oct 20 2023.
- Okuma HS, Watanabe K, Tsuchihashi K, Machida R, Sadachi R, Hirakawa A, Ariyama H, Kanai M, Kamikura M, Anjo K, Hiramitsu A, Sekine S, Okita N, Mano H, Nishikawa H, Nakamura K, Yonemori K: Phase 2 trial of nivolumab in metastatic rare cancer with dMMR or MSI-H and relation with immune phenotypic analysis (the ROCK trial). Clin Cancer Res. Oct 11 2023.
- Ito M, Iwama S, Sugiyama D, Yasuda Y, Okuji T, Kobayashi T, Zhou X, Yamagami A, Onoue T, Miyata T, Sugiyama M, Hagiwara D, Suga H, Banno R, Nishikawa H, Arima H: Anti-tumor effects of anti-programmed cell death-1 antibody treatment are attenuated in streptozotocin-induced diabetic mice. Sci Rep. 13(1):5939. 2023.
- Harusato A, Seo W, Abo H, Nakanishi Y, Nishikawa H, Itoh Y: Impact of particulate microplastics generated from polyethylene terephthalate on gut pathology and immune microenvironments. iScience. 26(4):106474 2023.
- Habu T, Kumanishi R, Ogata T, Fujisawa T, Mishima S, Kotani D, Kadowaki S, Nakamura M, Hojo H, Fujiwara H, Kumagai S, Koyama S, Fujita T, Kinoshita T, Nishikawa H, Yano T, Tajika M, Muro K, Mitsunaga S, Kojima T, Bando H: Complete response to definitive chemoradiotherapy in unresectable locally advanced esophageal squamous cell carcinoma. Esophagus. 20(3):533-540. 2023.
- Barakat C, Inagaki Y, Mizuno S, Nishio N, Katsuyama N, Sato Y, Kobayashi M, Ozeki K, Iida H, Tomita A, Sawa M, Demachi-Okamura A, Takahashi Y, Nishikawa H, Akatsuka Y : Development of TCR-T cell therapy targeting mismatched HLA-DPB1 for relapsed leukemia after allogeneic transplantation.Int J Hematol. 2023 Jun 13. doi: 10.1007/s12185-023-03621-y. Online ahead of print.PMID: 37310580
- Nishiwaki S, Sugiura I, Sato T, Kobayashi M, Osaki M, Sawa M, Adachi Y, Okabe M, Saito S, Morishita T, Kohno A, Nishiyama T, Iida H, Kurahashi S, Kuwatsuka Y, Sugiyama D, Ito S, Nishikawa H, Kiyoi H: Autologous peripheral blood stem cell transplantation for Philadelphia chromosome-positive acute lymphoblastic leukemia is safe but poses challenges for long-term maintenance of molecular remission: Results of the Auto-Ph17 study. EJHaem. 4(2):358-369 2023.
- Hiramatsu H, Nosaka K, Kusumoto S, Nakano N, Choi I, Yoshimitsu M, Imaizumi Y, Hidaka M, Sasaki H, Makiyama J, Ohtsuka E, Jo T, Ogata M, Ito A, Yonekura K, Tatetsu H, Kato T, Kawakita T, Suehiro Y, Ishitsuka K, Iida S, Matsutani T, Nishikawa H, Utsunomiya A, Ueda R, Ishida T: Landscape of immunoglobulin heavy chain gammagene class switch recombination in patients with adult T-cell leukemia-lymphoma. Haematologica. 108(4):1173-1178 2023.(2023)
- Harusato A, Seo W, Abo H, Nakanishi Y, Nishikawa H, Itoh Y : Impact of particulate microplastics generated from polyethylene terephthalate on gut pathology and immune microenvironments.iScience. 2023 Mar 25;26(4):106474. doi: 10.1016/j.isci.2023.106474. eCollection 2023 Apr 21.PMID: 37091249 Free PMC article.
- Ito M, Iwama S, Sugiyama D, Yasuda Y, Okuji T, Kobayashi T, Zhou X, Yamagami A, Onoue T, Miyata T, Sugiyama M, Hagiwara D, Suga H, Banno R, Nishikawa H, Arima H : Anti-tumor effects of anti-programmed cell death-1 antibody treatment are attenuated in streptozotocin-induced diabetic mice.Sci Rep. 2023 Apr 12;13(1):5939. doi: 10.1038/s41598-023-33049-7.PMID: 37046033 Free PMC article.
- Kameda K, Yanagiya R, Miyatake Y, Carreras J, Higuchi H, Murayama H, Ishida T, Ito A, Iida S, Fukuhara N, Harigae H, Fujioka Y, Takahashi N, Wada H, Ishida F, Nakazawa H, Ishihara R, Murakami Y, Tagawa H, Matsuura T, Nakagawa S, Iwabuchi S, Hashimoto S, Imadome KI, Nakamura N, Ishizawa K, Kanda Y, Ando K, Kotani A : Hepatic niche leads to aggressive natural killer cell leukemia proliferation through transferrin-transferrin receptor 1 axis.Blood. 2023 May 5:blood.2022018597. doi: 10.1182/blood.2022018597. Online ahead of print.PMID: 37146246
- Nomura A, Kobayashi T, Seo W, Ohno-Oishi M, Kakugawa K, Muroi S, Yoshida H, Endo TA, Moro K, Taniuchi I : Identification of a novel enhancer essential for Satb1 expression in TH2 cells and activated ILC2s.Life Sci Alliance. 2023 May 16;6(8):e202301897. doi: 10.26508/lsa.202301897. Print 2023 Aug.PMID: 37193606 Free PMC article.
2022
- Shinichiro K, Maeda Y, Sugiyama D, Watanabe K, Nishikawa H, Hinohara K: The cancer epigenome: non-cell autonomous player in tumor immunity. Cancer Sci. 2022 Dec 5. (2022)
- Sugiyama D, Hinohara K, Hiroyoshi N: Significance of regulatory T cells in cancer immunology and immunotherapy. Exp Dermatol. 2022 Dec 2. doi: 10.1111/exd.14721. (2022)
- Hiramatsu H, Nosaka K, Kusumoto S, Nakano N, Choi I, Yoshimitsu M, Imaizumi Y, Hidaka M, Sasaki H, Makiyama J, Ohtsuka E, Jo T, Ogata M, Ito A, Yonekura K, Tatetsu H, Kato T, Kawakita T, Suehiro Y, Ishitsuka K, Iida S, Matsutani T, Nishikawa H, Utsunomiya A, Ueda R, Ishida T: Landscape of immunoglobulin heavy chain gamma gene class switch recombination in patients with adult T-cell leukemia-lymphoma. Haematologica. 2022 Nov 24. (2022)
- Itahashi K, Irie T, Yuda J, Kumagai S, Tanegashima T, Lin Y-Z, Watanabe S, Goto Y, Suzuki J, Aokage K, Tsuboi M, Minami Y, Ishii G, Ohe Y, Ise W, Kurosaki T, Suzuki Y, Koyama S, Nishikawa H: BATF epigenetically and transcriptionally controls the activation program of regulatory T cells in human tumors. Sci Immunol. Epub 2022 Oct 7. (2022)
- Aoki C, Imai K, Mizutani T, Sugiyama D, Miki R, Koya Y, Kobayashi T, Ushida T, Iitani Y, Nakamura N, Owaki T, Nishikawa H, Toyokuni S, Kajiyama H, Kotani T: Molecular hydrogen has a positive impact on pregnancy maintenance through enhancement of mitochondrial function and immunomodulatory effects on T cells. Life Sci. 2022 Sep 15;308:120955. (2022)
- Kelkka T, Tyster M, Lundgren S, Feng X, Kerr C, Hosokawa K, Huuhtanen J, Keränen M, Patel B, Kawakami T, Maeda Y, Nieminen O, Kasanen T, Aronen P, Yadav B, Rajala H, Nakazawa H, Jaatinen T, Hellström-Lindberg E, Ogawa S, Ishida F, Nishikawa H, Nakao S, Maciejewski J, Young NS, Mustjoki S: Anti-COX-2 autoantibody is a novel biomarker of immune aplastic anemia. Leukemia. 2022 Sep;36(9):2317-2327. Epub 2022 Aug 5. (2022)
- Nagaharu K, Kojima Y, Hirose H, Minoura K, Hinohara K, Minami H, Kageyama Y, Sugimoto Y, Masuya M, Nii S, Seki M, Suzuki Y, Tawara I, Shimamura T, Katayama N, Nishikawa H, Ohishi K: A bifurcation concept for B-lymphoid/plasmacytoid dendritic cells with largely fluctuating transcriptome dynamics. Cell Rep. 2022 Aug 30;40(9):111260. (2022)
- Itahashi K, Irie T, Nishikawa H: Regulatory T-cell development in the tumor microenvironment. Eur J Immunol. 2022 Aug;52(8):1216-1227. Epub 2022 Jul 25. (2022)
- Kobayashi T, Kumagai S, Doi R, Afonina E, Koyama S, Nishikawa H: Isolation of tumor-infiltrating lymphocytes from preserved human tumor tissue specimens for downstream characterization. STAR Protoc. 2022 Sep 16;3(3):101557. Epub 2022 Jul 18. (2022)
- Yukami H, Kawazoe A, Lin YT, Koyama S, Fukuoka S, Hara H, Takahashi N, Kojima T, Asayama M, Yoshii T, Bando H, Kotani D, Nakamura Y, Kuboki Y, Mishima S, Wakabayashi M, Kuwata T, Goto M, Higuchi K, Yoshino T, Doi T, Nishikawa H, Shitara K: Updated efficacy outcomes of anti-PD-1 antibodies plus multikinase inhibitors for advanced gastric cancer patients with or without liver metastases in clinical trials. Clin Cancer Res. 2022 Aug 15;28(16):3480-3488. (2022)
- Miyai Y, Sugiyama D, Hase T, Asai N, Taki T, Nishida K, Fukui T, Chen-Yoshikawa TF, Kobayashi H, Mii S, Shiraki Y, Hasegawa Y, Nishikawa H, Ando Y, Takahashi M, Enomoto A: Meflin-positive cancer-associated fibroblasts enhance tumor response to immune checkpoint blockade. Life Sci Alliance. 2022 Mar 2;5(6):e202101230. Print 2022 Jun. (2022)
- Goda N, Sasada S, Shigematsu H, Masumoto N, Arihiro K, Nishikawa H, Sakaguchi S, Okada M, Kadoya T: The ratio of CD8 + lymphocytes to tumor-infiltrating suppressive FOXP3 + effector regulatory T cells is associated with treatment response in invasive breast cancer. Discov Oncol. 2022 Apr 19;13(1):27. (2022)
- Ong JZL, Yokomori R, Wong RWJ, Tan TK, Ueda R, Ishida T, Iida S, Sanda T: Requirement for TP73 and genetic alterations originating from its intragenic super-enhancer in adult T-cell leukemia. Leukemia. 2022 Sep;36(9):2293-2305. Epub 2022 Jul 30. (2022)
- Sakamoto Y, Ishida T, Masaki A, Murase T, Ohtsuka E, Takeshita M, Muto R, Iwasaki H, Ito A, Kusumoto S, Nakano N, Tokunaga M, Yonekura K, Tashiro Y, Iida S, Utsunomiya A, Ueda R, Inagaki H: CCR7 alterations associated with inferior outcome of adult T-cell leukemia/lymphoma under mogamulizumab treatment. Hematol Oncol. 2022 Aug 31. (2022)
- Tanaka N, Mori S, Kiyotani K, Ota Y, Gotoh O, Kusumoto S, Nakano N, Suehiro Y, Ito A, Choi I, Ohtsuka E, Hidaka M, Nosaka K, Yoshimitsu M, Imaizumi Y, Iida S, Utsunomiya A, Noda T, Nishikawa H, Ueda R, Ishida T: Genomic determinants impacting the clinical outcome of mogamulizumab treatment for adult T-cell leukemia/lymphoma. Haematologica. 2022 Apr 14. (2022)
- Aokage K, Tsuboi M, Zenke Y, Horinouchi H, Nakamura N, Ishikura S, Nishikawa H, Kumagai S, Koyama S, Kanato K, Kataoka T, Wakabayashi M, Fukutani M, Fukuda H, Ohe Y, Watanabe SI; Lung Cancer Surgical Study Group of the Japan Clinical Oncology Group: Study protocol for JCOG1807C (DEEP OCEAN): a interventional prospective trial to evaluate the efficacy and safety of durvalumab before and after operation or durvalumab as maintenance therapy after chemoradiotherapy against superior sulcus non-small cell lung cancer. Jpn J Clin Oncol. 2022 Apr 6;52(4):383-387. (2022)
- Hasegawa H, Shitara K, Takiguchi S, Takiguchi N, Ito S, Kochi M, Horinouchi H, Kinoshita T, Yoshikawa T, Muro K, Nishikawa H, Suna H, Kodera Y: A multicenter, open-label, single-arm phase I trial of neoadjuvant nivolumab monotherapy for resectable gastric cancer. Gastric Cancer. 2022 Mar 7. (2022)
- Kumagai S, Koyama S, Itahashi K, Tanegashima T, Lin Y-T, Togashi Y, Kamada T, Irie T, Okumura G, Kohno H, Ito D, Fujii R, Watanabe S, Sai A, Fukuoka S, Sugiyama E, Watanabe G, Owari T, Nishinakaumra H, Sugiyama D, Maeda Y, Kawazoe A, Yukami H, Cida K, Ohara Y, Yoshida T, Shinno Y, Takeyasu Y, Shirasawa M, Nakama K, Aokage K, Suzuki J, Ishii G, Kuwata T, Sakamoto N, Kawazu M, Ueno T, Mori T, Yamazaki N, Tsuboi M, Yatabe Y, Kinoshita T, Doi T, Shitara K, Mano H, Nishikawa H: Lactic acid promotes PD-1 expression in regulatory T cells in highly glycolytic tumor microenvironments. Cancer Cell. 2022 Jan 25:S1535-6108(22)00003-4. (2022)
- Nagasaki J, Inozume T, Sax N, Ariyasu R, Ishikawa M, Yamashita K, Kawazu M, Ueno T, Irie T, Tanji E, Morinaga T, Honobe A, Ohnuma T, Yoshino M, Iwata T, Kawase K, Sasaki K, Hanazawa T, Kochin V, Kawamura T, Matsue H, Hino M, Mano H, Suzuki Y, Nishikawa H, Togashi Y: PD-1 blockade therapy promotes infiltration of tumor-attacking exhausted T cell clonotypes. Cell Rep. 2022 Feb 1;38(5):110331. (2022)
- Bando H, Tsukada Y, Inamori K, Togashi Y, Koyama S, Kotani D, Fukuoka S, Yuki S, Komatsu Y, Homma S, Taketomi A, Uemura M, Kato T, Fukui M, Wakabayashi M, Nakamura N, Kojima M, Kawachi H, Kirsch R, Yoshida T, Suzuki Y, Sato A, Nishikawa H, Ito M, Yoshino T: Preoperative Chemoradiotherapy Plus Nivolumab Before Surgery in Microsatellite Stable and Microsatellite Instability-High Locally Advanced Rectal Cancer Patients. Clin Cancer Res. 2022 Jan 21:clincanres.3213.2021. (2022)
- Aokage K, Tsuboi M, Zenke Y, Horinouchi H, Nakamura N, Ishikura S, Nishikawa H, Kumagai S, Koyama S, Kanato K, Kataoka T, Wakabayashi M, Fukutani M, Fukuda H, Ohe Y, Watanabe SI; Lung Cancer Surgical Study Group of the Japan Clinical Oncology Group: Study protocol for JCOG1807C (DEEP OCEAN): a interventional prospective trial to evaluate the efficacy and safety of durvalumab before and after operation or durvalumab as maintenance therapy after chemoradiotherapy against superior sulcus non-small cell lung cancer. Jpn J Clin Oncol. 2022 Jan 7:hyab208. (2022)
- Okamoto A, Fujigaki H, Iriyama C, Goto N, Yamamoto H, Mihara K, Inaguma Y, Miura Y, Furukawa K, Yamamoto Y, Akatsuka Y, Kasahara S, Miyao K, Tokuda M, Sato S, Mizutani Y, Osawa M, Hattori K, Iba S, Kajiya R, Okamoto M, Saito K, Tomita A: CD19-positive lymphocyte count is critical for acquisition of anti-SARS-CoV-2 IgG after vaccination in B-cell lymphoma. Blood Adv. 2022 Jan 13:bloodadvances.2021006302. (2022)
- Harusato A, Chassaing B, Dauriat CJG, Ushiroda C, Seo W, Itoh Y: Dietary Emulsifiers Exacerbate Food Allergy and Colonic Type 2 Immune Response through Microbiota Modulation. Nutrients. 2022 Nov 23;14(23):4983. doi: 10.3390/nu14234983. (2022)
- Seo W, Nomura A, Taniuchi I: The Roles of RUNX Proteins in Lymphocyte Function and Anti-Tumor Immunity: Cells. 2022 Oct 3;11(19):3116. doi: 10.3390/cells11193116. (2022)
2021
- Maeda Y, Wada H, Sugiyama D, Saito T, Irie T, Itahashi K, Minoura K, Suzuki S, Kojima T, Kakimi K, Nakajima J, Funakoshi T, Iida S, Oka M, Shimamura T, Doi T, Doki Y, Nakayama E, Ueda R, Nishikawa H: Depletion of central memory CD8 + T cells might impede the antitumor therapeutic effect of Mogamulizumab. Nat Commun. 12(1):7280 2021.
- Takeuchi Y, Tanegashima T, Sato E, Irie T, Sai A, Itahashi K, Kumagai S, Tada Y, Togashi Y, Koyama S, Akbay E.A, Karasaki T, Kataoka K, Funaki S, Shintani Y, Nagatomo I, Kida H, Ishii G, Miyoshi T, Aokage K, Kakimi K, Ogawa S, Okumura M, Eto M, Kumanogoh A, Tsuboi M, Nishikawa H: Highly immunogenic cancer cells require activation of the WNT pathway for immunological escape. Sci Immunol. 6(65):eabc6424 2021.
- Kumagai S, Koyama S, Nishikawa H: Antitumour immunity regulated by aberrant ERBB family signalling. Nat Rev Cancer. 21(3):181-197 2021.
- Isoyama S, Mori S, Sugiyama D, Kojima Y, Tada Y, Shitara K, Hinohara K, Dan S, Nishikawa H: Cancer immunotherapy with PI3K and PD-1 dual-blockade via optimal modulation of T cell activation signal. J Immunother Cancer. 9(8):e002279 2021.
- Watanabe K, Nishikawa H: Engineering strategies for broad application of TCR-T and CAR-T cell therapies. Int Immunol. 33(11):551-562 2021.
- Koyama S, Nishikawa H: Mechanisms of regulatory T cell infiltration in tumors: implications for innovative immune precision therapies. J Immunother Cancer. 9(7):e002591 2021.
- Satoh K, Kobayashi Y, Fujimaki K, Hayashi S, Ishida S, Sugiyama D, Sato T, Kyungtaek L, Miyamoto M, Kozuma S, Kadokura M, Wakita K, Hata M, Hirahara K, Amano M, Watanabe I, Okamoto A, Tuettenberg A, Jonuleit H, Tanemura A, Maruyama S, Agatsuma T, Wada T, Nishikawa H: Novel anti-GARP antibody DS-1055a augments antitumor immunity by depleting highly suppressive GARP+ regulatory T cells. Int Immunol. 33(8):435-446 2021.
- Inamori K, Togashi Y, Fukuoka S, Akagi K, Ogasawara K, Irie T, Motooka D, Kobayashi Y, Sugiyama D, Kojima M, Shiiya N, Nakamura S, Maruyama S, Suzuki Y, Ito M, Nishikawa H: Importance of lymph node immune responses in MSI-H/dMMR colorectal cancer. JCI Insight. 6(9):137365. 2021.
- Seo W, Jerin C, Nishikawa H: Transcriptional regulatory network for the establishment of CD8 + T cell exhaustion. Exp Mol Med. 53(2):202-209 2021.
- Arakawa A, Ichikawa H, Kubo T, Motoi N, Kumamoto T, Nakajima M, Yonemori K, Noguchi E, Sunami K, Shiraishi K, Kakishima H, Yoshida H, Hishiki T, Kawakubo N, Kuroda T, Kiyokawa T, Yamada K, Yanaihara N, Takahashi K, Okamoto A, Hirabayashi S, Hasegawa D, Manabe A, Ono K, Matsuoka M, Arai Y, Togashi Y, Shibata T, Nishikawa H, Aoki K, Yamamoto N, Kohno T, Ogawa C: Vaginal Transmission of Cancer from Mothers with Cervical Cancer to Infants. N Engl J Med. 384(1):42-50 2021.
- Yasuda Y, Iwama S, Sugiyama D, Okuji T, Kobayashi T, Ito M, Okada N, Enomoto A, Ito S, Yan Y, Sugiyama M, Onoue T, Tsunekawa T, Ito Y, Takagi H, Hagiwara D, Goto M, Suga H, Banno R, Takahashi M, Nishikawa H, Arima H: CD4+ T cells are essential for the development of destructive thyroiditis induced by anti-PD-1 antibody in thyroglobulin-immunized mice. Sci Transl Med. 13(593):eabb7495 2021.
- Kawazu M, Ueno T, Saeki K, Sax N, Togashi Y, Kaneseki T, Chida K, Kishigami F, Sato K, Kojima S, Otsuka M, Kawazoe A, Nishinakamura H, Maeda Y, Yamamoto Y, Yamashita K, Inoue S, Tanegashima T, Matsubara D, Tane K, Tanaka Y, Iinuma H, Hashiguchi Y, Hazama S, Khor SS, Tokunaga K, Tsuboi M, Niki T, Eto M, Shitara K, Torigoe T, Ishihara S, Aburatani H, Haeno H, Nishikawa H, Mano H: HLA Class I analysis provides insight into the genetic and epigenetic background of immune evasion in colorectal cancer with high microsatellite instability Gastroenterology. S0016-5085(21)03644-1 2021.
- Kawazoe A, Itahashi K, Yamamoto N, Kotani D, Kuboki Y, Taniguchi H, Harano K, Naito Y, Suzuki M, Fukutani M, Higuchi T, Ikeno T, Wakabayashi M, Sato A, Koyama S, Nishikawa H, Shitara K: TAS-116 (Pimitespib), an Oral HSP90 Inhibitor, in Combination with Nivolumab in Patients with Colorectal Cancer and Other Solid Tumors: An Open-Label, Dose-Finding, and Expansion Phase Ib Trial (EPOC1704). Clin Cancer Res. 27(24):6709-6715 2021.
- Kawashima S, Inozume T, Kawazu M, Ueno T, Nagasaki J, Tanji E, Honobe A, Ohnuma T, Kawamura T, Umeda Y, Nakamura Y, Kawasaki T, Kiniwa Y, Yamasaki O, Fukushima S, Ikehara Y, Mano H, Suzuki Y, Nishikawa H, Matsue H, Togashi Y: TIGIT/CD155 axis mediates resistance to immunotherapy in patients with melanoma with the inflamed tumor microenvironment J Immunother Cancer. 9(11):e003134 2021.
- Kobayashi T, Iwama S, Sugiyama D, Yasuda Y, Okuji T, Ito M, Ito S, Sugiyama M, Onoue T, Takagi H, Hagiwara D, Ito Y, Suga H, Banno R, Nishikawa H, Arima H: Anti-pituitary antibodies and susceptible human leukocyte antigen alleles as predictive biomarkers for pituitary dysfunction induced by immune checkpoint inhibitors. J Immunother Cancer. 9(5):e002493 2021.
- Kitahara M, Shigeno Y, Shime M, Matsumoto Y, Nakamura S, Motooka D, Fukuoka S, Nishikawa H, Benno Y: Vescimonas gen. nov., Vescimonas coprocola sp. nov., Vescimonas fastidiosa sp. nov., Pusillimonasgen. nov. and Pusillimonas faecalis sp. nov. isolated from human faeces Int J Syst Evol Microbiol. Nov;71(11) 2021.
- Kelkka T, Savola P, Bhattacharya D, Huuhtanen J, Lönnberg T, Kankainen M, Paalanen K, Tyster M, Lepistö M, Ellonen P, Smolander J, Eldfors S, Yadav B, Khan S, Koivuniemi R, Sjöwall C, Elo LL, Lähdesmäki H, Maeda Y, Nishikawa H, Leirisalo-Repo M, Sokka-Isler T, Mustjoki S.: Adult-onset anti-citrullinated peptide antibody-negative destructive rheumatoid arthritis is characterized by a disease-specific CD8+ T lymphocyte signature. Front Immunol. 12:710831 2021.
- Kashima Y, Togashi Y, Fukuoka S, Kamada T, Irie T, Suzuki A, Nakamura Y, Shitara K, Minamide T, Yoshida T, Taoka N, Kawase T, Wada T, Inaki K, Chihara M, Ebisuno Y, Tsukamoto S, Fujii R, Ohashi A, Suzuki Y, Tsuchihara K, Nishikawa H, Doi T: Potentiality of multiple modalities for single-cell analyses to evaluate the tumor microenvironment in clinical specimens. Sci Rep. 11(1):341 2021.
- Fujioka Y, Sugiyama D, Matsumura I, Minami Y, Miura M, Atsuta Y, Ohtake S, Kiyoi H, Miyazaki Y, Nishikawa H, Takahashi N: Regulatory T Cell as a Biomarker of Treatment-Free Remission in Patients with Chronic Myeloid Leukemia. Cancers. 13(23):5904 2021.
- Nozaki K, Fujioka Y, Sugiyama D, Ishikawa J, Iida M, Shibata M, Kosugi S, Nishikawa H, Shibayama H: Flow cytometry analysis of peripheral Tregs in patients with multiple myeloma under lenalidomide maintenance. Int J Hematol. 113(5):772-774 2021.
- Chen S, Kiguchi T, Nagata Y, Tamai Y, Ikeda T, Kajiya R, Ono T, Sugiyama D, Nishikawa H, Akatsuka Y: A simple method to distinguish residual elotuzumab from monoclonal paraprotein in immunofixation assays for multiple myeloma patients. Int J Hematol. 113(4):473-479 2021.
- Watanabe S, Goto Y, Yasuda H, Kohno T, Motoi N, Ohe Y, Nishikawa H, Kobayashi SS, Kuwano K, Togashi Y.: HSP90 inhibition overcomes EGFR amplification-induced resistance to third-generation EGFR-TKIs. Thorac Cancer. 12(5):631-642 2021.
- Sakamoto Y, Ishida T, Masaki A, Takeshita M, Iwasaki H, Yonekura K, Tashiro Y, Ito A, Kusumoto S, Iida S, Utsunomiya A, Ueda R, Inagaki H: Clinicopathological significance of CD28 overexpression in adult T-cell leukemia/lymphoma. Cancer Sci. 2022 Jan;113(1):349-361. doi: 10.1111/cas.15191. Epub 2021 Nov 29. (2021)
- Sakamoto Y, Ishida T, Masaki A, Murase T, Takeshita M, Muto R, Iwasaki H, Ito A, Kusumoto S, Nakano N, Tokunaga M, Yonekura K, Tashiro Y, Iida S, Utsunomiya A, Ueda R, Inagaki H: Clinical significance of TP53 mutations in adult T-cell leukemia/lymphoma. Br J Haematol. 2021 Nov;195(4):571-584. doi: 10.1111/bjh.17749. Epub 2021 Aug 17. (2021)
- Nosaka K, Kusumoto S, Nakano N, Choi I, Yoshimitsu M, Imaizumi Y, Hidaka M, Sasaki H, Makiyama J, Ohtsuka E, Jo T, Ogata M, Ito A, Yonekura K, Tatetsu H, Kato T, Kawakita T, Suehiro Y, Ishitsuka K, Iida S, Matsutani T, Utsunomiya A, Ueda R, Ishida T: Clinical significance of the immunoglobulin G heavy-chain repertoire in peripheral blood mononuclear cells of adult T-cell leukaemia-lymphoma patients receiving mogamulizumab. Br J Haematol. 2022 Feb;196(3):629-638. doi: 10.1111/bjh.17895. Epub 2021 Oct 10. (2021)
- Kikuchi Y, Tokita S, Hirama T, Kochin V, Nakatsugawa M, Shinkawa T, Hirohashi Y, Tsukahara T, Hata F, Takemasa I, Sato N, Kanaseki T, Torigoe T: CD8+ T-cell Immune Surveillance against a Tumor Antigen Encoded by the Oncogenic Long Noncoding RNA PVT1. Cancer Immunol Res. 2021 Nov;9(11):1342-1353. doi: 10.1158/2326-6066.CIR-20-0964. Epub 2021 Aug 25.
- Yokoyama S, Takahashi A, Kikuchi R, Nishibu S, Lo JA, Hejna M, Moon WM, Kato S, Zhou Y, Hodi FS, Song JS, Sakurai H, Fisher DE, Hayakawa Y: SOX10 Regulates Melanoma Immunogenicity through an IRF4-IRF1 Axis. Cancer Res. 2021 Dec 15;81(24):6131-6141. doi: 10.1158/0008-5472.CAN-21-2078. Epub 2021 Nov 2. (2021)
- Takashima H, Sato Boku A, Miyamoro H, Kato S, Furuno S, Shibuya Y: Perioperative management of von Willebrand patients at the time of implant placement: Case report. Clin Case Rep. 2021 Aug 30;9(9):e04755. doi: 10.1002/ccr3.4755.(2021)
- Allouche J, Rachmin I, Adhikari K, Pardo LM, Lee JH, McConnell AM, Kato S, Fan S, Kawakami A, Suita Y, Wakamatsu K, Igras V, Zhang J, Navarro PP, Lugo CM, Noonan HR, Christie KA, Itin K, Mujahid N, Lo JA, Won CH, Evans CL, Weng QY, Wang H, Osseiran S, Lovas A, Németh I, Cozzio A, Navarini AA, Hsiao JJ, Nguyen N, Kemény LV, Iliopoulos O, Berking C, Ruzicka T, Gonzalez-José R, Bortolini MC, Canizales-Quinteros S, Acuna-Alonso V, Gallo C, Poletti G, Bedoya G, Rothhammer F, Ito S, Schiaffino MV, Chao LH, Kleinstiver BP, Tishkoff S, Zon LI, Nijsten T, Ruiz-Linares A, Fisher DE, Roider E: NNT mediates redox-dependent pigmentation via a UVB- and MITF-independent mechanism. Cell. 2021 Aug 5;184(16):4268-4283.e20. doi: 10.1016/j.cell.2021.06.022. Epub 2021 Jul 6. (2021)
- Kemény LV, Robinson KC, Hermann AL, Walker DM, Regan S, Yew YW, Lai YC, Theodosakis N, Rivera PD, Ding W, Yang L, Beyer T, Loh YE, Lo JA, van der Sande AAJ, Sarnie W, Kotler D, Hsiao JJ, Su MY, Kato S, Kotler J, Bilbo SD, Chopra V, Salomon MP, Shen S, Hoon DSB, Asgari MM, Wakeman SE, Nestler EJ, Fisher: Vitamin D deficiency exacerbates UV/endorphin and opioid addiction. Science Advances. 2021 Jun 11;7(24):eabe4577. doi: 10.1126/sciadv.abe4577 (2021)
2020
- Kumagai S, Togashi Y, Kamada T, Sugiyama E, Nishinakaumra H, Takeuchi Y, Kochin, V, Itahashi K, Maeda Y, Matsui S, Shibahara,T, Yamashita Y, Irie T, Tsuge A, Fukuoka S, Kawazoe A, Udagawa H, Kirita K, Aokage K, Ishii G, Kuwata T, Nakama K, Kawazu M, Ueno T, Yamazaki N, Goto K, Tsuboi M, Mano H, Doi T, Shitara K, Nishikawa H: The PD-1 expression balance between effector and regulatory T cell predicts the clinical efficacy of PD-1 blockade therapies. Nat Immunol. 21(11):1346-1358 2020.
- Kumagai S, Togashi Y, Sakai C, Kawazoe A, Kawazu M, Ueno T, Sato E, Kuwata T, Kinoshita T, Yamamoto M, Nomura S, Tsukamoto T, Mano H, Shitara K, Nishikawa H: An oncogenic alteration creates a tumor microenvironment that promotes tumor progression by conferring a metabolic advantage to regulatory T cells. Immunity. 53(1):187-203.e8 2020.
- Sugiyama E, Togashi Y, Takeuchi Y, Shinya S, Tada, Y, Kataoka K, Tane K, Sato E, Ishii G, Goto K, Shintani Y, Okumura M, Tsuboi M, Nishikawa H.: Blockade of EGFR improves responsiveness to PD1 blockade in EGFR-mutated non-small cell lung cancer. Sci Immunol 5(43). pii: eaav3937 2020.
- Nagasaki J, Togashi Y, Sugawara T, Itami M, Yamauchi N, Yuda J, Sugano M, Ohara Y, Minami Y, Nakamae H, Hino M, Takeuchi M, Nishikawa H: The critical role of CD4+ T cells in PD-1 blockade against MHC-II-expressing tumors such as classic Hodgkin lymphoma. Blood Adv. 4(17):4069-4082 2020.
- Muramatsu T, Noguchi T, Sugiyama D, Kanada Y, Fujimaki K, Ito S, Gotoh M, Nishikawa H: Newly emerged immunogenic neoantigens in established tumors enable hosts to regain immunosurveillance in a T cell-dependent manner. Int Immunol. Jul 30: dxaa049 2020.
- Tanaka A*, Nishikawa H*, Noguchi S* (*equally contributed), Sugiyama D, Morikawa H, Takeuchi Y, Ha D, Shigeta N, Kitawaki T, Maeda Y, Saito T, Shinohara Y, Kameoka Y, Iwaisako K, Monma F, Ohishi K, Karbach J, Jäger E, Sawada K, Katayama N, Takahashi N, Sakaguchi S.: Tyrosine kinase inhibitor imatinib augments tumor immunity by depleting effector regulatory T cells. J Exp Med. 217(2): 2020.
- Umemoto K, Togashi Y, Arai Y, Nakamura H, Takahashi S, Tanegashima T, Kato M, Nishikawa T, Sugiyama D, Kojima M, Gotohda N, Kuwata T, Ikeda M, Shibata T, Nishikawa H.: The potential application of PD-1 blockade therapy for early-stage biliary tract cancer. Int Immunol. 32(4):273-281 2020.
- Kawazoe A, Kuboki Y, Shinozaki E, Hara H, Nishina T, Komatsu Y, Yuki S, Wakabayashi M, Nomura S, Sato A, Kuwata T, Kawazu M, Mano H, Togashi Y, Nishikawa H, Yoshino T: Multicenter phase 1/2 Trial of napabucasin and pembrolizumab in patients with metastatic colorectal cancer (EPOC1503/SCOOP Trial). Clin Cancer Res. 2020 Jul 21:clincanres.1803 2020.
- Fukuoka S, Hara H, Takahashi N, Kojima T, Kawazoe A, Asayama M, Yoshii T, Kotani D, Tamura H, Mikamoto Y, Hirano N, Wakabayashi M, Nomura S, Sato A, Kuwata T, Togashi Y, Nishikawa H, Shitara K: Regorafenib Plus Nivolumab in Patients With Advanced Gastric or Colorectal Cancer: An Open-Label, Dose-Escalation, and Dose-Expansion Phase Ib Trial (REGONIVO, EPOC1603) J Clin Oncol. 38(18):2053-2061 2020.
- Minoura K, Abe K, Maeda Y, Nishikawa H, Shimamura T.: CYBERTRACK2.0: zero-inflated model-based cell clustering and population tracking method for longitudinal mass cytometry data. Bioinformatics. Oct 14:btaa873 2020.
- Abe K, Minoura K, Maeda Y, Nishikawa H, Shimamura T.: Model-based clustering for flow and mass cytometry data with clinical information. BMC Bioinformatics. Sep 17;21(Suppl 13):393 2020.
- Murate K, Maeda K, Nakamura M, Sugiyama D, Wada H, Yamamura T, Sawada T, Mizutani Y, Ishikawa T, Furukawa K, Ohno E, Honda T, Kawashima H, Miyahara R, Ishigami M, Nishikawa H, Fujishiro M.: Endoscopic Activity and Serum TNF-α Level at Baseline Are Associated With Clinical Response to Ustekinumab in Crohn's Disease Patients. Inflamm Bowel Dis. 2020 May 14 2020.
- Bando H, Kotani D, Tsushima T, Hara H, Kadowaki S, Kato K, Chin K, Yamaguchi K, Kageyama SI, Hojo H, Nakamura M, Tachibana H, Wakabayashi M, Fukutani M, Togashi Y, Fuse N, Nishikawa H, Kojima T.: TENERGY: Multicenter Phase II Study of Atezolizumab Monotherapy Following Definitive Chemoradiotherapy With 5-FU Plus Cisplatin in Patients With Unresectable Locally Advanced Esophageal Squamous Cell Carcinoma. BMC Cancer. 20(1):336 2020.
- Sasaki A, Nakamura Y, Togashi Y, Kuno H, Hojo H, Kageyama S, Nakamura N, Takashima K, Kadota T, Yoda Y, Mishima S, Sawada K, Kotani D, Kawazoe A, Kuboki Y, Taniguchi H, Kojima T, Doi T, Yoshino T, Yano T, Kobayashi T, Akimoto T, Nishikawa H, Shitara K.: Enhanced Tumor Response to Radiotherapy After PD-1 Blockade in Metastatic Gastric Cancer. Gastric Cancer. 23(5):893-903.2020.
- Akatsuka Y: TCR-Like CAR-T Cells Targeting MHC-Bound Minor Histocompatibility Antigens.Frontiers in Immunology.28 February 2020.doi:10.3389/fimmu.2020.00257
- Fujii K, Sakamoto Y, Masaki A, Murase T, Tashiro Y, Yonekura K, Utsunomiya A, Ito A, Kusumoto S, Iida S, Ueda R, Ishida T, Inagaki H: Immunohistochemistry for CCR4 C-terminus predicts CCR4 mutations and mogamulizumab efficacy in adult T-cell leukemia/lymphoma. J Pathol Clin Res. 2021 Jan;7(1):52-60. doi: 10.1002/cjp2.180. Epub 2020 Oct 6. (2020)
- Imaizumi Y, Iwanaga M, Nosaka K, Ishitsuka K, Ishizawa K, Ito S, Amano M, Ishida T, Uike N, Utsunomiya A, Ohshima K, Tanaka J, Tokura Y, Tobinai K, Watanabe T, Uchimaru K, Tsukasaki K; for collaborative: Prognosis of patients with adult T-cell leukemia/lymphoma in Japan: A nationwide hospital-based study. Cancer Sci. 2020 Dec;111(12):4567-4580. doi: 10.1111/cas.14658. Epub 2020 Oct 21. (2020)
- Masaki A, Ishida T, Maeda Y, Ito A, Suzuki S, Narita T, Kinoshita S, Yoshida T, Ri M, Kusumoto S, Komatsu H, Inagaki H, Ueda R, Choi I, Suehiro Y, Iida S: Clinical significance of tryptophan catabolism in follicular lymphoma. Hematol Oncol. 2020 Dec;38(5):742-753. doi: 10.1002/hon.2804. Epub 2020 Sep 29. (2020)
- Sakamoto Y, Ishida T, Masaki A, Takeshita M, Iwasaki H, Yonekura K, Tashiro Y, Ito A, Kusumoto S, Utsunomiya A, Iida S, Ueda R, Inagaki H: Clinical significance of CD28 gene-related activating alterations in adult T-cell leukaemia/lymphoma. Br J Haematol. 2021 Jan;192(2):281-291. doi: 10.1111/bjh.17211. Epub 2020 Nov 18. (2020)
- Yonekura K, Kusumoto S, Choi I, Nakano N, Ito A, Suehiro Y, Imaizumi Y, Yoshimitsu M, Nosaka K, Ohtsuka E, Hidaka M, Jo T, Sasaki H, Moriuchi Y, Ogata M, Tatetsu H, Ishitsuka K, Miyazaki Y, Ueda R, Utsunomiya A, Ishida T: Mogamulizumab for adult T-cell leukemia-lymphoma: a multicenter prospective observational study. Blood Adv. 2020 Oct 27;4(20):5133-5145. doi: 10.1182/bloodadvances.2020003053. (2020)
- Totani H, Shinjo K, Suzuki M, Katsushima K, Mase S, Masaki A, Ito A, Ri M, Kusumoto S, Komatsu H, Ishida T, Inagaki H, Iida S, Kondo Y: Autocrine HGF/c-Met signaling pathway confers aggressiveness in lymph node adult T-cell leukemia/lymphoma. Oncogene. 2020 Aug;39(35):5782-5794. doi: 10.1038/s41388-020-01393-x. Epub 2020 Aug 4. (2020)
- Saito M, Ishii T, Urakawa I, Matsumoto A, Masaki A, Ito A, Kusumoto S, Suzuki S, Takahashi T, Morita A, Inagaki H, Iida S, Ishida T: Robust CD8+ T-cell proliferation and diversification after mogamulizumab in patients with adult T-cell leukemia-lymphoma. Blood Adv. 2020 May 26;4(10):2180-2191. doi: 10.1182/bloodadvances.2020001641. (2020)
- Shu S, Wu HJ, Ge JY, Zeid R, Harris IS, Jovanović B, Murphy K, Wang B, Qiu X, Endress JE, Reyes J, Lim K, Font-Tello A, Syamala S, Xiao T, Reddy Chilamakuri CS, Papachristou EK, D'Santos C, Anand J, Hinohara K, Li W, McDonald TO, Luoma A, Modiste RJ, Nguyen QD, Michel B, Cejas P, Kadoch C, Jaffe JD, Wucherpfennig KW, Qi J, Liu XS, Long H, Brown M, Carroll JS, Brugge JS, Bradner J, Michor F, Polyak K: Synthetic Lethal and Resistance Interactions with BET Bromodomain Inhibitors in Triple-Negative Breast Cancer. Mol Cell. 2020 Jun 18;78(6):1096-1113.e8. Epub 2020 May 15. (2020)
- Seo W, Shimizu K, Kojo S, Okeke A, Kohwi-Shigematsu T, Fujii SI, Taniuchi I: Runx-mediated regulation of CCL5 via antagonizing two enhancers influences immune cell function and anti-tumor immunity. Nat Commun. 2020 Mar 26;11(1):1562. doi: 10.1038/s41467-020-15375-w. (2020)
- Kojo S, Ohno-Oishi M, Wada H, Nieke S, Seo W, Muroi S, Taniuchi I: Constitutive CD8 expression drives innate CD8+ T-cell differentiation via induction of iNKT2 cells. Life Sci Alliance. 2020 Jan 24;3(2):e202000642. doi: 10.26508/lsa.202000642. Print 2020 Feb (2020)
- Seo W, Taniuchi I: The Roles of RUNX Family Proteins in Development of Immune Cells. Mol Cells. 2020 Feb 29;43(2):107-113. doi: 10.14348/molcells.2019.0291. (2020)
- Tenno M, Wong AYW, Ikegaya M, Miyauchi E, Seo W, See P, Kato T, Taida T, Ohno-Oishi M, Ohno H, Yoshida H, Ginhoux F, Taniuchi I: Essential functions of Runx/Cbfβ in gut conventional dendritic cells for priming Rorγt + T cells. Life Sci Alliance. 2019 Dec 9;3(1):e201900441. doi: 10.26508/lsa.201900441. Print 2020 Jan. (2020)
- Kato S, Weng QY, Insco ML, Chen KY, Muralidhar S, Poźniak J, Diaz JM Drier Y, Nguyen N, Lo JA, van Rooijen E, Kemeny LV, Zhan Y, Feng Y, Silkworth W, Powell CT, Liau BB, Xiong Y, Jin J, Newton-Bishop J, Zon LI, Bernstein BE, Fisher DE: Gain-of-function genetic alterations of G9a drive oncogenesis. Cancer Discovery. 2020 Jul;10(7):980-997. doi: 10.1158/2159-8290.CD-19-0532. Epub 2020 Apr (2020)
2019
- Tokunaga A, Sugiyama D, Maeda Y, Warner AB, Panageas KS, Ito S, Togashi Y, Sakai C, Wolchok JD, Nishikawa H: Selective inhibition of low-affinity memory CD8+ T cells by corticosteroids. J Exp Med. 216(12):2701-2713 2019.
- Kamada T, Togashi Y, Tay C, Ha D, Sasaki A, Nakamura Y, Sato E, Fukuoka S, Tada Y, Tanaka A, Morikawa H, Kawazoe A, Kinoshita T, Shitara K, Sakaguchi S, Nishikawa H.: PD-1+ regulatory T cells amplified by PD-1 blockade promote hyperprogression of cancer. Proc Natl Acad Sci USA. 116 (20):9999-10008 2019.
- Tanegashima T, Togashi Y, Azuma K, Kawahara A, Ideguchi K, Sugiyama D, Kinoshita F, Akiba J, Kashiwagi E, Takeuchi A, Irie T, Tatsugami K, Hoshino T, Eto M. Nishikawa H.: Immune suppression by PD-L2 against spontaneous and treatment-related antitumor immunity. Clin Cancer Res. 25(15):4808-4819 2019.
- Togashi Y, Shitara K, Nishikawa H.: Regulatory T cells in cancer immunosuppression - Implications for anticancer therapy. Nat Rev Clin Oncol. 16(6):356-371 2019.
- Ohue Y, Nishikawa H.: Regulatory T (Treg) cells in cancer: can Treg cells be a new therapeutic target? Cancer Sci. 110(7):2080-2089 2019.
- Kochin V, Nishikawa H.: Meddling with meddlers: curbing regulatory T cells and augmenting antitumor immunity. Nagoya J Med Sci. 81(1):1-18 2019.
- Datta M, Coussens LM, Nishikawa H, Hodi FS, Jain RK.: R Reprogramming the Tumor Microenvironment to Improve Immunotherapy: Emerging Strategies and Combination Therapies. Am Soc Clin Oncol Educ Book. Jan; 39:165-174 2019.
- Doi T, Muro K, Ishii H, Kato T, Tsushima T, Takenoyama M, Oizumi S, Gemmoto K, Suna H, Enokitani K, Kawakami T, Nishikawa H, Yamamoto N.: A phase 1 study of the anti-CC chemokine receptor 4 antibody, mogamulizumab, in combination with nivolumab in patients with advanced or metastatic solid tumors. Clin Cancer Res. 25(22):6614-6622. 2019.
- Ha D, Tanaka A, Kibayashi T, Tanemura A, Sugiyama D, Wing JB, Lim EL, Teng KWW, Adeegbe D, Newell EW, Katayama I, Nishikawa H, Sakaguchi S.: Differential control of human Treg and effector T cells in tumor immunity by Fc-engineered anti-CTLA-4 antibody. Proc Natl Acad Sci USA. 116(2):609-618 2019.
- Minoura K, Abe K, Maeda Y, Nishikawa H, Shimamura T.: Model-based cell clustering and population tracking for time-series flow cytometry data. BMC Bioinformatics. Dec 27;20(Suppl 23):633 2019
- Inozume T, Yaguchi T, Ariyasu R, Togashi Y, Ohnuma T, Honobe A, Nishikawa H, Kawakami Y, Kawamura T: Analysis of the Tumor Reactivity of Tumor-Infiltrating Lymphocytes in a Metastatic Melanoma Lesion that Lost Major Histocompatibility Complex Class I Expression after Anti-PD-1 Therapy. J Invest Dermatol. 139(7):1490-1496. 2019.
- Kawazoe A, Shitara K, Kuboki Y, Bando H, Kojima T, Yoshino T, Ohtsu A, Ochiai A, Togashi Y, Nishikawa H, Doi T, Kuwata T.: Clinicopathological features of 22C3 PD-L1 expression with mismatch repair, Epstein-Barr virus status, and cancer genome alterations in metastatic gastric cancer. Gastric Cancer. 22(1):69-76 2019.
- Kataoka K, Miyoshi H, Sakata S, Dobashi A, Couronné L, Kogure Y, Sato Y, Nishida K, Gion Y, Shiraishi Y, Tanaka H, Chiba K, Watatani Y, Kakiuchi N, Shiozawa Y, Yoshizato T, Yoshida K, Makishima H, Sanada M, Onozawa M, Teshima T, Yoshiki Y, Ishida T, Suzuki K, Shimada K, Tomita A, Kato M, Ota Y, Izutsu K, Demachi-Okamura A, Akatsuka Y, Miyano S, Yoshino T, Gaulard P, Hermine O, Takeuchi K, Ohshima K, Ogawa S: Frequent structural variations involving programmed death ligands in Epstein-Barr virus-associated lymphomas. Leukemia. 2019 Jul;33(7):1687-1699. doi: 10.1038/s41375-019-0380-5. Epub 2019 Jan 25.
- Akatsuka Y. [Progress in immune checkpoint inhibitor therapies]: Rinsho Ketsueki. 2019;60(9):1341-1350. Japanese. doi: 10.11406/rinketsu.60.1341.
- Yoshida T, Ri M, Fujinami H, Oshima Y, Tachita T, Marumo Y, Sasaki H, Kinoshita S, Totani H, Narita T, Masaki A, Ito A, Kusumoto S, Ishida T, Komatsu H, Iida S: Impact of chromosomal abnormalities on the efficacy of lenalidomide plus dexamethasone treatment in patients with relapsed/refractory multiple myeloma. Int J Hematol. 2019 Aug;110(2):228-236. doi: 10.1007/s12185-019-02669-z. Epub 2019 May 22. (2019)
- Sakamoto Y, Fujii K, Murase S, Nakano S, Masaki A, Murase T, Kusumoto S, Iida S, Utsunomiya A, Ueda R, Ishida T, Inagaki H: CCR4 is rarely expressed in CCR4-mutated T/NK-cell lymphomas other than adult T-cell leukemia/lymphoma. Int J Hematol. 2019 Oct;110(4):389-392. doi: 10.1007/s12185-019-02728-5. Epub 2019 Aug 29. (2019)
- Suzuki Y, Saito M, Ishii T, Urakawa I, Matsumoto A, Masaki A, Ito A, Kusumoto S, Suzuki S, Hiura M, Takahashi T, Morita A, Inagaki H, Iida S, Ishida T: Mogamulizumab Treatment Elicits Autoantibodies Attacking the Skin in Patients with Adult T-Cell Leukemia-Lymphoma. Clin Cancer Res. 2019 Jul 15;25(14):4388-4399. doi: 10.1158/1078-0432.CCR-18-2575. Epub 2019 Apr 24 (2019)
- Sasaki H, Mitani S, Kusumoto S, Marumo Y, Asano A, Yoshida T, Narita T, Ito A, Yano H, Ri M, Ishida T, Komatsu H, Iida S: Pre- and post-transplant ponatinib for a patient with acute megakaryoblastic blast phase chronic myeloid leukemia with T315I mutation who underwent allogeneic hematopoietic stem cell transplantation. Int J Hematol. 2019 Jul;110(1):119-123. doi: 10.1007/s12185-019-02628-8. Epub 2019 Mar 16. (2019)
- Ding L, Su Y, Fassl A, Hinohara K, Qiu X, Harper NW, Huh SJ, Bloushtain-Qimron N, Jovanović B, Ekram M, Zi X, Hines WC, Alečković M, Gil Del Alcazar C, Caulfield RJ, Bonal DM, Nguyen QD, Merino VF, Choudhury S, Ethington G, Panos L, Grant M, Herlihy W, Au A, Rosson GD, Argani P, Richardson AL, Dillon D, Allred DC, Babski K, Kim EMH, McDonnell CH 3rd, Wagner J, Rowberry R, Bobolis K, Kleer CG, Hwang ES, Blum JL, Cristea S, Sicinski P, Fan R, Long HW, Sukumar S, Park SY, Garber JE, Bissell M, Yao J, Polyak K: Perturbed myoepithelial cell differentiation in BRCA mutation carriers and in ductal carcinoma in situ. Nat Commun. 2019 Sep 13;10(1):4182. (2019)
- An J, Naruse TK, Hinohara K, Soejima Y, Sawabe M, Nakagawa Y, Kuwahara K, Kimura A: MRTF-A regulates proliferation and survival properties of pro-atherogenic macrophages. J Mol Cell Cardiol. 2019 Aug;133:26-35. Epub 2019 May 22. (2019)
- Hinohara K, Polyak K: Intratumoral Heterogeneity: More Than Just Mutations. Trends Cell Biol. 2019 Jul;29(7):569-579. Epub 2019 Apr 12. (2019)
- Ding L, Shunkwiler LB, Harper NW, Zhao Y, Hinohara K, Huh SJ, Ekram MB, Guz J, Kern MJ, Awgulewitsch A, Shull JD, Smits BMG, Polyak K: Deletion of Cdkn1b in ACI rats leads to increased proliferation and pregnancy-associated changes in the mammary gland due to perturbed systemic endocrine environment. PLoS Genet. 2019 Mar 20;15(3):e1008002. eCollection 2019 Mar. (2019)
- Yamamoto M, Jin C, Hata T, Yasumizu Y, Zhang Y, Hong D, Maeda T, Miyo M, Hiraki M, Suzuki Y, Hinohara K, Rajabi H, Kufe D: MUC1-C Integrates Chromatin Remodeling and PARP1 Activity in the DNA Damage Response of Triple-Negative Breast Cancer Cells. Cancer Res. 2019 Apr 15;79(8):2031-2041. Epub 2019 Mar 1. (2019)
- Hinohara K, Wu HJ, Sébastien Vigneau, McDonald TO, Igarashi KJ, Yamamoto KN, Madsen T, Fassl A, Egri SB, Papanastasiou M, Ding L, Peluffo G, Cohen O, Kales SC, Lal-Nag M, Rai G, Maloney DJ, Jadhav A, Simeonov A, Wagle N, Brown M, Meissner A, Sicinski P, Jaffe JD, Jeselsohn R, Gimelbrant AA, Michor F, Polyak K: KDM5 Histone Demethylase Activity Links Cellular Transcriptomic Heterogeneity to Therapeutic Resistance. Cancer Cell. 2019 Feb 11;35(2):330-332. (2019)
- Seo W, Taniuchi I. Too much can be as bad as too little. Nat Immunol. 2019 Oct;20(10):1262-1264. doi: 10.1038/s41590-019-0498-7. (2019)
- Hongo A, Kanaseki T, Tokita S, Kochin V, Miyamoto S, Hashino Y, Codd A, Kawai N, Nakatsugawa M, Hirohashi Y, Sato N, Torigoe T: Upstream Position of Proline Defines Peptide-HLA Class I Repertoire Formation and CD8+ T Cell Responses. J Immunol. 2019 May 15;202(10):2849-2855. doi: 10.4049/jimmunol.1900029. Epub 2019 Apr 1. (2019)
- Xu X, Eshima S, Kato S, Fisher DE, Sakurai H, Hayakawa Y, Yokoyama S: Rational Combination Therapy for Melanoma with Dinaciclib by Targeting BAK-dependent Cell Death. Mol Cancer Ther. 2020 Feb;19(2):627-636. doi: 10.1158/1535-7163.MCT-19-0451. Epub 2019 Nov 19 (2019)
2018
- Tada Y, Togashi Y, Kotani D, Kuwata T, Sato E, Kawazoe A, Doi T, Wada H, Nishikawa H, Shitara K: Targeting VEGFR2 with Ramucirumab strongly impacts effector/activated regulatory T cells and CD8+ T cells in the tumor microenvironment. J. ImmunoTher Cancer 6(1):106 2018.
- Takeuchi Y, Tanemura A, Tada Y, Katayama I, Kumanogoh A, Nishikawa H.: Clinical response to PD-1 blockade correlates with a sub-fraction of peripheral central memory CD4+ T cells in patients with malignant melanoma. Int Immunol. 30(1):13-22 2018.
- Shitara K, Nishikawa H.: Regulatory T cells: a potential target in cancer immunotherapy. Ann NY Acad Sci. 1417 (1):104-115 2018.
- Ueda T, Aokage K, Mimaki S, Tane K, Miyoshi T, Sugano M, Kojima M, Fujii S, Kuwata T, Ochiai A, Kusumoto M, Suzuki K, Tsuchihara K, Nishikawa H, Goto K, Tsuboi M, Ishii G.: Characterization of the tumor immune-microenvironment of lung adenocarcinoma associated with usual interstitial pneumonia. Lung Cancer. 126:162-169 2018.
- Takahashi N, Nishiwaki K, Nakaseko C, Aotsuka N, Sano K, Ohwada C, Kuroki J, Kimura H, Tokuhira M, Mitani K, Fujikawa K, Iwase O, Ohishi K, Kimura F, Fukuda T, Tanosaki S, Takahashi S, Kameoka Y, Nishikawa H, Wakita H.: Treatment-free remission after two-year consolidation therapy with nilotinib in patients with chronic myeloid leukemia: STAT2 trial in Japan. Haematologica. 103(11):1835-1842. 2018.
- Shitaoka K, Hamana H, Kishi H, Hayakawa Y, Kobayashi E, Sukegawa K, Piao X, Lyu F, Nagata T, Sugiyama D, Nishikawa H, Tanemura A, Katayama I, Murahashi M, Takamatsu Y, Tani K, Ozawa T, Muraguchi A.: Identification of Tumoricidal TCRs from Tumor-Infiltrating Lymphocytes by Single-Cell Analysis. Cancer Immunol Res. 6 (4):378-388 2018.
- Ueda T, Aokage K, Nishikawa H, Neri S, Nakamura H, Sugano M, Tane K, Miyoshi T, Kojima M, Fujii S, Kuwata T, Ochiai A, Kusumoto M, Suzuki K, Tsuboi M, Ishii G.: Clinical response to PD-1 blockade correlates with a sub-fraction ofripheral central memory CD4+ T cells in patients with malignant melanoma. J Cancer Res Clin Oncol. 44 (5):835-844 2018.
- Ohta R, Demachi-Okamura A, Akatsuka Y, Fujiwara H, Kuzushima K: Improving TCR affinity on 293T cells. J Immunol Methods. 2019 Mar;466:1-8. doi: 10.1016/j.jim.2018.11.010. Epub 2018 Nov 22.
- Matsuura H, Akatsuka Y, Matsuno T, Sugiura Y, Arakawa S, Oikawa S, Yoshida J, Kosugi M, Emi N: Comparison of the tube test and column agglutination techniques for anti-A/-B antibody titration in healthy individuals. Vox Sang. 2018 Nov;113(8):787-794. doi: 10.1111/vox.12713. Epub 2018 Sep 24.
- Akahori Y, Wang L, Yoneyama M, Seo N, Okumura S, Miyahara Y, Amaishi Y, Okamoto S, Mineno J, Ikeda H, Maki T, Fujiwara H, Akatsuka Y, Kato T, Shiku H: Antitumor activity of CAR-T cells targeting the intracellular oncoprotein WT1 can be enhanced by vaccination. Blood. 2018 Sep 13;132(11):1134-1145. doi: 10.1182/blood-2017-08-802926. Epub 2018 Jul 25.
- Espinoza JL, Elbadry MI, Chonabayashi K, Yoshida Y, Katagiri T, Harada K, Nakagawa N, Zaimoku Y, Imi T, Takamatsu H, Ozawa T, Maruyama H, Hassanein HA, Khalifa A Noreldin A, Takenaka K, Akashi K, Hamana H, Kishi H, Akatsuka Y, Nakao S: Hematopoiesis by iPSC-derived hematopoietic stem cells of aplastic anemia that escape cytotoxic T-cell attack. Blood Adv. 2018 Feb 27;2(4):390-400. doi: 10.1182/bloodadvances.2017013342.
- Kinoshita S, Ishida T, Ito A, Narita T, Masaki A, Suzuki S, Yoshida T, Ri M, Kusumoto S, Komatsu H, Shimizu N, Inagaki H, Kuroda T, Scholz A, Ueda R, Sanda T, Iida S: Cyclin-dependent kinase 9 as a potential specific molecular target in NK-cell leukemia/lymphoma. Haematologica. 2018 Dec;103(12):2059-2068. doi: 10.3324/haematol.2018.191395. Epub 2018 Aug 3. (2018)
- Sakamoto Y, Ishida T, Masaki A, Murase T, Yonekura K, Tashiro Y, Tokunaga M, Utsunomiya A, Ito A, Kusumoto S, Iida S, Ueda R, Inagaki H: CCR4 mutations associated with superior outcome of adult T-cell leukemia/lymphoma under mogamulizumab treatment. Blood. 2018 Aug 16;132(7):758-761. doi: 10.1182/blood-2018-02-835991. Epub 2018 Jun 21. (2018)
- Ishitsuka K, Utsunomiya A, Ishida T: PD-1 Inhibitor Therapy in Adult T-Cell Leukemia–Lymphoma. N Engl J Med. 2018 Aug 16;379(7):695. doi: 10.1056/NEJMc1807852. (2018)
- Masaki A, Ishida T, Suzuki S, Ito A, Narita T, Kinoshita S, Ri M, Kusumoto S, Komatsu H, Inagaki H, Ueda R, Iida S: Human T-cell lymphotropic/leukemia virus type 1 (HTLV-1) Tax-specific T-cell exhaustion in HTLV-1-infected individuals. Cancer Sci. 2018 Aug;109(8):2383-2390. doi: 10.1111/cas.13654. Epub 2018 Jun 27. (2018)
- Yoshida T, Ri M, Kinoshita S, Narita T, Totani H, Ashour R, Ito A, Kusumoto S, Ishida T, Komatsu H, Iida S: Low expression of neural cell adhesion molecule, CD56, is associated with low efficacy of bortezomib plus dexamethasone therapy in multiple myeloma. PLoS One. 2018 May 8;13(5):e0196780. doi: 10.1371/journal.pone.0196780. eCollection 2018. (2018)
- Kinoshita S, Ri M, Kanamori T, Aoki S, Yoshida T, Narita T, Totani H, Ito A, Kusumoto S, Ishida T, Komatsu H, Iida S: Potent antitumor effect of combination therapy with sub-optimal doses of Akt inhibitors and pomalidomide plus dexamethasone in multiple myeloma. Oncol Lett. 2018 Jun;15(6):9450-9456. doi: 10.3892/ol.2018.8501. Epub 2018 Apr 16. (2018)
- Kanamori T, Kusumoto S, Okita K, Hagiwara S, Kato C, Nakashima T, Murakami S, Narita T, Ito A, Ri M, Ishida T, Komatsu H, Matsukawa N, Iida S: [Sporadic late-onset nemaline myopathy with monoclonal gammopathy of undetermined significance mimicking POEMS syndrome]. Rinsho Ketsueki. 2018;59(2):161-166. doi: 10.11406/rinketsu.59.161. (2018)
- Ishida T, Jo T, Takemoto S, Suzushima H, Suehiro Y, Choi I, Yoshimitsu M, Saburi Y, Nosaka K, Utsunomiya A, Kobayashi Y, Yamamoto K, Fujiwara H, Ishitsuka K, Yoshida S, Taira N, Imada K, Kato K, Moriuchi Y, Yoshimura K, Takahashi T, Tobinai K, Ueda R: Follow-up of a randomised phase II study of chemotherapy alone or in combination with mogamulizumab in newly diagnosed aggressive adult T-cell leukaemia-lymphoma: impact on allogeneic haematopoietic stem cell transplantation. Br J Haematol. 2019 Feb;184(3):479-483. doi: 10.1111/bjh.15123. Epub 2018 Feb 7. (2018)
- Yoshida T, Ri M, Kanamori T, Aoki S, Ashour R, Kinoshita S, Narita T, Totani H, Masaki A, Ito A, Kusumoto S, Ishida T, Komatsu H, Kitahata S, Chiba T, Ichikawa S, Iida S: Potent anti-tumor activity of a syringolin analog in multiple myeloma: a dual inhibitor of proteasome activity targeting β2 and β5 subunits. Oncotarget. 2018 Jan 11;9(11):9975-9991. doi: 10.18632/oncotarget.24160. eCollection 2018 Feb 9. (2018)
- Aiki S, Okuyama T, Sugano K, Kubota Y, Imai F, Nishioka M, Ito Y, Iida S, Komatsu H, Ishida T, Kusumoto S, Akechi T: Cognitive dysfunction among newly diagnosed older patients with hematological malignancy: frequency, clinical indicators and predictors. Jpn J Clin Oncol. 2018 Jan 1;48(1):61-67. doi: 10.1093/jjco/hyx159. (2018)
- Xing S, Shao P, Li F, Zhao X, Seo W, Wheat JC, Ramasamy S, Wang J, Li X, Peng W, Yu S, Liu C, Taniuchi I, Sweetser DA, Xue HH: Tle corepressors are differentially partitioned to instruct CD8+ T cell lineage choice and identity. J Exp Med. 2018 Aug 6;215(8):2211-2226. doi: 10.1084/jem.20171514. Epub 2018 Jul 25. (2018)
- Kim KH, Ree JH, Kim Y, Kim S, Kang SY, Seo W: Assessing whether the 2017 Mw 5.4 Pohang earthquake in South Korea was an induced event. Science. 2018 Jun 1;360(6392):1007-1009. doi: 10.1126/science.aat6081. Epub 2018 Apr 26. (2018)
- Sasaki H, Mitani S, Kusumoto S, Marumo Y, Asano A, Yoshida T, Narita T, Ito A, Yano H, Ri M, Ishida T, Komatsu H, Iida S: Pre- and post-transplant ponatinib for a patient with acute megakaryoblastic blast phase chronic myeloid leukemia with T315I mutation who underwent allogeneic hematopoietic stem cell transplantation. Int J Hematol. 2019 Jul;110(1):119-123. doi: 10.1007/s12185-019-02628-8. Epub 2019 Mar 16.
- Ishida T, Jo T, Takemoto S, Suzushima H, Suehiro Y, Choi I, Yoshimitsu M, Saburi Y, Nosaka K, Utsunomiya A, Kobayashi Y, Yamamoto K, Fujiwara H, Ishitsuka K, Yoshida S, Taira N, Imada K, Kato K, Moriuchi Y, Yoshimura K, Takahashi T, Tobinai K, Ueda R: Follow-up of a randomised phase II study of chemotherapy alone or in combination with mogamulizumab in newly diagnosed aggressive adult T-cell leukaemia-lymphoma: impact on allogeneic haematopoietic stem cell transplantation. Br J Haematol. 2019 Feb;184(3):479-483. doi: 10.1111/bjh.15123. Epub 2018 Feb 7.
- Kinoshita S, Ishida T, Ito A, Narita T, Masaki A, Suzuki S, Yoshida T, Ri M, Kusumoto S, Komatsu H, Shimizu N, Inagaki H, Kuroda T, Scholz A, Ueda R, Sanda T, Iida S: Cyclin-dependent kinase 9 as a potential specific molecular target in NK-cell leukemia/lymphoma. Haematologica. 2018 Dec;103(12):2059-2068. doi: 10.3324/haematol.2018.191395. Epub 2018 Aug 3.
- Sakamoto Y, Ishida T, Masaki A, Murase T, Yonekura K, Tashiro Y, Tokunaga M, Utsunomiya A, Ito A, Kusumoto S, Iida S, Ueda R, Inagaki H: CCR4 mutations associated with superior outcome of adult T-cell leukemia/lymphoma under mogamulizumab treatment. Blood. 2018 Aug 16;132(7):758-761. doi: 10.1182/blood-2018-02-835991. Epub 2018 Jun 21.
- Ishitsuka K, Utsunomiya A, Ishida T: PD-1 Inhibitor Therapy in Adult T-Cell Leukemia–Lymphoma. N Engl J Med. 2018 Aug 16;379(7):695. doi: 10.1056/NEJMc1807852.
- Masaki A, Ishida T, Suzuki S, Ito A, Narita T, Kinoshita S, Ri M, Kusumoto S, Komatsu H, Inagaki H, Ueda R, Iida S: Human T-cell lymphotropic/leukemia virus type 1 (HTLV-1) Tax-specific T-cell exhaustion in HTLV-1-infected individuals. Cancer Sci. 2018 Aug;109(8):2383-2390. doi: 10.1111/cas.13654. Epub 2018 Jun 27.
- Yoshida T, Ri M, Kinoshita S, Narita T, Totani H, Ashour R, Ito A, Kusumoto S, Ishida T, Komatsu H, Iida S.: Low expression of neural cell adhesion molecule, CD56, is associated with low efficacy of bortezomib plus dexamethasone therapy in multiple myeloma. PLoS One. 2018 May 8;13(5):e0196780. doi: 10.1371/journal.pone.0196780. eCollection 2018.
- Kinoshita S, Ri M, Kanamori T, Aoki S, Yoshida T, Narita T, Totani H, Ito A, Kusumoto S, Ishida T, Komatsu H, Iida S: Potent antitumor effect of combination therapy with sub-optimal doses of Akt inhibitors and pomalidomide plus dexamethasone in multiple myeloma. Oncol Lett. 2018 Jun;15(6):9450-9456. doi: 10.3892/ol.2018.8501. Epub 2018 Apr 16.
- Kanamori T, Kusumoto S, Okita K, Hagiwara S, Kato C, Nakashima T, Murakami S, Narita T, Ito A, Ri M, Ishida T, Komatsu H, Matsukawa N, Iida S.: [Sporadic late-onset nemaline myopathy with monoclonal gammopathy of undetermined significance mimicking POEMS syndrome]. Rinsho Ketsueki. 2018;59(2):161-166. doi: 10.11406/rinketsu.59.161.
- Hinohara K, Wu HJ, Vigneau S, McDonald TO, Igarashi KJ, Yamamoto KN, Madsen T, Fassl A, Egri SB, Papanastasiou M, Ding L, Peluffo G, Cohen O, Kales SC, Lal-Nag M, Rai G, Maloney DJ, Jadhav A, Simeonov A, Wagle N, Brown M, Meissner A, Sicinski P, Jaffe JD, Jeselsohn R, Gimelbrant AA, Michor F, Polyak K: KDM5 Histone Demethylase Activity Links Cellular Transcriptomic Heterogeneity to Therapeutic Resistance. Cancer Cell. 2018 Dec 10;34(6):939-953.e9. Epub 2018 Nov 21. (2018)
- Ben-David U, Siranosian B, Ha G, Tang H, Oren Y, Hinohara K, Strathdee CA, Dempster J, Lyons NJ, Burns R, Nag A, Kugener G, Cimini B, Tsvetkov P, Maruvka YE, O'Rourke R, Garrity A, Tubelli AA, Bandopadhayay P, Tsherniak A, Vazquez F, Wong B, Birger C, Ghandi M, Thorner AR, Bittker JA, Meyerson M, Getz G, Beroukhim R, Golub TR: Genetic and transcriptional evolution alters cancer cell line drug response. Nature. 2018 Aug;560(7718):325-330. Epub 2018 Aug 8. (2018)
- Komura K, Yoshikawa Y, Shimamura T, Chakraborty G, Gerke TA, Hinohara K, Chadalavada K, Jeong SH, Armenia J, Du SY, Mazzu YZ, Taniguchi K, Ibuki N, Meyer CA, Nanjangud GJ, Inamoto T, Lee GM, Mucci LA, Azuma H, Sweeney CJ, Kantoff PW: ATR inhibition controls aggressive prostate tumors deficient in Y-linked histone demethylase KDM5D. J Clin Invest. 2018 Jul 2;128(7):2979-2995. Epub 2018 Jun 4. (2018)
- Miyamoto S, Kochin V, Kanaseki T, Hongo A, Tokita S, Kikuchi Y, Takaya A, Hirohashi Y, Tsukahara T, Terui T, Ishitani K, Hata F, Takemasa I, Miyazaki A, Hiratsuka H, Sato N, Torigoe T: The Antigen ASB4 on Cancer Stem Cells Serves as a Target for CTL Immunotherapy of Colorectal Cancer. Cancer Immunol Res. 2018 Mar;6(3):358-369. doi: 10.1158/2326-6066.CIR-17-0518. Epub 2018 Jan 25. (2018)
- Watanabe K, Yokoyama S, Kaneto N, Hori T, Iwakami Y, Kato S, Hayakawa Y, Sakurai H, Fukuoka J, Saiki I: COPS9 signalosome subunit 5 regulates cancer metastasis by deubiquitinating SNAIL. Oncotarget. 2018 Apr 17;9(29):20670-20680. doi: 10.18632/oncotarget.25060. (2018)
2017
- Nosaka K, Iwanaga M, Imaizumi Y, Ishitsuka K, Ishizawa K, Ishida Y, Amano M, Ishida T, Uike N, Utsunomiya A, Ohshima K, Kawai K, Tanaka J, Tokura Y, Tobinai K, Watanabe T, Uchimaru K, Tsukasaki K. Epidemiological and clinical features of adult T-cell leukemia-lymphoma in Japan, 2010-2011: A nationwide survey. Cancer Sci. 2017 Dec;108(12):2478-2486. doi: 10.1111/cas.13398. Epub 2017 Oct 8. (2017)
- Wong RWJ, Ngoc PCT, Leong WZ, Yam AWY, Zhang T, Asamitsu K, Iida S, Okamoto T, Ueda R, Gray NS, Ishida T, Sanda T: Enhancer profiling identifies critical cancer genes and characterizes cell identity in adult T-cell leukemia. Blood. 2017 Nov 23;130(21):2326-2338. doi: 10.1182/blood-2017-06-792184. Epub 2017 Oct 4. (2017)
- Kharfan-Dabaja MA, Kumar A, Ayala E, Hamadani M, Reimer P, Gisselbrecht C, d'Amore F, Jantunen E, Ishida T, Bazarbachi A, Foss F, Advani R, Fenske TS, Lazarus HM, Friedberg JW, Aljurf M, Sokol L, Tobinai K, Tse E, Burns LJ, Chavez JC, Reddy NM, Suzuki R, Ahmed S, Nademanee A, Mohty M, Gopal AK, Fanale MA, Pro B, Moskowitz AJ, Sureda A, Perales MA, Carpenter PA, Savani BN: Clinical Practice Recommendations on Indication and Timing of Hematopoietic Cell Transplantation in Mature T Cell and NK/T Cell Lymphomas: An International Collaborative Effort on Behalf of the Guidelines Committee of the American Society for Blood and Marrow Transplantation. Biol Blood Marrow Transplant. 2017 Nov;23(11):1826-1838. doi: 10.1016/j.bbmt.2017.07.027. Epub 2017 Aug 7. (2017)
- Maruyama D, Tobinai K, Ogura M, Uchida T, Hatake K, Taniwaki M, Ando K, Tsukasaki K, Ishida T, Kobayashi N, Ishizawa K, Tatsumi Y, Kato K, Kiguchi T, Ikezoe T, Laille E, Ro T, Tamakoshi H, Sakurai S, Ohtsu T: Romidepsin in Japanese patients with relapsed or refractory peripheral T-cell lymphoma: a phase I/II and pharmacokinetics study. Int J Hematol. 2017 Nov;106(5):655-665. doi: 10.1007/s12185-017-2286-1. Epub 2017 Jun 29.
- Ishida T, Utsunomiya A, Jo T, Yamamoto K, Kato K, Yoshida S, Takemoto S, Suzushima H, Kobayashi Y, Imaizumi Y, Yoshimura K, Kawamura K, Takahashi T, Tobinai K, Ueda R: Mogamulizumab for relapsed adult T-cell leukemia-lymphoma: Updated follow-up analysis of phase I and II studies. Cancer Sci. 2017 Oct;108(10):2022-2029. doi: 10.1111/cas.13343. Epub 2017 Aug 28. (2017)
- Yoshida T, Ri M, Kanamori T, Aoki S, Ashour R, Kinoshita S, Narita T, Totani H, Masaki A, Ito A, Kusumoto S, Ishida T, Komatsu H, Kitahata S, Chiba T, Ichikawa S, Iida S: Potent anti-tumor activity of a syringolin analog in multiple myeloma: a dual inhibitor of proteasome activity targeting β2 and β5 subunits. Oncotarget . 2018 Jan 11;9(11):9975-9991. doi: 10.18632/oncotarget.24160. eCollection 2018 Feb 9.
- Aiki S, Okuyama T, Sugano K, Kubota Y, Imai F, Nishioka M, Ito Y, Iida S, Komatsu H, Ishida T, Kusumoto S, Akechi T: Cognitive dysfunction among newly diagnosed older patients with hematological malignancy: frequency, clinical indicators and predictors. Jpn J Clin Oncol. 2018 Jan 1;48(1):61-67. doi: 10.1093/jjco/hyx159.
- Masaki A, Ishida T, Maeda Y, Ito A, Suzuki S, Narita T, Kinoshita S, Takino H, Yoshida T, Ri M, Kusumoto S, Komatsu H, Inagaki H, Ueda R, Choi I, Suehiro Y, Iida S:
- Clinical significance of tryptophan catabolism in Hodgkin lymphoma. Cancer Sci. 2018 Jan;109(1):74-83. doi: 10.1111/cas.13432. Epub 2017 Nov 29.
- Yoshimitsu M, Tanosaki R, Kato K, Ishida T, Choi I, Takatsuka Y, Fukuda T, Eto T, Hidaka M, Uchida N, Miyamoto T, Nakashima Y, Moriuchi Y, Nagafuji K, Miyazaki Y, Ichinohe T, Takanashi M, Atsuta Y, Utsunomiya A, ATL Working Group of the Japan Society for Hematopoietic Cell Transplantation: Risk Assessment in Adult T Cell Leukemia/Lymphoma Treated with Allogeneic Hematopoietic Stem Cell Transplantation Biol Blood Marrow Transplant. 2018 Apr;24(4):832-839. doi: 10.1016/j.bbmt.2017.11.005. Epub 2017 Nov 16.
- Nosaka K, Iwanaga M, Imaizumi Y, Ishitsuka K, Ishizawa K, Ishida Y, Amano M, Ishida T, Uike N, Utsunomiya A, Ohshima K, Kawai K, Tanaka J, Tokura Y, Tobinai K, Watanabe T, Uchimaru K, Tsukasaki K. Epidemiological and clinical features of adult T-cell leukemia-lymphoma in Japan, 2010-2011: A nationwide survey. Cancer Sci. 2017 Dec;108(12):2478-2486. doi: 10.1111/cas.13398. Epub 2017 Oct 8.
- Wong RWJ, Ngoc PCT, Leong WZ, Yam AWY, Zhang T, Asamitsu K, Iida S, Okamoto T, Ueda R, Gray NS, Ishida T, Sanda T: Enhancer profiling identifies critical cancer genes and characterizes cell identity in adult T-cell leukemia. Blood. 2017 Nov 23;130(21):2326-2338. doi: 10.1182/blood-2017-06-792184. Epub 2017 Oct 4.
- Kharfan-Dabaja MA, Kumar A, Ayala E, Hamadani M, Reimer P, Gisselbrecht C, d'Amore F, Jantunen E, Ishida T, Bazarbachi A, Foss F, Advani R, Fenske TS, Lazarus HM, Friedberg JW, Aljurf M, Sokol L, Tobinai K, Tse E, Burns LJ, Chavez JC, Reddy NM, Suzuki R, Ahmed S, Nademanee A, Mohty M, Gopal AK, Fanale MA, Pro B, Moskowitz AJ, Sureda A, Perales MA, Carpenter PA, Savani BN: Clinical Practice Recommendations on Indication and Timing of Hematopoietic Cell Transplantation in Mature T Cell and NK/T Cell Lymphomas: An International Collaborative Effort on Behalf of the Guidelines Committee of the American Society for Blood and Marrow Transplantation. Biol Blood Marrow Transplant. 2017 Nov;23(11):1826-1838. doi: 10.1016/j.bbmt.2017.07.027. Epub 2017 Aug 7.
- Maruyama D, Tobinai K, Ogura M, Uchida T, Hatake K, Taniwaki M, Ando K, Tsukasaki K, Ishida T, Kobayashi N, Ishizawa K, Tatsumi Y, Kato K, Kiguchi T, Ikezoe T, Laille E, Ro T, Tamakoshi H, Sakurai S, Ohtsu T: Romidepsin in Japanese patients with relapsed or refractory peripheral T-cell lymphoma: a phase I/II and pharmacokinetics study. Int J Hematol. 2017 Nov;106(5):655-665. doi: 10.1007/s12185-017-2286-1. Epub 2017 Jun 29.
- Ishida T, Utsunomiya A, Jo T, Yamamoto K, Kato K, Yoshida S, Takemoto S, Suzushima H, Kobayashi Y, Imaizumi Y, Yoshimura K, Kawamura K, Takahashi T, Tobinai K, Ueda R: Mogamulizumab for relapsed adult T-cell leukemia-lymphoma: Updated follow-up analysis of phase I and II studies. Cancer Sci. 2017 Oct;108(10):2022-2029. doi: 10.1111/cas.13343. Epub 2017 Aug 28.
- Maeda T, Hiraki M, Jin C, Rajabi H, Tagde A, Alam M, Bouillez A, Hu X, Suzuki Y, Miyo M, Hata T, Hinohara K, Kufe D: MUC1-C Induces PD-L1 and Immune Evasion in Triple-Negative Breast Cancer. Cancer Res. 2018 Jan 1;78(1):205-215. Epub 2017 Dec 20. (2017)
- Terai H, Kitajima S, Potter DS, Matsui Y, Quiceno LG, Chen T, Kim TJ, Rusan M, Thai TC, Piccioni F, Donovan KA, Kwiatkowski N, Hinohara K, Wei G, Gray NS, Fischer ES, Wong KK, Shimamura T, Letai A, Hammerman PS, Barbie DA: ER Stress Signaling Promotes the Survival of Cancer \\\"Persister Cells\\\" Tolerant to EGFR Tyrosine Kinase Inhibitors. Cancer Res. 2018 Feb 15;78(4):1044-1057. Epub 2017 Dec 19. (2017)
- Kojo S, Tanaka H, Endo TA, Muroi S, Liu Y, Seo W, Tenno M, Kakugawa K, Naoe Y, Nair K, Moro K, Katsuragi Y, Kanai A, Inaba T, Egawa T, Venkatesh B, Minoda A, Kominami R, Taniuchi I: Priming of lineage-specifying genes by Bcl11b is required for lineage choice in post-selection thymocytes. Nat Commun. 2017 Sep 26;8(1):702. doi: 10.1038/s41467-017-00768-1. (2017)
- Kakugawa K, Kojo S, Tanaka H, Seo W, Endo TA, Kitagawa Y, Muroi S, Tenno M, Yasmin N, Kohwi Y, Sakaguchi S, Kowhi-Shigematsu T, Taniuchi I: Essential Roles of SATB1 in Specifying T Lymphocyte Subsets. Cell Rep. 2017 May 9;19(6):1176-1188. doi: 10.1016/j.celrep.2017.04.038. (2017)
- Seo W, Taniuchi I: Regulation of hematopoiesis and immune responses by long non-coding RNAs. Int Immunol. 2017 Apr 1;29(4):165-172. doi: 10.1093/intimm/dxx021. (2017)
- Seo W, Muroi S, Akiyama K, Taniuchi I: Distinct requirement of Runx complexes for TCRβ enhancer activation at distinct developmental stages. Sci Rep. 2017 Feb 2;7:41351. doi: 10.1038/srep41351. (2017)
- Ebihara T, Seo W, Taniuchi I: Roles of RUNX Complexes in Immune Cell Development. Adv Exp Med Biol. 2017;962:395-413. doi: 10.1007/978-981-10-3233-2_24. (2017)
- Tanaka T, Kutomi G, Kajiwara T, Kukita K, Kochin V, Kanaseki T, Tsukahara T, Hirohashi Y, Torigoe T, Okamoto Y, Hirata K, Sato N, Tamura Y: Cancer-associated oxidoreductase ERO1-α promotes immune escape through up-regulation of PD-L1 in human breast cancer. Oncotarget. 2017 Apr 11;8(15):24706-24718. doi: 10.18632/oncotarget.14960. (2017)
- Kochin V, Kanaseki T, Tokita S, Miyamoto S, Shionoya Y, Kikuchi Y, Morooka D, Hirohashi Y, Tsukahara T, Watanabe K, Toji S, Kokai Y, Sato N, Torigoe T: HLA-A24 ligandome analysis of colon and lung cancer cells identifies a novel cancer-testis antigen and a neoantigen that elicits specific and strong CTL responses. Oncoimmunology. 2017 Feb 16;6(4):e1293214. doi: 10.1080/2162402X.2017.1293214. (2017)
- Shionoya Y, Kanaseki T, Miyamoto S, Tokita S, Hongo A, Kikuchi Y, Kochin V, Watanabe K, Horibe R, Saijo H, Tsukahara T, Hirohashi Y, Takahashi H, Sato N, Torigoe T: Loss of tapasin in human lung and colon cancer cells and escape from tumor-associated antigen-specific CTL recognition. Oncoimmunology. 2017 Jan 3;6(2):e1274476. doi: 10.1080/2162402X.2016.1274476. (2017)
2016
- Akane K, Kojima S, Mak TW, Shiku H, Suzuki H. CD8+CD122+CD49dlow regulatory T cells maintain T-cell homeostasis by killing activated T cells via Fas/FasL-mediated cytotoxicity. Proc Natl Acad Sci U S A, 2016;113:2460-2465.
- Haseda F, Imagawa A, Nishikawa H, Mitsui S, Tsutsumi C, Fujisawa R, Sano H, Murase-Mishiba Y, Terasaki J, Sakaguchi S, Hanafusa T. Antibody to CMRF35-Like Molecule 2, CD300e A Novel Biomarker Detected in Patients with Fulminant Type 1 Diabetes. PLoS One, 2016;11:e0160576.
- Hayakawa Y, Kawada M, Nishikawa H, Ochiya T, Saya H, Seimiya H, Yao R, Hayashi M, Kai C, Matsuda A, Naoe T, Ohtsu A, Okazaki T, Saji H, Sata M, Sugimura H, Sugiyama Y, Toi M, Irimura T. Report on the use of non-clinical studies in the regulatory evaluation of oncology drugs. Cancer Sci, 2016;107:189-202.
- Hirohashi Y, Torigoe T, Tsukahara T, Kanaseki T, Kochin V, Sato N. Immune responses to human cancer stem-like cells/cancer-initiating cells. Cancer Sci, 2016;107:12-17.
- Ito N, Kamiguchi K, Nakanishi K, Sokolovskya A, Hirohashi Y, Tamura Y, Murai A, Yamamoto E, Kanaseki T, Tsukahara T, Kochin V, Chiba S, Shimohama S, Sato N, Torigoe T. A novel nuclear DnaJ protein, DNAJC8, can suppress the formation of spinocerebellar ataxia 3 polyglutamine aggregation in a J-domain independent manner. Biochem Biophys Res Commun, 2016;474:626-633.
- Ito S, Tanaka Y, Oshino R, Okado S, Hori M, Isobe KI. GADD34 suppresses lipopolysaccharide-induced sepsis and tissue injury through the regulation of macrophage activation. Cell Death Dis, 2016;7:e2219.
- Kajiwara T, Tanaka T, Kukita K, Kutomi G, Saito K, Okuya K, Takaya A, Kochin V, Kanaseki T, Tsukahara T, Hirohashi Y, Torigoe T, Hirata K, Sato N, Tamura Y. Hypoxia augments MHC class I antigen presentation via facilitation of ERO1-α-mediated oxidative folding in murine tumor cells. Eur J Immunol, 2016.
- Kakihana K, Fujioka Y, Suda W, Najima Y, Kuwata G, Sasajima S, Mimura I, Morita H, Sugiyama D, Nishikawa H, Hattori M, Hino Y, Ikegawa S, Yamamoto K, Toya T, Doki N, Koizumi K, Honda K, Ohashi K. Fecal microbiota transplantation for patients with steroid-resistant/dependent acute graft-versus-host disease of the gut. Blood, 2016.
- Liu L, Ito S, Nishio N, Sun Y, Tanaka Y, Isobe K. GADD34 Promotes Tumor Growth by Inducing Myeloid-derived Suppressor Cells. Anticancer Res, 2016;36:4623-4628.
- Saito T, Nishikawa H, Wada H, Nagano Y, Sugiyama D, Atarashi K, Maeda Y, Hamaguchi M, Ohkura N, Sato E, Nagase H, Nishimura J, Yamamoto H, Takiguchi S, Tanoue T, Suda W, Morita H, Hattori M, Honda K, Mori M, Doki Y, Sakaguchi S. Two FOXP3(+)CD4(+) T cell subpopulations distinctly control the prognosis of colorectal cancers. Nat Med, 2016;22:679-684.
- Sasaki T, Kanaseki T, Shionoya Y, Tokita S, Miyamoto S, Saka E, Kochin V, Takasawa A, Hirohashi Y, Tamura Y, Miyazaki A, Torigoe T, Hiratsuka H, Sato N. Microenvironmental stresses induce HLA-E/Qa-1 surface expression and thereby reduce CD8(+) T-cell recognition of stressed cells. Eur J Immunol, 2016;46:929-940.
- Shimazu Y, Hishizawa M, Hamaguchi M, Nagai Y, Sugino N, Fujii S, Kawahara M, Kadowaki N, Nishikawa H, Sakaguchi S, Takaori-Kondo A. Hypomethylation of the Treg-Specific Demethylated Region in FOXP3 Is a Hallmark of the Regulatory T-cell Subtype in Adult T-cell Leukemia. Cancer Immunol Res, 2016;4:136-145.
- Takeuchi Y, Nishikawa H. Roles of regulatory T cells in cancer immunity. Int Immunol, 2016;28:401-409.
- Tanaka T, Kutomi G, Kajiwara T, Kukita K, Kochin V, Kanaseki T, Tsukahara T, Hirohashi Y, Torigoe T, Okamoto Y, Hirata K, Sato N, Tamura Y. Cancer-associated oxidoreductase ERO1-α drives the production of VEGF via oxidative protein folding and regulating the mRNA level. Br J Cancer, 2016;114:1227-1234.
- Tanaka Y, Ito S, Isobe K. Vancomycin-sensitive bacteria trigger development of colitis-associated colon cancer by attracting neutrophils. Sci Rep, 2016;6:23920.
- Ureshino H, Shindo T, Nishikawa H, Watanabe N, Watanabe E, Satoh N, Kitaura K, Kitamura H, Doi K, Nagase K, Kimura H, Samukawa M, Kusunoki S, Miyahara M, Shin-I T, Suzuki R, Sakaguchi S, Kimura S. Effector Regulatory T Cells Reflect the Equilibrium between Antitumor Immunity and Autoimmunity in Adult T-cell Leukemia. Cancer Immunol Res, 2016;4:644-649.
2015
- Adeegbe DO, Nishikawa H. Regulatory T cells in cancer; can they be controlled? Immunotherapy, 2015;7:843-846.
- Chen N, Nishio N, Ito S, Tanaka Y, Sun Y, Isobe K. Growth arrest and DNA damage-inducible protein (GADD34) enhanced liver inflammation and tumorigenesis in a diethylnitrosamine (DEN)-treated murine model. Cancer Immunol Immunother, 2015;64:777-789.
- Himeno T, Kamiya H, Naruse K, Cheng Z, Ito S, Shibata T, Kondo M, Kato J, Okawa T, Fujiya A, Suzuki H, Kito T, Hamada Y, Oiso Y, Isobe K, Nakamura J. Angioblast Derived from ES Cells Construct Blood Vessels and Ameliorate Diabetic Polyneuropathy in Mice. J Diabetes Res, 2015;2015:257230.
- Hirohashi Y, Torigoe T, Mariya T, Kochin V, Saito T, Sato N. HLA class I as a predictor of clinical prognosis and CTL infiltration as a predictor of chemosensitivity in ovarian cancer. Oncoimmunology, 2015;4:e1005507.
- Ito S, Tanaka Y, Oshino R, Aiba K, Thanasegaran S, Nishio N, Isobe K. GADD34 inhibits activation-induced apoptosis of macrophages through enhancement of autophagy. Sci Rep, 2015;5:8327.
- Kurose K, Ohue Y, Wada H, Iida S, Ishida T, Kojima T, Doi T, Suzuki S, Isobe M, Funakoshi T, Kakimi K, Nishikawa H, Udono H, Oka M, Ueda R, Nakayama E. Phase Ia Study of FoxP3+ CD4 Treg Depletion by Infusion of a Humanized Anti-CCR4 Antibody, KW-0761, in Cancer Patients. Clin Cancer Res, 2015;21:4327-4336.
- Liu L, Ito S, Nishio N, Sun Y, Chen N, Tanaka Y, Isobe K. GADD34 Facilitates Cell Death Resulting from Proteasome Inhibition. Anticancer Res, 2015;35:5317-5324.
- Miyara M, Chader D, Sage E, Sugiyama D, Nishikawa H, Bouvry D, Claër L, Hingorani R, Balderas R, Rohrer J, Warner N, Chapelier A, Valeyre D, Kannagi R, Sakaguchi S, Amoura Z, Gorochov G. Sialyl Lewis x (CD15s) identifies highly differentiated and most suppressive FOXP3high regulatory T cells in humans. Proc Natl Acad Sci U S A, 2015;112:7225-7230.
- Nishikawa H. Overview: New Modality for Cancer Treatment. Oncology, 2015;89 Suppl 1:33-35.
- Okabe M, Ito S, Nishio N, Tanaka Y, Isobe K. Thymic Epithelial Cells Induced from Pluripotent Stem Cells by a Three-Dimensional Spheroid Culture System Regenerates Functional T Cells in Nude Mice. Cell Reprogram, 2015;17:368-375.
- Sun Y, Ito S, Nishio N, Tanaka Y, Chen N, Liu L, Isobe K. Enhancement of the acrolein-induced production of reactive oxygen species and lung injury by GADD34. Oxid Med Cell Longev, 2015;2015:170309.
- Takada K, Van Laethem F, Xing Y, Akane K, Suzuki H, Murata S, Tanaka K, Jameson SC, Singer A, Takahama Y. TCR affinity for thymoproteasome-dependent positively selecting peptides conditions antigen responsiveness in CD8(+) T cells. Nat Immunol, 2015;16:1069-1076.
- Tanaka Y, Ito S, Oshino R, Chen N, Nishio N, Isobe K. Effects of growth arrest and DNA damage-inducible protein 34 (GADD34) on inflammation-induced colon cancer in mice. Br J Cancer, 2015;113:669-679.
- Thanasegaran S, Ito S, Nishio N, Uddin MN, Sun Y, Isobe K. Recruitment of Gr1(+)CD11b (+)F4/80 (+) population in the bone marrow and spleen by irradiation-induced pulmonary damage. Inflammation, 2015;38:465-475.
- Torvaldson E, Kochin V, Eriksson JE. Phosphorylation of lamins determine their structural properties and signaling functions. Nucleus, 2015;6:166-171.
2014
- de Thonel A, Hazoumé A, Kochin V, Isoniemi K, Jego G, Fourmaux E, Hammann A, Mjahed H, Filhol O, Micheau O, Rocchi P, Mezger V, Eriksson JE, Rangnekar VM, Garrido C. Regulation of the proapoptotic functions of prostate apoptosis response-4 (Par-4) by casein kinase 2 in prostate cancer cells. Cell Death Dis, 2014;5:e1016.
- Isobe K, Cheng Z, Nishio N, Suganya T, Tanaka Y, Ito S. iPSCs, aging and age-related diseases. N Biotechnol, 2014;31:411-421.
- Ito T, Yamada S, Tanaka C, Ito S, Murai T, Kobayashi D, Fujii T, Nakayama G, Sugimoto H, Koike M, Nomoto S, Fujiwara M, Kodera Y. Overexpression of L1CAM is associated with tumor progression and prognosis via ERK signaling in gastric cancer. Ann Surg Oncol, 2014;21:560-568.
- Ito Y, Hashimoto M, Hirota K, Ohkura N, Morikawa H, Nishikawa H, Tanaka A, Furu M, Ito H, Fujii T, Nomura T, Yamazaki S, Morita A, Vignali DA, Kappler JW, Matsuda S, Mimori T, Sakaguchi N, Sakaguchi S. Detection of T cell responses to a ubiquitous cellular protein in autoimmune disease. Science, 2014;346:363-368.
- Kochin V, Shimi T, Torvaldson E, Adam SA, Goldman A, Pack CG, Melo-Cardenas J, Imanishi SY, Goldman RD, Eriksson JE. Interphase phosphorylation of lamin A. J Cell Sci, 2014;127:2683-2696.
- Liu L, Nishio N, Ito S, Tanaka Y, Isobe K. Negative regulation of GADD34 on myofibroblasts during cutaneous wound healing. Biomed Res Int, 2014;2014:137049.
- Maeda Y, Nishikawa H, Sugiyama D, Ha D, Hamaguchi M, Saito T, Nishioka M, Wing JB, Adeegbe D, Katayama I, Sakaguchi S. Detection of self-reactive CD8⁺ T cells with an anergic phenotype in healthy individuals. Science, 2014;346:1536-1540.
- Matsumoto M, Baba A, Yokota T, Nishikawa H, Ohkawa Y, Kayama H, Kallies A, Nutt SL, Sakaguchi S, Takeda K, Kurosaki T, Baba Y. Interleukin-10-producing plasmablasts exert regulatory function in autoimmune inflammation. Immunity, 2014;41:1040-1051.
- Morishima A, Hirano T, Nishikawa H, Nakai K, Sakaguchi S, Kumanogoh A. Comprehensive exploration of autoantibody in Behçet's disease: a novel autoantibody to claudin-1, an essential protein for tight junctions, is identified. Joint Bone Spine, 2014;81:546-548.
- Morita R, Nishizawa S, Torigoe T, Takahashi A, Tamura Y, Tsukahara T, Kanaseki T, Sokolovskaya A, Kochin V, Kondo T, Hashino S, Asaka M, Hara I, Hirohashi Y, Sato N. Heat shock protein DNAJB8 is a novel target for immunotherapy of colon cancer-initiating cells. Cancer Sci, 2014;105:389-395.
- Nishikawa H, Sakaguchi S. Regulatory T cells in cancer immunotherapy. Curr Opin Immunol, 2014;27:1-7.
- Nishio N, Ito S, Isobe K. Loss of GADD34 induces early age-dependent deviation to the myeloid lineage. Immunol Cell Biol, 2014;92:170-180.
- Saito T, Wada H, Yamasaki M, Miyata H, Nishikawa H, Sato E, Kageyama S, Shiku H, Mori M, Doki Y. High expression of MAGE-A4 and MHC class I antigens in tumor cells and induction of MAGE-A4 immune responses are prognostic markers of CHP-MAGE-A4 cancer vaccine. Vaccine, 2014;32:5901-5907.
- Sun Y, Ito S, Nishio N, Tanaka Y, Chen N, Isobe K. Acrolein induced both pulmonary inflammation and the death of lung epithelial cells. Toxicol Lett, 2014;229:384-392.
- Tsukahara T, Emori M, Murata K, Hirano T, Muroi N, Kyono M, Toji S, Watanabe K, Torigoe T, Kochin V, Asanuma H, Matsumiya H, Yamashita K, Himi T, Ichimiya S, Wada T, Yamashita T, Hasegawa T, Sato N. Specific targeting of a naturally presented osteosarcoma antigen, papillomavirus binding factor peptide, using an artificial monoclonal antibody. J Biol Chem, 2014;289:22035-22047.
- Wada H, Isobe M, Kakimi K, Mizote Y, Eikawa S, Sato E, Takigawa N, Kiura K, Tsuji K, Iwatsuki K, Yamasaki M, Miyata H, Matsushita H, Udono H, Seto Y, Yamada K, Nishikawa H, Pan L, Venhaus R, Oka M, Doki Y, Nakayama E. Vaccination with NY-ESO-1 overlapping peptides mixed with Picibanil OK-432 and montanide ISA-51 in patients with cancers expressing the NY-ESO-1 antigen. J Immunother, 2014;37:84-92.
2013
- Adeegbe DO, Nishikawa H. Natural and induced T regulatory cells in cancer. Front Immunol, 2013;4:190.
- Atarashi K, Tanoue T, Oshima K, Suda W, Nagano Y, Nishikawa H, Fukuda S, Saito T, Narushima S, Hase K, Kim S, Fritz JV, Wilmes P, Ueha S, Matsushima K, Ohno H, Olle B, Sakaguchi S, Taniguchi T, Morita H, Hattori M, Honda K. Treg induction by a rationally selected mixture of Clostridia strains from the human microbiota. Nature, 2013;500:232-236.
- Cheng Z, Ito S, Nishio N, Thanasegaran S, Fang H, Isobe K. Characteristics of cardiac aging in C57BL/6 mice. Exp Gerontol, 2013;48:341-348.
- Eikawa S, Kakimi K, Isobe M, Kuzushima K, Luescher I, Ohue Y, Ikeuchi K, Uenaka A, Nishikawa H, Udono H, Oka M, Nakayama E. Induction of CD8 T-cell responses restricted to multiple HLA class I alleles in a cancer patient by immunization with a 20-mer NY-ESO-1f (NY-ESO-1 91-110) peptide. Int J Cancer, 2013;132:345-354.
- Emori M, Tsukahara T, Murase M, Kano M, Murata K, Takahashi A, Kubo T, Asanuma H, Yasuda K, Kochin V, Kaya M, Nagoya S, Nishio J, Iwasaki H, Sonoda T, Hasegawa T, Torigoe T, Wada T, Yamashita T, Sato N. High expression of CD109 antigen regulates the phenotype of cancer stem-like cells/cancer-initiating cells in the novel epithelioid sarcoma cell line ESX and is related to poor prognosis of soft tissue sarcoma. PLoS One, 2013;8:e84187.
- Fujiwara S, Wada H, Kawada J, Kawabata R, Takahashi T, Fujita J, Hirao T, Shibata K, Makari Y, Iijima S, Nishikawa H, Jungbluth AA, Nakamura Y, Kurokawa Y, Yamasaki M, Miyata H, Nakajima K, Takiguchi S, Nakayama E, Mori M, Doki Y. NY-ESO-1 antibody as a novel tumour marker of gastric cancer. Br J Cancer, 2013;108:1119-1125.
- Gupta A, Nuber N, Esslinger C, Wittenbrink M, Treder M, Landshammer A, Noguchi T, Kelly M, Gnjatic S, Ritter E, von Boehmer L, Nishikawa H, Shiku H, Old L, Ritter G, Knuth A, van den Broek M. A novel human-derived antibody against NY-ESO-1 improves the efficacy of chemotherapy. Cancer Immun, 2013;13:3.
- Himeno T, Kamiya H, Naruse K, Cheng Z, Ito S, Kondo M, Okawa T, Fujiya A, Kato J, Suzuki H, Kito T, Hamada Y, Oiso Y, Isobe K, Nakamura J. Mesenchymal stem cell-like cells derived from mouse induced pluripotent stem cells ameliorate diabetic polyneuropathy in mice. Biomed Res Int, 2013;2013:259187.
- Hirayama M, Nishikawa H, Nagata Y, Tsuji T, Kato T, Kageyama S, Ueda S, Sugiyama D, Hori S, Sakaguchi S, Ritter G, Old LJ, Gnjatic S, Shiku H. Overcoming regulatory T-cell suppression by a lyophilized preparation of Streptococcus pyogenes. Eur J Immunol, 2013;43:989-1000.
- Ito S, Tanaka Y, Nishio N, Thanasegaran S, Isobe K. Establishment of self-renewable GM-CSF-dependent immature macrophages in vitro from murine bone marrow. PLoS One, 2013;8:e76943.
- Kito T, Shibata R, Ishii M, Suzuki H, Himeno T, Kataoka Y, Yamamura Y, Yamamoto T, Nishio N, Ito S, Numaguchi Y, Tanigawa T, Yamashita JK, Ouchi N, Honda H, Isobe K, Murohara T. iPS cell sheets created by a novel magnetite tissue engineering method for reparative angiogenesis. Sci Rep, 2013;3:1418.
- Liu B, Ohishi K, Orito Y, Nakamori Y, Nishikawa H, Ino K, Suzuki K, Matsumoto T, Masuya M, Hamada H, Mineno J, Ono R, Nosaka T, Shiku H, Katayama N. Manipulation of human early T lymphopoiesis by coculture on human bone marrow stromal cells: potential utility for adoptive immunotherapy. Exp Hematol, 2013;41:367-376.e361.
- Muraoka D, Nishikawa H, Noguchi T, Wang L, Harada N, Sato E, Luescher I, Nakayama E, Kato T, Shiku H. Establishment of animal models to analyze the kinetics and distribution of human tumor antigen-specific CD8⁺ T cells. Vaccine, 2013;31:2110-2118.
- Noguchi T, Ritter G, Nishikawa H. Antibody-based therapy in colorectal cancer. Immunotherapy, 2013;5:533-545.
- Okawa T, Kamiya H, Himeno T, Kato J, Seino Y, Fujiya A, Kondo M, Tsunekawa S, Naruse K, Hamada Y, Ozaki N, Cheng Z, Kito T, Suzuki H, Ito S, Oiso Y, Nakamura J, Isobe K. Transplantation of neural crest-like cells derived from induced pluripotent stem cells improves diabetic polyneuropathy in mice. Cell Transplant, 2013;22:1767-1783.
- Okuno Y, Murakoshi A, Negita M, Akane K, Kojima S, Suzuki H. CD8+ CD122+ regulatory T cells contain clonally expanded cells with identical CDR3 sequences of the T-cell receptor β-chain. Immunology, 2013;139:309-317.
- Saijo H, Hirohashi Y, Torigoe T, Kochin V, Takahashi H, Sato N. Cytotoxic T lymphocytes: the future of cancer stem cell eradication? Immunotherapy, 2013;5:549-551.
- Shozib HB, Suzuki H, Iino S, Nakayama S. Acceleration of ileal pacemaker activity in mice lacking interleukin 10. Inflamm Bowel Dis, 2013;19:1577-1585.
- Sugiyama D, Nishikawa H, Maeda Y, Nishioka M, Tanemura A, Katayama I, Ezoe S, Kanakura Y, Sato E, Fukumori Y, Karbach J, Jäger E, Sakaguchi S. Anti-CCR4 mAb selectively depletes effector-type FoxP3+CD4+ regulatory T cells, evoking antitumor immune responses in humans. Proc Natl Acad Sci U S A, 2013;110:17945-17950.
- Takahashi A, Hirohashi Y, Torigoe T, Tamura Y, Tsukahara T, Kanaseki T, Kochin V, Saijo H, Kubo T, Nakatsugawa M, Asanuma H, Hasegawa T, Kondo T, Sato N. Ectopically expressed variant form of sperm mitochondria-associated cysteine-rich protein augments tumorigenicity of the stem cell population of lung adenocarcinoma cells. PLoS One, 2013;8:e69095.
- Thanasegaran S, Cheng Z, Ito S, Nishio N, Isobe K. No immunogenicity of IPS cells in syngeneic host studied by in vivo injection and 3D scaffold experiments. Biomed Res Int, 2013;2013:378207.
- Yasuda K, Torigoe T, Morita R, Kuroda T, Takahashi A, Matsuzaki J, Kochin V, Asanuma H, Hasegawa T, Saito T, Hirohashi Y, Sato N. Ovarian cancer stem cells are enriched in side population and aldehyde dehydrogenase bright overlapping population. PLoS One, 2013;8:e68187.
2012
- Fujiwara S, Wada H, Miyata H, Kawada J, Kawabata R, Nishikawa H, Gnjatic S, Sedrak C, Sato E, Nakamura Y, Sakakibara M, Kanto T, Shimosegawa E, Hatazawa J, Takahashi T, Kurokawa Y, Yamasaki M, Nakajima K, Takiguchi S, Nakayama E, Mori M, Doki Y. Clinical trial of the intratumoral administration of labeled DC combined with systemic chemotherapy for esophageal cancer. J Immunother, 2012;35:513-521.
- Hirohashi Y, Torigoe T, Inoda S, Morita R, Kochin V, Sato N. Cytotoxic T lymphocytes: Sniping cancer stem cells. Oncoimmunology, 2012;1:123-125.
- Isobe K, Cheng Z, Ito S, Nishio N. Aging in the mouse and perspectives of rejuvenation through induced pluripotent stem cells (iPSCs). Results Probl Cell Differ, 2012;55:413-427.
- Ito S, Nishio N, Isobe K. Analysis of b-amyloid peptide-binding proteins in microglial cells. The Open geriatric medicine journal, 2012; 5: 1-6.
- Iwami K, Shimato S, Ohno M, Okada H, Nakahara N, Sato Y, Yoshida J, Suzuki S, Nishikawa H, Shiku H, Natsume A, Wakabayashi T. Peptide-pulsed dendritic cell vaccination targeting interleukin-13 receptor α2 chain in recurrent malignant glioma patients with HLA-A*24/A*02 allele. Cytotherapy, 2012;14:733-742.
- Kawada J, Wada H, Isobe M, Gnjatic S, Nishikawa H, Jungbluth AA, Okazaki N, Uenaka A, Nakamura Y, Fujiwara S, Mizuno N, Saika T, Ritter E, Yamasaki M, Miyata H, Ritter G, Murphy R, Venhaus R, Pan L, Old LJ, Doki Y, Nakayama E. Heteroclitic serological response in esophageal and prostate cancer patients after NY-ESO-1 protein vaccination. Int J Cancer, 2012;130:584-592.
- Mori T, Nishizawa S, Hirohashi Y, Torigoe T, Tamura Y, Takahashi A, Kochin V, Fujii R, Kondo T, Greene MI, Hara I, Sato N. Efficiency of G2/M-related tumor-associated antigen-targeting cancer immunotherapy depends on antigen expression in the cancer stem-like population. Exp Mol Pathol, 2012;92:27-32.
- Nakamori Y, Liu B, Ohishi K, Suzuki K, Ino K, Matsumoto T, Masuya M, Nishikawa H, Shiku H, Hamada H, Katayama N. Human bone marrow stromal cells simultaneously support B and T/NK lineage development from human haematopoietic progenitors: a principal role for flt3 ligand in lymphopoiesis. Br J Haematol, 2012;157:674-686.
- Nishikawa H, Maeda Y, Ishida T, Gnjatic S, Sato E, Mori F, Sugiyama D, Ito A, Fukumori Y, Utsunomiya A, Inagaki H, Old LJ, Ueda R, Sakaguchi S. Cancer/testis antigens are novel targets of immunotherapy for adult T-cell leukemia/lymphoma. Blood, 2012;119:3097-3104.
- Noguchi T, Kato T, Wang L, Maeda Y, Ikeda H, Sato E, Knuth A, Gnjatic S, Ritter G, Sakaguchi S, Old LJ, Shiku H, Nishikawa H. Intracellular tumor-associated antigens represent effective targets for passive immunotherapy. Cancer Res, 2012;72:1672-1682.
- Suzuki H, Shibata R, Kito T, Yamamoto T, Ishii M, Nishio N, Ito S, Isobe K, Murohara T. Comparative angiogenic activities of induced pluripotent stem cells derived from young and old mice. PLoS One, 2012;7:e39562.
- Suzuki S, Masaki A, Ishida T, Ito A, Mori F, Sato F, Narita T, Ri M, Kusumoto S, Komatsu H, Fukumori Y, Nishikawa H, Tanaka Y, Niimi A, Inagaki H, Iida S, Ueda R. Tax is a potential molecular target for immunotherapy of adult T-cell leukemia/lymphoma. Cancer Sci, 2012;103:1764-1773.
- Uddin MN, Nishio N, Ito S, Suzuki H, Isobe K. Autophagic activity in thymus and liver during aging. Age (Dordr), 2012;34:75-85.
2011
- Cheng Z, Ito S, Nishio N, Xiao H, Zhang R, Suzuki H, Okawa Y, Murohara T, Isobe K. Establishment of induced pluripotent stem cells from aged mice using bone marrow-derived myeloid cells. J Mol Cell Biol, 2011;3:91-98.
- Endharti AT, Okuno Y, Shi Z, Misawa N, Toyokuni S, Ito M, Isobe K, Suzuki H. CD8+CD122+ regulatory T cells (Tregs) and CD4+ Tregs cooperatively prevent and cure CD4+ cell-induced colitis. J Immunol, 2011;186:41-52.
- Hayakawa A, Suzuki H, Kamei Y, Tanuma S, Magae J. Cladribine enhances apoptotic cell death in lung carcinoma cells over-expressing DNase γ. Biol Pharm Bull, 2011;34:1001-1004.
- Inami Y, Yoshikai T, Ito S, Nishio N, Suzuki H, Sakurai H, Isobe K. Differentiation of induced pluripotent stem cells to thymic epithelial cells by phenotype. Immunol Cell Biol, 2011;89:314-321.
- Toda M, Wang L, Ogura S, Torii M, Kurachi M, Kakimi K, Nishikawa H, Matsushima K, Shiku H, Kuribayashi K, Kato T. UV irradiation of immunized mice induces type 1 regulatory T cells that suppress tumor antigen specific cytotoxic T lymphocyte responses. Int J Cancer, 2011;129:1126-1136.
- Uddin MN, Ito S, Nishio N, Suganya T, Isobe K. Gadd34 induces autophagy through the suppression of the mTOR pathway during starvation. Biochem Biophys Res Commun, 2011;407:692-698.
- Zhang R, Ito S, Nishio N, Cheng Z, Suzuki H, Isobe KI. Dextran sulphate sodium increases splenic Gr1(+)CD11b(+) cells which accelerate recovery from colitis following intravenous transplantation. Clin Exp Immunol, 2011;164:417-427.
- Zhang R, Ito S, Nishio N, Cheng Z, Suzuki H, Isobe K. Up-regulation of Gr1+CD11b+ population in spleen of dextran sulfate sodium administered mice works to repair colitis. Inflamm Allergy Drug Targets, 2011;10:39-46.
2010
- de Thonel A, Ferraris SE, Pallari HM, Imanishi SY, Kochin V, Hosokawa T, Hisanaga S, Sahlgren C, Eriksson JE. Protein kinase Czeta regulates Cdk5/p25 signaling during myogenesis. Mol Biol Cell, 2010;21:1423-1434.
- Mitsui J, Nishikawa H, Muraoka D, Wang L, Noguchi T, Sato E, Kondo S, Allison JP, Sakaguchi S, Old LJ, Kato T, Shiku H. Two distinct mechanisms of augmented antitumor activity by modulation of immunostimulatory/inhibitory signals. Clin Cancer Res, 2010;16:2781-2791.
- Muraoka D, Kato T, Wang L, Maeda Y, Noguchi T, Harada N, Takeda K, Yagita H, Guillaume P, Luescher I, Old LJ, Shiku H, Nishikawa H. Peptide vaccine induces enhanced tumor growth associated with apoptosis induction in CD8+ T cells. J Immunol, 2010;185:3768-3776.
2009
- Kaunisto A, Kochin V, Asaoka T, Mikhailov A, Poukkula M, Meinander A, Eriksson JE. PKC-mediated phosphorylation regulates c-FLIP ubiquitylation and stability. Cell Death Differ, 2009;16:1215-1226.
2008
- Nishikawa H, Tsuji T, Jäger E, Briones G, Ritter G, Old LJ, Galán JE, Shiku H, Gnjatic S. Induction of regulatory T cell-resistant helper CD4+ T cells by bacterial vector. Blood, 2008;111:1404-1412.
- Nishikawa H, Kato T, Hirayama M, Orito Y, Sato E, Harada N, Gnjatic S, Old LJ, Shiku H. Regulatory T cell-resistant CD8+ T cells induced by glucocorticoid-induced tumor necrosis factor receptor signaling. Cancer Res, 2008;68:5948-5954.
2006
- Kochin V, Imanishi SY, Eriksson JE. Fast track to a phosphoprotein sketch - MALDI-TOF characterization of TLC-based tryptic phosphopeptide maps at femtomolar detection sensitivity. Proteomics, 2006;6:5676-5682.
- Nishikawa H, Sato E, Briones G, Chen LM, Matsuo M, Nagata Y, Ritter G, Jäger E, Nomura H, Kondo S, Tawara I, Kato T, Shiku H, Old LJ, Galán JE, Gnjatic S. In vivo antigen delivery by a Salmonella typhimurium type III secretion system for therapeutic cancer vaccines. J Clin Invest, 2006;116:1946-1954.
- Nishikawa H, Qian F, Tsuji T, Ritter G, Old LJ, Gnjatic S, Odunsi K. Influence of CD4+CD25+ regulatory T cells on low/high-avidity CD4+ T cells following peptide vaccination. J Immunol, 2006;176:6340-6346.
2005
- Nishikawa H, Kato T, Tawara I, Takemitsu T, Saito K, Wang L, Ikarashi Y, Wakasugi H, Nakayama T, Taniguchi M, Kuribayashi K, Old LJ, Shiku H. Accelerated chemically induced tumor development mediated by CD4+CD25+ regulatory T cells in wild-type hosts. Proc Natl Acad Sci U S A, 2005;102:9253-9257.
- Nishikawa H, Jäger E, Ritter G, Old LJ, Gnjatic S. CD4+ CD25+ regulatory T cells control the induction of antigen-specific CD4+ helper T cell responses in cancer patients. Blood, 2005;106:1008-1011.
- Nishikawa H, Kato T, Tawara I, Saito K, Ikeda H, Kuribayashi K, Allen PM, Schreiber RD, Sakaguchi S, Old LJ, Shiku H. Definition of target antigens for naturally occurring CD4(+) CD25(+) regulatory T cells. J Exp Med, 2005;201:681-686.
- Nishikawa H, Kato T, Tawara I, Ikeda H, Kuribayashi K, Allen PM, Schreiber RD, Old LJ, Shiku H. IFN-gamma controls the generation/activation of CD4+ CD25+ regulatory T cells in antitumor immune response. J Immunol, 2005;175:4433-4440.
2003
- Nishikawa H, Kato T, Tanida K, Hiasa A, Tawara I, Ikeda H, Ikarashi Y, Wakasugi H, Kronenberg M, Nakayama T, Taniguchi M, Kuribayashi K, Old LJ, Shiku H. CD4+ CD25+ T cells responding to serologically defined autoantigens suppress antitumor immune responses. Proc Natl Acad Sci U S A, 2003;100:10902-10906.
2001
- Nishikawa H, Tanida K, Ikeda H, Sakakura M, Miyahara Y, Aota T, Mukai K, Watanabe M, Kuribayashi K, Old LJ, Shiku H. Role of SEREX-defined immunogenic wild-type cellular molecules in the development of tumor-specific immunity. Proc Natl Acad Sci U S A, 2001;98:14571-14576.

