Ophthalmology/Protective Care for Sensory Disorders
KEYWORDS
- Applied Genetics
- Translational Research
HEAD

LAB MEMBER
| Faculty | Position | Researchers |
|---|---|---|
| YUKI Kenya | Associate Professor | Researchers |
| USHIDA Hiroaki | Lecturer | Researchers |
| KOMINAMI Taro | Lecturer | Researchers |
| FUJITA Kosuke | Assistant Professor | Researchers |
| TOMITA Ryo | Assistant Professor | |
| TAKEUCHI Jun | Assistant Clinical Professor | Researchers |
| SHIMIZU Hideyuki | Assistant Professor | Researchers |
| SUZUMURA Ayana | Assistant Clinical Professor | Researchers |
| SAJIKI FUJITA Ai | Assistant Professor | Researchers |
| YASUDA Sayuri | Assistant Clinical Professor | Researchers |
| TAKI Yosuke | Assistant Clinical Professor | Researchers |
| HIRAZAWA Kiichi | Project Assistant Professor | |
| OTA Hikaru | Assistant Clinical Professor | |
| INOOKA Taiga | Assistant Clinical Professor | Researchers |
CONTACT
| iga-ryu◎t.mail.nagoya-u.ac.jp (Please send a message after replacing "◎" mark with "@" mark. ) | |
| HP | Private Page |
OUTLINE
The Department of Ophthalmology of the Nagoya University Medical School was founded in 1882, and throughout its long history, the clinical and experimental programs have been focused on the diagnosis and treatment of retinal diseases. Thus, the department has performed clinical and laboratory research designed to improve the diagnosis and treatment of patients with age-related macular disease, diabetic retinopathy, and retinal detachments. The diagnosis is made with the most innovative devices, and the surgery is performed with the most advanced surgical instruments. Vitrectomy is performed on more than 700 cases/year with good outcomes. Hereditary retinal dystrophies and optic nerve diseases are also diagnosed and treated with many of the techniques developed in our department.
Our staff also includes skilled and experienced doctors who specialize in corneal diseases, glaucoma, pediatric ocular diseases including strabismus, uveal diseases, uveal diseases, ocular tumors, oculoplastic surgery, low vision, and other diseases and disorders of the eye.
RESEARCH PROJECTS
A: Applied Genetics Team
Our goal
Through translational research, we aim to elucidate of the pathogenesis of ocular diseases through multi-omics analysis of human samples and development of novel gene therapy for retinal diseases and glaucoma.
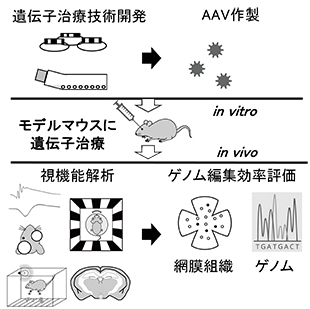
Our research
We are focused on developing novel gene therapy for inherited retinal degeneration and other ocular disease, with specific attention to genome editing technology using patient-derived cells and specimen, mice, and monkeys.
We also explore pathogenesis of ocular diseases using cutting-edge multi-omics analysis with the aim of finding therapeutic target and clinically useful biomarkers.
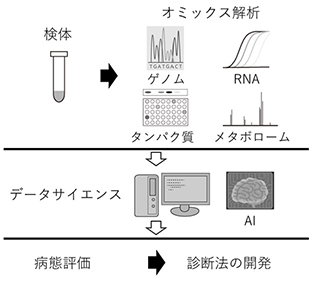
B: Reverse Translational Research Team
Our group has been conducting reverse translational research to solve clinical problems by applying basic research methods using samples such as vitreous humor and anterior chamber aqueous humor from patients, based on the unique viewpoint of clinicians on the symptoms and problems of retinal diseases.
We have reported that histamine H4 receptors, which are allergy-related, are expressed in choroidal neovascularization in age-related macular degeneration and may be a potential new therapeutic target. We have also reported that the metabolite 18-HEPE specifically acts on Müller glial cells in the retina by oral administration of eicosapentaenoic acid (EPA), an ω3 fatty acid, and it may treat the functional impairment of neuroretinal cells seen in early diabetes via brain-derived trophic factor (BDNF).
In addition, we are conducting multifaceted research on retinal diseases, such as proposing a new concept of retinal disorders by elucidating the pathogenesis of silicone oil-related vision loss (SORVL).
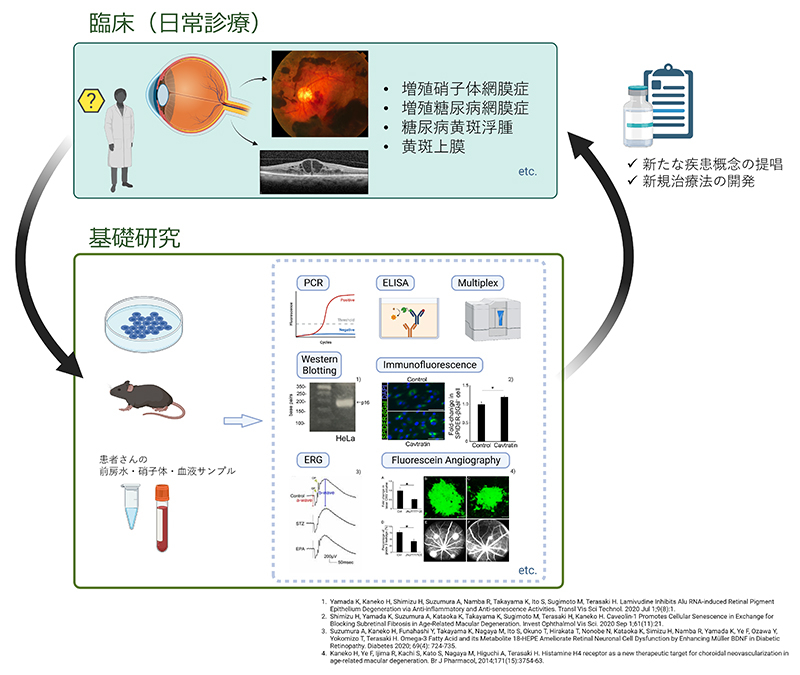
C. Glaucoma Team
Glaucoma is the leading cause of blindness in Japan.
Therefore, new findings on glaucoma are needed to provide better medical care.
The glaucoma research group is researching visual function and structure relationships in glaucoma patients, the quality of life of the glaucoma patients, and glaucoma surgery. Our accomplishments will be presented at national and international conferences and academic journals.
D. Macular Disease Team
We are engaged in clinical research using OCT/OCTA imaging and aqueous humor cytokine profiling for macular diseases such as age-related macular degeneration and pachychoroid diseases. Taking advantage of the abundant number of cases at Nagoya university hospital, we are working to elucidate the pathophysiology of macular diseases and to build evidence that will be directly relevant to tomorrow’s practice.
E. Uveitis Team
About 30-40% of patients with uveitis have unknown causes. Our goal is to elucidate the causes of these diseases and to create new examination methods by applying molecular biological techniques.
In addition, we aim to improve the diagnostic rate of vitreoretinal lymphoma, which is difficult to diagnose.
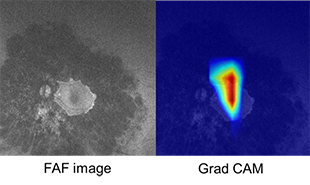
F. AI Team
Artificial intelligence (AI) has made remarkable progress in recent years with the big data and the development of computer resource. AI is also spreading in the field of ophthalmology. We try to apply machine learning techniques to assessing progression of retinal diseases.
BIBLIOGRAPHY
2024
- Kensuke Goto , Ryo Tomita, Jiro Hiraiwa , Mitsuki Kawabe , Koji M Nishiguchi , Kenya Yuki. “Secondary Angle Closure Caused by Anterior Displacement of Capsular Tension Ring and Intraocular Lens Due to Aqueous Misdirection” Cureus. 2024 Mar 7;16(3):e55716.
- Mathieu Quinodoz, Karolina Kaminska, Francesca Cancellieri, Ji Hoon Han, Virginie G Peter, Elifnaz Celik, Lucas Janeschitz-Kriegl, Nils Schärer, Daniela Hauenstein, Bence György, Giacomo Calzetti, Vincent Hahaut, Sónia Custódio, Ana Cristina Sousa, Yuko Wada, Yusuke Murakami, Almudena Avila Fernández, Cristina Rodilla Hernández, Pablo Minguez, Carmen Ayuso, Koji M Nishiguchi, Cristina Santos, Luisa Coutinho Santos, Viet H Tran, Veronika Vaclavik, Hendrik P N Scholl, Carlo Rivolta. “Detection of elusive DNA copy-number variations in hereditary disease and cancer through the use of noncoding and off-target sequencing reads” Am J Hum Genet. 2024 Apr 4;111(4):701-713.
- Akiko Suga, Kei Mizobuchi, Taiga Inooka, Kazutoshi Yoshitake, Naoko Minematsu, Kazushige Tsunoda, Kazuki Kuniyoshi, Yosuke Kawai, Yosuke Omae, Katsushi Tokunaga, Takaaki Hayashi, Shinji Ueno, Takeshi Iwata. “A homozygous structural variant of RPGRIP1 is frequently associated with achromatopsia in Japanese patients with IRD” Genet Med Open. 2024 Mar 26:2:101843.
- Katsuya Yamaguchi, Ryo Tomita, Yoshito Koyanagi, Kazuhide Kawase, Ryo Asaoka, Hiroko Terasaki, Takeshi Iwase, Koji M Nishiguchi. “Abilities of circumpapillary retinal nerve fiber layer thickness and vascular density to discriminate stages in primary open-angle glaucoma” Graefes Arch Clin Exp Ophthalmol. 2024 Apr;262(4):1221-1229.
- Kelvin Yi Chong Teo, Kyu-Hyung Park, Nor Fariza Ngah , Shih-Jen Chen, Paisan Ruamviboonsuk, Ryusaburo Mori, Nagako Kondo, Won Ki Lee, Rajesh Rajagopalan, Ryo Obata, Ian Y H Wong, Caroline Chee, Hiroko Terasaki, Tetsuju Sekiryu, Shih-Chou Chen, Yasuo Yanagi, Shigeru Honda, Timothy Y Y Lai, Chui Ming Gemmy Cheung. “Six-Year Outcomes in Subjects with Polypoidal Choroidal Vasculopathy in the EVEREST II Study” Ophthalmol Ther. 2024 Apr;13(4):935-954.
- Satoru Inoda, Hidenori Takahashi, Maiko Maruyama-Inoue, Shoko Ikeda, Tetsuju Sekiryu, Kanako Itagaki, Hidetaka Matsumoto, Ryo Mukai, Yoshimi Nagai, Masayuki Ohnaka, Sentaro Kusuhara, Akiko Miki, Annabelle A Okada, Makiko Nakayama, Koji M Nishiguchi, Jun Takeuchi, Ryusaburo Mori, Koji Tanaka, Shigeru Honda, Takeya Kohno, Hideki Koizumi, Yasunori Miyara, Yuji Inoue, Hiroki Takana, Tomohiro Iida, Ichiro Maruko, Atsushi Hayashi, Tomoko Ueda-Consolvo, Yasuo Yanagi. “INCIDENCE AND RISK FACTORS OF INTRAOCULAR INFLAMMATION AFTER BROLUCIZUMAB TREATMENT IN JAPAN: A Multicenter Age-Related Macular Degeneration Study” Retina. 2024 Apr 1;44(4):714-722.
- Yoshiki Kato, Taro Kominami. “A Case of Sickle Cell Retinopathy With Retinal Artery Occlusion in African-Japanese Patients” Cureus. 2024 May 20;16(5):e60653.
- Hiroaki Ushida, Ayana Suzumura, Kazuhisa Yamada, Hideyuki Shimizu, Atsuo Suzuki, Yusuke Ishikawa, Ryosuke Kikuch, Koji M Nishiguchi, Hiroki Kaneko. “Decrease in electrolyte after vitrectomy surgery may affect the results of forensic investigations using vitreous humor” BMC Opthalmol. 2024 May 23;24(1):219.
- Daisuke Mori, Chihiro Inami, Ryosuke Ikeda, Masahito Sawahata, Shinji Urata, Sho T Yamaguchi, Yohei Kobayashi, Kosuke Fujita, Yuko Arioka, Hiroki Okumura, Itaru Kushima, Akiko Kodama, Toshiaki Suzuki, Takashi Hirao, Akira Yoshimi, Akira Sobue, Takahiro Ito, Yukikiro Noda, Hiroyuki Mizoguchi, Taku Nagai, Kozo Kaibuchi, Shigeo Okabe, Koji Nishiguchi, Kazuhiko Kume, Kiyofumi Yamada, Norio Ozaki. “Mice with deficiency in Pcdh15, a gene associated with bipolar disorders, exhibit significantly elevated diurnal amplitudes of locomotion and body temperature” Transl Psychiatry. 2024 May 28;14(1):216.
- Kensuke Goto, Yoshito Koyanagi, Masato Akiyama, Yusuke Murakami, Masatoshi Fukushima, Kohta Fujiwara, Hanae Iijima, Mitsuyo Yamaguchi, Mikiko Endo, Kazuki Hashimoto, Masataka Ishizu, Toshiaki Hirakata, Kei Mizobuchi, Masakazu Takayama, Junya Ota, Ai Fujita Sajiki, Taro Kominami, Hiroaki Ushida, Kosuke Fujita, Hiroki Kaneko, Shinji Ueno, Takaaki Hayashi, Chikashi Terao, Yoshihiro Hotta, Akira Murakami, Kazuki Kuniyoshi, Shunji Kusaka, Yuko Wada, Toshiaki Abe, Toru Nakazawa, Yasuhiro Ikeda, Yukihide Momozawa, Koh-Hei Sonoda, Koji M Nishiguchi. “Disease-specific variant interpretation highlighted the genetic findings in 2325 Japanese patients with retinitis pigmentosa and allied diseases” J Med Genet. 2024 Jun 20;61(7):613-620.
- Kaoru Fujinami, Koji M Nishiguchi, Akio Oishi, Masato Akiyama, Yasuhiro Ikeda. “Specification of variant interpretation guidelines for inherited retinal dystrophy in Japan” Jpn J Ophthalmol. 2024 Jul;68(4):389-399.
- Kei Mizobuchi, Takaaki Hayashi, Koji Tanaka, Kazuki Kuniyoshi, Yusuke Murakami, Natsuko Nakamura, Kaoruko Torii, Atsushi Mizota, Daiki Sakai, Akiko Maeda, Taro Kominami, Shinji Ueno, Shunji Kusaka, Koji M Nishiguchi, Yasuhiro Ikeda, Mineo Kondo, Kazushige Tsunoda, Yoshihiro Hotta, Tadashi Nakano. “Genetic and Clinical Features of ABCA4-Associated Retinopathy in a Japanese Nationwide Cohort” Am J Ophthalmol. 2024 Aug:264:36-43.
- Takahito Todoroki, Jun Takeuchi, Hikaru Ota, Yuyako Nakano, Ai Fujita Sajiki, Koichi Nakamura, Hiroki Kaneko, Koji M Nishiguchi. “Aqueous Humor Cytokine Analysis in Age-Related Macular Degeneration After Switching From Aflibercept to Faricimab” Invest Ophthalmol Vis Sci. 2024 Sep 3;65(11):15.
- Yutaka Kato, Kenya Yuki, Koji Nishiguchi, Shinji Naganawa. “Visualization of distribution in the vitreous cavity via eye drops using ultra-heavily T2-weighted sequences in MRI: a preliminary study with enucleated pig eyes” Radiol Phys Technol. 2024 Sep;17(3):715-724.
- Taiga Inooka, Takaaki Hayashi, Kazushige Tsunoda, Kazuki Kuniyoshi, Hiroyuki Kondo, Kei Mizobuchi, Akiko Suga, Takeshi Iwata, Kazutoshi Yoshitake, Mineo Kondo, Kensuke Goto, Junya Ota, Taro Kominami, Koji M Nishiguchi, Shinji Ueno. “GENETIC ETIOLOGY AND CLINICAL FEATURES OF ACHROMATOPSIA IN JAPAN” Retina. 2024 Oct 1;44(10):1836-1844.
- Keigo Natsume, Taro Kominami, Kensuke Goto, Yoshito Koyanagi, Taiga Inooka, Junya Ota, Kenichi Kawano, Kazuhisa Yamada, Daishi Okuda, Kenya Yuki, Koji M Nishiguchi, Hiroaki Ushida. “Phenotypic variability of RP1-related inherited retinal dystrophy associated with the c.5797 C > T (p.Arg1933*) variant in the Japanese population” Sci Rep. 2024 Oct 27;14(1):25669.
- Ryo Tomita, Ryo Asaoka, Kazunori Hirasawa, Yuri Fujino, Tetsuro Omura, Tsutomu Inatomi, Akira Obana, Koji M Nishiguchi, Masaki Tanito. “A Novel Approach To Predict Glaucomatous Impairment in the Central 10° Visual Field, Excluding the Effect of Cataract” Transl Vis Sci Technol. 2024 Oct 1;13(10):35.
- Hikaru Ota, Keiko Kataoka, Keiko Asai, Jun Takeuchi, Yuyako Nakano, Koichi Nakamura, Takahito Todoroki, Koji M Nishiguchi. “Five-year outcomes of treat and extend regimen using intravitreal aflibercept injection for treatment-naïve age-related macular degeneration” Graefes Arch Clin Exp Ophthalmol. 2024 Nov;262(11):3483-3491.
- Shun Nakamura, Kohta Fujiwara, Masatoshi Fukushima, Sakurako Shimokawa, Shotaro Shimokawa, Yoshito Koyanagi, Toshio Hisatomi, Atsunobu Takeda, Ikeda Yasuhiro, Yusuke Murakami, Koh-Hei Sonoda. “Relationships between causative genes and epiretinal membrane formation in Japanese patients with retinitis pigmentosa” Graefes Arch Clin Exp Ophthalmol. 2024 Nov;262(11):3553-3558.
- Masato Akiyama, Gen Tamiya, Kohta Fujiwara, Yukihiro Shiga, Yu Yokoyama, Kazuki Hashimoto, Masataka Sato, Kota Sato, Akira Narita, Sawako Hashimoto, Emi Ueda, Yoshihiko Furuta, Jun Hata, Masahiro Miyake, Hanako O Ikeda, Kenji Suda, Shogo Numa, Yuki Mori, Kazuya Morino, Yusuke Murakami, Sakurako Shimokawa, Shun Nakamura, Nobuyo Yawata, Kimihiko Fujisawa, Satoshi Yamana, Kenichiro Mori, Yasuhiro Ikeda, Kazunori Miyata, Keisuke Mori, Ken Ogino, Yoshito Koyanagi, Yoichiro Kamatani, Biobank Japan Project, Toshiharu Ninomiya, Koh-Hei Sonoda, Toru Nakazawa. “Genetic Risk Stratification of Primary Open-Angle Glaucoma in Japanese Individuals” Ophthalmology. 2024 Nov;131(11):1271-1280.
- Ai Fujita Sajiki, Keiko Kataoka, Jun Takeuchi, Hikaru Ota, Yuyako Nakano, Etsuyo Horiguchi, Hiroki Kaneko, Hiroko Terasaki, Yasuki Ito, Koji M Nishiguchi. “Clinical utility of swept-source optical coherence tomography angiography for the diagnosis of exudative maculopathy” Jpn J Ophthalmol. 2024 Nov;68(6):614-620.
- Marko M Popovic, Michael Balas, SriniVas R Sadda, David Sarraf, Ryan Huang, Sophie J Bakri, Audina Berrocal, Andrew Chang, Chui Ming Gemmy Cheung, Sunir Garg, Roxane J Hillier, Frank G Holz, Mark W Johnson, Peter K Kaiser, Peter J Kertes, Timothy Y Y Lai, Jason Noble, Susanna S Park, Yannis M Paulus, Giuseppe Querques, Aleksandra Rachitskaya, Paisan Ruamviboonsuk, Shohista Saidkasimova, Maria Teresa Sandinha, David H Steel, Hiroko Terasaki, Christina Y Weng, Basil K Williams Jr, Lihteh Wu, Rajeev H Muni. “International Classification System for Ocular Complications of Anti-VEGF Agents in Clinical Trials” Ophthalmology. 2024 Dec;131(12):1457-1467.
- Taiga Inooka, Taro Kominami, Ryo Tomita, Ayana Suzumura, Tsuyoshi Matsuno, Junya Ota, Yoshito Koyanagi, Hideo Takeyama, Shinji Ueno, Yasuki Ito, Koji M Nishiguchi, Kenya Yuki. “Assessment of factors affecting anterior chamber depth from data obtained from health checkup participants in Japan” Sci Rep. 2024 Dec 5;14(1):30342.
- Ryo Nonogaki, Hikaru Ota, Jun Takeuchi, Yuyako Nakano, Ai Fujita Sajiki, Takahito Todoroki, Koichi Nakamura, Hiroki Kaneko, Koji M Nishiguchi. “Analysis of the aqueous humor before and after the administration of faricimab in patients with nAMD” Sci Rep. 2024 Dec 30;14(1):31951.
2023
- Panneman DM, Hitti-Malin RJ, Holtes LK, de Bruijn SE, Reurink J, Boonen EGM, Khan MI, Ali M, Andréasson S, De Baere E, Banfi S, Bauwens M, Ben-Yosef T, Bocquet B, De Bruyne M, de la Cerda B, Coppieters F, Farinelli P, Guignard T, Inglehearn CF, Karali M, Kjellström U, Koenekoop R, de Koning B, Leroy BP, McKibbin M, Meunier I, Nikopoulos K, Nishiguchi KM, Poulter JA, Rivolta C, Rodríguez de la Rúa E, Saunders P, Simonelli F, Tatour Y, Testa F, Thiadens AAHJ, Toomes C, Tracewska AM, Tran HV, Ushida H, Vaclavik V, Verhoeven VJM, van de Vorst M, Gilissen C, Hoischen A, Cremers FPM, Roosing S. “Cost-effective sequence analysis of 113 genes in 1,192 probands with retinitis pigmentosa and Leber congenital amaurosis.” Front Cell Dev Biol. 2023 Feb 3;11:1112270.
- Nakano Y, Takeuchi J, Horiguchi E, Ota H, Taki Y, Ito Y, Terasaki H, Nishiguchi KM, Kataoka K. “LONG-TERM MORPHOLOGIC CHANGES IN MACULAR NEOVASCULARIZATION UNDER AFLIBERCEPT TREATMENT WITH A TREAT-AND-EXTEND REGIMEN” Retina. 2023 Mar 1;43(3):412-419.
- Yamada K, Tazaki A, Ushio-Watanabe N, Usui Y, Takeda A, Matsunaga M, Suzumura A, Shimizu H, Zheng H, Ariefta NR, Yamamoto M, Hara H, Goto H, Sonoda KH, Nishiguchi KM, Kato M, Nishikawa Y, Toyokuni S, Kaneko H. “Retinal ferroptosis as a critical mechanism for the induction of retinochoroiditis during ocular toxoplasmosis.” Redox Biol. 2023 Nov;67:102890.
- Ota J, Inooka T, Okado S, Maeda N, Koyanagi Y, Kominami T, Nishiguchi KM, Ueno S. “Pathogenic variants of MFRP and PRSS56 genes are major causes of nanophthalmos in Japanese patients” Ophthalmic Genet. 2023 Oct;44(5):423-429.
- Takeuchi J, Ota H, Nakano Y, Horiguchi E, Taki Y, Ito Y, Terasaki H, Nishiguchi KM, Kataoka K. “Predictive factors for outcomes of half-dose photodynamic therapy combined with aflibercept for pachychoroid neovasculopathy” Graefes Arch Clin Exp Ophthalmol. 2023 Aug;261(8):2235-2243.
- Sajiki AF, Koyanagi Y, Ushida H, Kawano K, Fujita K, Okuda D, Kawabe M, Yamada K, Suzumura A, Kachi S, Kaneko H, Komatsu H, Usui Y, Goto H, Nishiguchi KM. “Association Between Torque Teno Virus and Systemic Immunodeficiency in Patients With Uveitis With a Suspected Infectious Etiology” Am J Ophthalmol. 2023 Oct;254:80-86.
- Akiyama M, Miyake M, Momozawa Y, Arakawa S, Maruyama-Inoue M, Endo M, Iwasaki Y, Ishigaki K, Matoba N, Okada Y, Yasuda M, Oshima Y, Yoshida S, Nakao SY, Morino K, Mori Y, Kido A, Kato A, Yasukawa T, Obata R, Nagai Y, Takahashi K, Fujisawa K, Miki A, Nakamura M, Honda S, Ushida H, Yasuma T, Nishiguchi KM, Mori R, Tanaka K, Wakatsuki Y, Yamashiro K, Kadonosono K, Terao C, Ishibashi T, Tsujikawa A, Sonoda KH, Kubo M, Kamatani Y. “Genome-Wide Association Study of Age-Related Macular Degeneration Reveals 2 New Loci Implying Shared Genetic Components with Central Serous Chorioretinopathy” Ophthalmology. 2023 Apr;130(4):361-372.
- Inoda S, Takahashi H, Maruyama-Inoue M, Ikeda S, Sekiryu T, Itagaki K, Matsumoto H, Mukai R, Nagai Y, Ohnaka M, Kusuhara S, Miki A, Okada AA, Nakayama M, Nishiguchi KM, Takeuchi J, Mori R, Tanaka K, Honda S, Kohno T, Koizumi H, Miyara Y, Inoue Y, Takana H, Iida T, Maruko I, Hayashi A, Ueda-Consolvo T, Yanagi Y. “Incidence and Risk factors of Intraocular Inflammation after Brolucizumab Treatment in Japan: A Multicenter AMD Study” Retina. 2023 Nov 28.
- Inooka T, Kominami T, Yasuda S, Koyanagi Y, Ota J, Okado S, Tomita R, Ito Y, Iwase T, Terasaki H, Nishiguchi KM, Ueno S. “Assessment of factors affecting flicker ERGs recorded with RETeval from data obtained from health checkup screening.” PLoS One. 2023 Apr 24;18(4):e0284686.
- Yamaguchi K, Tomita R, Koyanagi Y, Kawase K, Asaoka R, Terasaki H, Iwase T, Nishiguchi KM. “Abilities of circumpapillary retinal nerve fiber layer thickness and vascular density to discriminate stages in primary open-angle glaucoma” Graefes Arch Clin Exp Ophthalmol. 2023 Nov 3.
- Tomita R, Asaoka R, Hirasawa K, Fujino Y, Nakakura S, Murata H, Omura T, Shoji N, Obana A, Nishiguchi KM, Tanito M. “Accuracy of pattern deviation in estimating the glaucomatous damage in the central 10° visual field in eyes with glaucoma and cataract.” Br J Ophthalmol. 2023 Dec 18;108(1):78-83.
- Hososhima S, Ueno S, Okado S, Inoue KI, Konno M, Yamauchi Y, Inoue K, Terasaki H, Kandori H, Tsunoda SP. “A light-gated cation channel with high reactivity to weak light” Sci Rep. 2023 May 10;13(1):7625.
- Mizobuchi K, Hayashi T, Ueno S, Kondo M, Terasaki H, Aoki T, Nakano T. “One-Year Outcomes of Oral Treatment With Alga Capsules Containing Low Levels of 9-cis-β-Carotene in RDH5-Related Fundus Albipunctatus” Am J Ophthalmol. 2023 Oct;254:193-202.
- Funahashi S, Ito Y, Kataoka K, Takeuchi J, Nakano Y, Fujita A, Horiguchi E, Taki Y, Terasaki H. “SPONTANEOUS CLOSURE OF MACULAR HOLE AFTER VITRECTOMY FOR MYOPIC RETINOSCHISIS WITH FOVEAL DETACHMENT” Retin Cases Brief Rep. 2023 Mar 1;17(2):98-100.
- Iwase T, Ueno Y, Tomita R, Terasaki H. “Relationship Between Retinal Microcirculation and Renal Function in Patients with Diabetes and Chronic Kidney Disease by Laser Speckle Flowgraphy” Life (Basel). 2023 Feb 2;13(2):424.
- Taki Y, Ito Y, Takeuchi J, Ito H, Nakano Y, Sajiki AF, Horiguchi E, Ota H, Kataoka K, Terasaki H. “Displacement of the retina and changes in the foveal avascular zone area after internal limiting membrane peeling for epiretinal membrane” Jpn J Ophthalmol. 2023 Jan;67(1):74-83.
- Matsushita I, Izumi H, Ueno S, Hayashi T, Fujinami K, Tsunoda K, Iwata T, Kiuchi Y, Kondo H. “Functional Characteristics of Diverse PAX6 Mutations Associated with Isolated Foveal Hypoplasia” Genes (Basel). 2023 Jul 21;14(7):1483.
- Matsushita M, Kitoh H, Mishima K, Kamiya Y, Kato D, Takemoto G, Sawamura K, Ueno S, Yasuhiro N, Nishida K, Imagama S. “Phase 1b study on the repurposing of meclizine hydrochloride for children with achondroplasia” PLoS One. 2023 Jul 10;18(7):e0283425.
- Sone J, Ueno S, Akagi A, Miyahara H, Tamai C, Riku Y, Yabata H, Koizumi R, Hattori T, Hirose H, Koyanagi Y, Kobayashi R, Okada H, Kishimoto Y, Hashizume Y, Sobue G, Yoshida M, Iwasaki Y. “NOTCH2NLC GGC repeat expansion causes retinal pathology with intranuclear inclusions throughout the retina and causes visual impairment” Acta Neuropathol Commun. 2023 May 2;11(1):71.
- Hayashi T, Mizobuchi K, Kameya S, Ueno S, Matsuura T, Nakano T. “A mild form of POC1B-associated retinal dystrophy with relatively preserved cone system function” Doc Ophthalmol. 2023 Aug;147(1):59-70.
- Katayama N, Yoshida T, Nakashima T, Ito Y, Teranishi M, Iwase T, Sugiura S, Goto K, Uchida Y, Taki Y, Nakada T, Tada A, Suzuki H, Nakano Y, Shimono M, Saji N, Kogure A, Shimizu E, Sone M, Hamajima N. “Relationship between tinnitus and olfactory dysfunction: audiovisual, olfactory, and medical examinations” Front Public Health. 2023 Apr 20;11:1124404.
- Tomita R, Goto K, Ueno Y, Yamaguchi K, Takeuchi J, Akahori T, Kaneko H, Iwase T. “Narrowing Ratio of Retinal Veins at Arteriovenous Crossing in Patients With Branch Retinal Vein Occlusion Versus That in Healthy Individuals.” Invest Ophthalmol Vis Sci. 2023 Nov 1;64(14):22.
- Tomita R, Iwase T. “Visualization of Changes in Retinal Vascular Resistance Before and After Administration of Anti-Vascular Endothelial Growth Factor for Branch Retinal Vein Occlusion.” Ophthalmic Surg Lasers Imaging Retina. 2023 Sep;54(9):550-551. doi: 10.3928/23258160-20230809-01. Epub 2023 May 1.
2022
- Miyagi M, Takeuchi J, Koyanagi Y, Mizobuchi K, Hayashi T, Ito Y, Terasaki H, Nishiguchi KM, Ueno S. “Clinical findings in eyes with BEST1-related retinopathy complicated by choroidal neovascularization.” Graefes Arch Clin Exp Ophthalmol. 2022 Apr;260(4):1125-1137
- Inooka D, Omori Y, Ouchi N, Ohashi K, Kawakami Y, Koyanagi Y, Koike C, Terasaki H, Nishiguchi KM, Ueno S. “Ablation of Ctrp9, Ligand of AdipoR1, and Lower Number of Cone Photoreceptors in Mouse Retina.” Invest Ophthalmol Vis Sci. 2022 May,63(5):14.
- Ota H, Takeuchi J, Nakano Y, Horiguchi E, Taki Y, Ito Y, Terasaki H, Nishiguchi KM, Kataoka K. “Switching from aflibercept to brolucizumab for the treatment of refractory neovascular age-related macular degeneration.” Jpn J Ophthalmol. 2022 May;66(3):278-284.
- Tomita R, Asaoka R, Hirasawa K, Fujino Y, Nakakura S, Murata H, Omura T, Shoji N, Obana A, Nishiguchi KM, Tanito M. Accuracy of pattern deviation in estimating the glaucomatous damage in the central 10° visual field in eyes with glaucoma and cataract. Br J Ophthalmol. 2022 Oct 19:bjo-2022-322274.
- Horiguchi E, Takeuchi J, Tomita R, Asai K, Nakano Y, Ota H, Taki Y, Ito Y, Terasaki H, Nishiguchi KM, Kataoka K. Choroidal hemodynamics in central serous chorioretinopathy after half-dose photodynamic therapy and the effects of smoking. Sci Rep. 2022 Oct 11;12(1):17032.
- Okado S, Koyanagi Y, Inooka T, Kominami T, Terasaki H, Nishiguchi KM, Ueno S. Assessments of macular function by focal macular electroretinography and static perimetry in eyes with retinitis pigmentosa. Retina. 2022 Nov 1;42(11):2184-2193
- Nakamura K, Takeuchi J, Kataoka K, Ota H, Asai K, Nakano Y, Horiguchi E, Taki Y, Ito Y, Terasaki H, Nishiguchi KM. EFFECTS OF HALF-DOSE PHOTODYNAMIC THERAPY ON CHRONIC CENTRAL SEROUS CHORIORETINOPATHY WITH OR WITHOUT MACULAR NEOVASCULARIZATION ASSESSED USING OPTICAL COHERENCE TOMOGRAPHY ANGIOGRAPHY. Retina. 2022 Dec 1;42(12):2346-2353.
- Shimizu H, Takayama K, Yamada K, Suzumura A, Sato T, Nishio Y, Ito M, Ushida H, Nishiguchi KM, Takeuchi M, Kaneko H. Dimethyl Fumarate Protects Retinal Pigment Epithelium from Blue Light-Induced Oxidative Damage via the Nrf2 Pathway. Antioxidants (Basel). 2022 Dec 26;12(1):45.
2021
- Nishiguchi KM, Miya F, Mori Y, Fujita K, Akiyama M, Kamatani T, Koyanagi Y, Sato K, Takigawa T, Ueno S, Tsugita M, Kunikata H, Cisarova K, Nishino J, Murakami A, Abe T, Momozawa Y, Terasaki H, Wada Y, Sonoda KH, Rivolta C, Tsunoda T, Tsujikawa M, Ikeda Y, Nakazawa T. A hypomorphic variant in EYS detected by genome-wide association study contributes toward retinitis pigmentosa. Commun Biol. 2021 Jan 29;4(1):140.
- Tsunekawa Y, Kataoka K, Asai K, Ito Y, Terasaki H. Four-year outcome of aflibercept administration using a treat-and-extend regimen in eyes with recurrent neovascular age-related macular degeneration. Jpn J Ophthalmol. 2021 Jan;65(1):69-76.
- Takashi N, Nakamura A, Kataoka K, Usui Y, Ito Y, Kaneko H. “Optical coherence tomography angiography for the diagnosis of granulomatosis with polyangiitis with serous retinal detachment: A case report.” Medicine (Baltimore). 2021 Feb19;100(7):e24789.
- Ueno Y, Iwase T, Goto K, Tomita R, Ra E, Yamamoto K, Terasaki H. Association of changes of retinal vessels diameter with ocular blood flow in eyes with diabetic retinopathy. Sci Rep. 2021 Feb 25;11(1):4653.
- Suwa S, Tomita R, Kataoka K, Ueno S. Development of Vogt-Koyanagi-Harada Disease-like Uveitis during Treatment by Anti-programmed Death Ligand-1 Antibody for Non-small Cell Lung Cancer: A Case Report. Ocul Immunol Inflamm. 2021 Apr 2:1-5.
- Ito H, Ito Y, Kataoka K, Ueno S, Takeuchi J, Nakano Y, Fujita A, Horiguchi E, Kaneko H, Iwase T, Terasaki H. Erratum to Association Between Retinal Layer Thickness and Perfusion Status in Extramacular Areas in Diabetic Retinopathy. Am J Ophthalmol 2020; 215:25-36. Am J Ophthalmol. 2021 Apr 13:S0002-9394(20)30675-9.
- Takeuchi J, Kataoka K, Shimizu H, Tomita R, Kominami T, Ushida H, Kaneko H, Ito Y, Terasaki H. Intraoperative and postoperative monitoring of autologous neurosensory retinal flap transplantation for a refractory macular hole associated with high myopia. Retina. 2021 May 1;41(5):921-930.
- Kaneko H, Hirata N, Shimizu H, Kataoka K, Nonobe N, Mokuno K, Terasaki H. Effect of internal limiting membrane peeling on visual field sensitivity in eyes with epiretinal membrane accompanied by glaucoma with hemifield defect and myopia. Jpn J Ophthalmol. 2021 May ;65(3):380-387.
- Takeuchi J, Kataoka K, Shimizu H, Tomita R, Kominami T, Ushida H, Kaneko H, Ito Y, Terasaki H. Intraoperative and Postoperative Monitoring of Autologous Neurosensory Retinal Flap Transplantation for Refractory Macular Hole Associated with High Myopia. Retina. 2021 May 1;41(5):921-930.
- Koyanagi Y, Akiyama M, Nishiguchi KM, Momozawa Y, Kamatani Y, Takata S, Inai C, Iwasaki Y, Kumano M, Murakami Y, Komori S, Gao D, Kurata K, Hosono K, Ueno S, Hotta Y, Murakami A, Terasaki H, Wada Y, Nakazawa T, Ishibashi T, Ikeda Y, Kubo M, Sonoda KH. Regional differences in genes and variants causing retinitis pigmentosa in Japan. Jpn J Ophthalmol. 2021 May;65(3):338-343.
- Iwase C, Iwase T, Tomita R, Akahori T, Yamamoto K, Ra E, Terasaki H. Changes in pulse waveforms in response to intraocular pressure elevation determined by laser speckle flowgraphy in healthy subjects. BMC Ophthalmol. 2021 Aug 21;21(1):303.
- Tomita R, Iwase T, Fukami M, Goto K, Ra E, Terasaki H. Elevated retinal artery vascular resistance determined by novel visualized technique of laser speckle flowgraphy in branch retinal vein occlusion. Sci Rep. 2021 Oct 8;11(1):20034.
- Kaneko H, Takashi N, Matsunaga M, Ito Y, Takeuchi J, Terasaki H, Yatsuya H, Nishiguchi KM. Seasonal variation in submacular hemorrhages in retinal macroaneurysms and its disappearance in age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2021 Dec ;259(12):3589–3596.
2020
- Nakanishi A, Ueno S, Hayashi T, Katagiri S, Ito Y, Kominami T, Fujinami K,Tsunoda K, Iwata T Terasaki H. Changes of cone photoreceptor mosaic in autosomal recessive bestrophinopathy. Retina 2020 Jan;40(1):181-186.
- Matsuura T, Kaneko H, Takayama K, Shibata R, Kataoka K, Ito S, Tsunekawa T, Shimizu H,Suzumura A, Namba R, Ito Y, Murohara T, Terasaki H. “Diacron reactive oxygen metabolitesand biological antioxidant potential tests for patients with age-related macular degeneration“BMC Ophthalmol 2020 Feb 18;20(1):56.
- Yang L, Fujinami K, Ueno S, Kuniyoshi K, Hayashi T, Kondo M, Mizota A, Naoi N, ShinodaK, Kameya S, Fujinami-Yokokawa Y, Liu X, Arno G, Pontikos N, Kominami T, Terasaki H,Sakuramoto H, Katagiri S, Mizobuchi K, Nakamura N, Mawatari G, Kurihara T, Tsubota K,Miyake Y, Yoshitake K, Iwata T, Tsunoda K; JEGC study group. Genetic Spectrum of EYS-associated Retinal Disease in a Large Japanese Cohort: Identification of Disease-associatedVariants with Relatively High Allele Frequency. Sci Rep. 2020 Mar 26;10(1):5497.
- Suzumura A, Kaneko H, Funahashi Y, Takayama K, Nagaya M, Ito S, Okuno T, Hirakata T,Nonobe N, Kataoka K, Simizu H, Namba R, Yamada K, Ye F, Ozawa Y, Yokomizo T, TerasakiH.“Omega-3 Fatty Acid and its Metabolite 18-HEPE Ameliorate Retinal Neuronal CellDysfunction by Enhancing Müller BDNF in Diabetic Retinopathy”Diabetes 2020 Apr; 69(4):724-735.
- Liu X, Fujinami K, Kuniyoshi K, Kondo M, Ueno S, Hayashi T, Mochizuki K, Kameya S, YangL, Fujinami-Yokokawa Y, Arno G, Pontikos N, Sakuramoto H, Kominami T, Terasaki H,Katagiri S, Mizobuchi K, Nakamura N, Yoshitake K, Miyake Y, Li S, Kurihara T, Tsubota K,Iwata T, Tsunoda K; Japan Eye Genetics Consortium. Clinical and Genetic Characteristics of15 Affected Patients From 12 Japanese Families with GUCY2D-Associated Retinal Disorder.Transl Vis Sci Technol. 2020 May 11;9(6):2
- Tomita R, Iwase T, Ueno Y, Goto K, Yamamoto K, Ra E, Terasaki H. Differences in BloodFlow Between Superior and Inferior Retinal Hemispheres. Invest Ophthalmol Vis Sci. 2020May 11;61(5):27.
- Fujinami-Yokokawa Y, Fujinami K, Kuniyoshi K, Hayashi T, Ueno S, Mizota A, Shinoda K,Arno G, Pontikos N, Yang L, Liu X, Sakuramoto H, Katagiri S, Mizobuchi K, Kominami T,Terasaki H, Nakamura N, Kameya S, Yoshitake K, Miyake Y, Kurihara T, Tsubota K, MiyataH, Iwata T, Tsunoda K; Japan Eye Genetics Consortium. Clinical and Genetic Characteristicsof 18 Patients from 13 Japanese Families with CRX-associated retinal disorder: Identificationof Genotype-phenotype Association. Sci Rep. 2020 Jun 12;10(1):9531.
- Yamada K, Kaneko H, Shimizu H, Suzumura A, Namba R, Takayama K, Ito S. Sugimoto M,Terasaki H. “Lamivudine inhibits Alu RNA-induced retinal pigment epitheliumdegeneration via anti-inflammatory and anti-senescence activities.ʼʼ Transl Vis Sci Technol.2020 Jul 1 ;9(8):1.
- Ito H, Ito Y, Kataoka K, Ueno S, Takeuchi J, Nakano Y, Fujita A, Horiguchi E, Kaneko H,Iwase T, Terasaki H. “Association between retinal layer thickness and perfusion status inextramacular areas in diabetic retinopathy”. Am J Ophthalmol. 2020 Jul;215:25-36.Terao R, Kaneko H. “Lipid Signaling in Ocular Neovascularization.” Int J Mol Sci. 2020 Jul4;21(13):4758.
- Yamada K, Kaneko H, Shimizu H, Suzumura A, Namba R, Takayama K, Ito S, Sugimoto M,Terasaki H. “ Lamivudine Inhibits Alu RNA-induced Retinal Pigment EpitheliumDegeneration via Anti-inflammatory and Anti-senescence Activities”. Transl Vis Sci Technol.2020 Jul 1;9(8):1.
- Ito Y, Ito M, Ueno S, Kataoka K, Takeuchi J, Kominami T, Takayama K, Terasaki H. Changesin intraocular pressure and aqueous flare in eyes with multiple evanescent white dot syndrome.Jpn J Ophthalmol. 2020 Jul;64(4):378-384.
- Momota A, Iwase T, Akahori T, Goto K, Yamamoto K, Eimei R, Terasaki H. Associationbetween displacement and thickness of macular after vitrectomy in eyes with epiretinalmembrane. sientific reports 2020 Aug 6;10(1):13227.
- Koyanagi Y, Ueno S, Ito Y, Kominami T, Komori S, Akiyama M, Murakami Y, Ikeda Y, SonodaKH, Terasaki H. Relationship Between Macular Curvature and Common Causative Genes ofRetinitis Pigmentosa in Japanese Patients. Invest Ophthalmol Vis Sci. 2020 Aug 3;61(10):6.
- Shimizu H, Yamada K, Suzumura A, Kataoka K, Takayama K, Sugimoto M, Terasaki H,Kaneko H. “Caveolin-1 Promotes Cellular Senescence in Exchange for Blocking SubretinalFibrosis in Age-Related Macular Degeneration”.Invest Ophthalmol Vis Sci. 2020 Sep1;61(11):21.
- Suzumura A, Terao R, Kaneko H. “Protective Effects and Molecular Signaling of n-3 FattyAcids on Oxidative Stress and Inflammation in Retinal Diseases”. Antioxidants (Basel). 2020Sep 26;9(10):920.
- Suzumura A, Terao R, Kaneko H. “Protective Effects and Molecular Signaling of n-3 FattyAcids on Oxidative Stress and Inflammation in Retinal Diseases”. Antioxidants (Basel). 2020Sep 26;9(10):920.
- Meinert M, Ueno S, Komori S, Koyanagi Y, Sayo A, Andreasson S, Kominami T, Ito Y, TerasakiH. Longitudinal Changes of Macular Curvature in Patients with Retinitis Pigmentosa. TranslVis Sci Technol. 2020 Sep 10;9(10):11.
- Fujinami K, Liu X, Ueno S, Mizota A, Shinoda K, Kuniyoshi K, Fujinami-Yokokawa Y, YangL, Arno G, Pontikos N, Kameya S, Kominami T, Terasaki H, Sakuramoto H, Nakamura N,Kurihara T, Tsubota K, Miyake Y, Yoshiake K, Iwata T, Tsunoda K; Japan Eye GeneticsConsortium Study Group. RP2-associated retinal disorder in a Japanese cohort: Report ofnovel variants and a literature review, identifying a genotype-phenotype association. Am JMed Genet C Semin Med Genet. 2020 Sep;184(3):675-693.
- Ueno S, Koyanagi Y, Kominami T, Ito Y, Kawano K, Nishiguchi KM, Rivolta C, Nakazawa T,Sonoda KH, Terasaki H. Clinical characteristics and high resolution retinal imaging of retinitispigmentosa caused by RP1 gene variants. Jpn J Ophthalmol. 2020 Sep;64(5):485-496.
- Fujita A, Kataoka K, Takeuchi J, Nakano Y, Horiguchi E, Kaneko K, Ito Y, Terasaki H.Diagnostic characteristics of polypoidal choroidal vasculopathy Based on b-scan swept-sourceoptical coherence tomography angiography and its interrater agreement compared withindocyanine green angiography. Retina. 2020 Dec;40(12):2296-2303.
2016
- Takayama K, Ito Y, Kaneko H, Nagasaka Y, Tsunekawa T, Sugita T, Terasaki H. Cross-sectional pupillographic evaluation of relative afferent pupillary defect in age-related macular degeneration. Medicine (Baltimore), 2016; 95(39):e4978.
- Nagasaka Y, Ito Y, Ueno S, Terasaki H.Increased aqueous flare is associated with thickening of inner retinal layers in eyes with retinitis pigmentosa. Sci Rep, 2016; 6:33921.
- Fujinami K, Kameya S, Kikuchi S, Ueno S, Kondo M, Hayashi T, Shinoda K, Machida S, Kuniyoshi K, Kawamura Y, Akahori M, Yoshitake K, Katagiri S, Nakanishi A, Sakuramoto H, Ozawa Y, Tsubota K, Yamaki K, Mizota A, Terasaki H, Miyake Y, Iwata T, Tsunoda K.Novel RP1L1 Variants and Genotype-Photoreceptor Microstructural Phenotype Associations in Cohort of Japanese Patients With Occult Macular Dystrophy. Invest Ophthalmol Vis Sci, 2016; 57(11):4837-4846.
- Asami T, Terasaki H, Ito Y, Sugita T, Kaneko H, Nishiyama J, Namiki H, Kobayashi M, Nishizawa N. Development of a fiber-optic optical coherence tomography probe for intraocular use. Invest Ophthalmol Vis Sci, 2016; 57(9):OCT568-574.
- Iwase T, Yamamoto K, Yanagida K, Kobayashi M, Ra E, Murotani K, Terasaki H. Change in refraction after lens-sparing vitrectomy for rhegmatogenous retinal detachment and epiretinal membrane. Medicine (Baltimore), 2016; 95(32):e4317.
- Hasegawa T, Muraoka Y, Ikeda HO, Tsuruyama T, Kondo M, Terasaki H, Kakizuka A, Yoshimura N. Neuoroprotective efficacies by KUS121, a VCP modulator, on animal models of retinal degeneration. Sci Rep, 2016; 6:31184.
- Nakanishi A, Ueno S, Hayashi T, Katagiri S, Kominami T, Ito Y, Gekka T, Masuda Y, Tsuneoka H, Shinoda K, Hirakata A, Inoue M, Fujinami K, Tsunoda K, Iwata T, Terasaki H. Clinical and genetic findings of autosomal recessive bestrophinopathy in Japanese cohort. Am J Ophthalmol, 2016;168:86-94.
- Wang C, Hosono K, Kachi S, Suto K, Nakamura M, Terasaki H, Miyake Y, Hotta Y, Minoshima S. Novel OPN1LW/OPN1MW deletion mutations in 2 Japanese families with blue cone monochromacy. Hum Genome Var, 2016;3:16011.
- Takayama K, Kaneko H, Hwang SJ, Ye F, Higuchi A, Tsunekawa T, Matsuura T, Iwase T, Asami T, Ito Y, Ueno S, Yasuda S, Nonobe N, Terasaki H. Increased ocular levels of microRNA-148a in cases of retinal detachment promote epithelial- mesenchymal transition. Invest Ophthalmol Vis Sci, 2016;57(6):2699-2705.
- Nakanishi A, Ueno S, Hayashi T, Katagiri S, Kominami T, Ito Y, Gekka T, Masuda Y, Tsuneoka H, Shinoda K, Hirakata A, Inoue M, Fujinami K, Tsunoda K, Iwata T, Terasaki H. Clinical and genetic findings of autosomal recessive bestrophinopathy in Japanese cohort. Am J Ophthalmol, 2016;168:86-94.
- Kominami T, Ueno S, Nakanishi A, Kominami A, Kondo M, Furukawa T, Terasaki H. Temporal properties of cone ERGs of pikachurin null mutant mouse. Invest Ophthalmol Vis Sci, 2016;57(3):1264-1269.
- Kobayashi M, Iwase T, Yamamoto K, Ra E, Murotani K, Matsui S, Terasaki H. Association between photoreceptor regeneration and visual acuity following surgery for rhegmatogenous retinal detachment. Invest Ophthalmol Vis Sci, 2016;57(3):889-898.
- Ye F, Kaneko H, Hayashi Y, Takayama K, Hwang SJ, Nishizawa Y, Kimoto R, Nagasaka Y, Tsunekawa T, Matsuura T, Yasukawa T, Kondo T, Terasaki H. Malondialdehyde induces autophagy dysfunction and VEGF secretion in the retinal pigment epithelium in age-related macular degeneration. Free Radic Biol Med, 2016; 94:121-134.
- Bogdanovich S, Kim Y, Mizutani T, Yasuma R, Tudisco L, Cicatiello V, Bastos-Carvalho A, Kerur N, Hirano Y, Baffi JZ, Tarallo V, Li S, Yasuma T, Arpitha P, Fowler BJ, Wright CB, Apicella I, Greco A, Brunetti A, Ruvo M, Sandomenico A, Nozaki M, Ijima R, Kaneko H, Ogura Y, Terasaki H, Ambati BK, Leusen JH, Langdon WY, Clark MR, Armour KL, Bruhns P, Verbeek JS, Gelfand BD, De Falco S, Ambati J. Human IgG1 antibodies suppress angiogenesis in a target-independent manner. Signal Transduct Target Ther, 2016;1.
- Sato C, Kaneko H, Kondo T, Takayama K, Yasuda S, Terasaki H. Association of intraocular pressure changes with right ventricular diameter and brain natriuretic peptide in a case of pulmonary arterial hypertension. J Glaucoma, 2016;25(3):e295-298.
- Shirai H, Mandai M, Matsushita K, Kuwahara A, Yonemura S, Nakano T, Assawachananont J, Kimura T, Saito K, Terasaki H, Eiraku M, Sasai Y, Takahashi M. Transplantation of human embryonic stem cell-derived retinal tissue in two primate models of retinal degeneration. Proc Natl Acad Sci U S A, 2016;113(1):E81-90.
- Higashide T, Ohkubo S, Hangai M, Ito Y, Shimada N, Ohno-Matsui K, Terasaki H, Sugiyama K, Chew P, Li KK, Yoshimura N. Influence of clinical factors and magnification correction on normal thickness profiles of macular retinal layers using optical coherence tomography. PLoS One, 2016;11(1):e0147782.
2015
- Matsui A, Kaneko H, Kachi S, Ye F, Hwang SJ, Takayama K, Nagasaka Y, Sugita T, Terasaki H. Expression of vascular endothelial growth factor by retinal pigment epithelial cells induced by amyloid-β is depressed by an endoplasmic reticulum stress inhibitor. Ophthalmic Res, 2015; 55(1):37-44.
- Nakanishi A, Ueno S, Kawano K, Ito Y, Kominami T, Yasuda S, Kondo M, Tsunoda, K, Iwata T, Terasaki H. Pathologic changes of cone photoreceptors in eyes with occult macular dystrophy. Invest Ophthalmol Vis Sci, 2015;56(12):7243-7249.
- Futamura Y, Asami T, Nonobe N, Kachi S, Ito Y, Sato Y, Hayakawa M, Terasaki H. Buckling surgery and supplemental intravitreal bevacizumab or photocoagulation on stage 4 retinopathy of prematurity eyes. Jpn J Ophthalmol, 2015;59(6):378-388.
- Nakagami Y, Hatano E, Inoue T, Yoshida K, Kondo M, Terasaki H. Cytoprotective effects of a novel Nrf2 activator, RS9, in rhodopsin Pro347Leu rabbits. Curr Eye Res, 20152:1-4.
- Brown DM, Schmidt-Erfurth U, Do DV, Holz FG, Boyer DS, Midena E, Heier JS, Terasaki H, Kaiser PK, Marcus DM, Nguyen QD, Jaffe GJ, Slakter JS, Simader C, Soo Y, Schmelter T, Yancopoulos GD, Stahl N, Vitti R, Berliner AJ, Zeitz O, Metzig C,Korobelnik JF. Intravitreal aflibercept for diabetic macular edema: 100-week results from the VISTA and VIVID studies. Ophthalmology, 2015;122(10):2044-2052.
- Kaneko H, Ra E, Kawano K, Yasukawa T, Takayama K, Iwase T, Terasaki H. Surgical videos with synchronised vertical 2-split screens recording the surgeons' hand movement. Ophthalmologica, 2015;234(4):243-246.
- Yasuda S, Kachi S, Ueno S, Piao CH, Terasaki H. Flicker electroretinograms before and after intravitreal ranibizumab injection in eyes with central retinal vein occlusion. Acta Ophthalmol, 2015;93(6):e465-468.
- Sato Y, Oshiro M, Takemoto K, Hosono H, Saito A, Kondo T, Aizu K, Matsusawa M, Futamura Y, Asami T, Terasaki H, Hayakawa M. Multicenter observational study comparing sedation/ analgesia protocols for laser photocoagulation treatment of retinopathy of prematurity. J Perinatol, 2015;35(9):965-969.
- Iwase T, Ra E, Yamamoto K, Kaneko H, Ito Y, Terasaki H. Differences of retinal blood flow between arteries and veins determined by laser speckle flowgraphy in healthy subjects. Medicine (Baltimore), 2015;94(33):e1256.
- Ueno S, Kawano K, Ito Y, Ra E, Nakanishi A, Nagaya M, Terasaki H. Near-infrared reflectance imaging in eyes with acute zonal occult outer retinopathy. Retina, 2015;35(8):1521-1530.
- Gomi F, Oshima Y, Mori R, Kano M, Saito M, Yamashita A, Iwata E, Maruko R; Fujisan Study Group. Initial versus delayed photodynamic therapy in combination with anibizumab for treatment of polypoidal choroidal vasculopathy: The Fujisan Study. Retina, 2015;35(8):1569-1576.
- Asakawa K, Ishikawa H, Uga S, Mashimo K, Shimizu K, Kondo M, Terasaki H. Functional and morphological study of retinal photoreceptor cell degeneration in transgenic rabbits with a Pro347Leu rhodopsin mutation. Jpn J Ophthalmol, 2015;59(5):353-363.
- Yanagida K, Iwase T, Yamamoto K, Ra E, Kaneko H, Murotani K, Matsui S, Terasaki H. Sex-related differences in ocular blood flow of healthy subjects using laser speckle flowgraphy. Invest Ophthalmol Vis Sci, 2015;56(8):4880-4890.
- Yasuda S, Kachi S, Kondo M, Ueno S, Kaneko H, Terasaki H. Significant correlation between retinal venous tortuosity and aqueous vascular endothelial growth factor concentration in eyes with central retinal vein occlusion. PLoS One, 2015;10(7):e0134267.
- Nagaya M, Ueno S, Kominami T, Nakanishi A, Koyasu T, Kondo M, Furukawa T, Terasaki H. Pikachurin protein required for increase of cone electroretinogram b-wave during light adaptation. PLoS One, 2015;10(6):e0128921.
- Yamamoto K, Iwase T, Ushida H, Sugita T, Terasaki H. Changes in retinochoroidal thickness after vitrectomy for proliferative diabetic retinopathy. Invest Ophthalmol Vis Sci, 2015;56(5):3034-3040.
- Kataoka K, Matsumoto H, Kaneko H, Notomi S, Takeuchi K, Sweigard JH, Atik A, Murakami Y, Connor KM, Terasaki H, Miller JW, Vavvas DG. Macrophage- and RIP3-dependent inflammasome activation exacerbates retinal detachment-induced photoreceptor cell death. Cell Death Dis, 2015;6:e1731.
- Ijima R, Kaneko H, Ye F, Takayama K, Nagasaka Y, Kataoka K, Funahashi Y, Iwase T, Kachi S, Kato S, Terasaki H. Suppression of laser-induced choroidal neovascularization by the oral medicine targeting histamine receptor H4 in mice. Transl Vis Sci Technol, 2015;4(2):6.
- Iwase T, Yamamoto K, Ra E, Murotani K, Matsui S, Terasaki H. Diurnal variations in blood flow at optic nerve head and choroid in healthy eyes: diurnal variations in blood flow. Medicine (Baltimore), 2015;94(6):e519.
- Asami T, Kachi S, Mohamed UA, Ito Y, Terasaki H. High osmolarity effect of intravitreal plasmin enzyme on rabbit retina. Nagoya J Med Sci, 2015;77(1-2):245-252.
- Ueno S, Nakanishi A, Nishi K, Suzuki S, Terasaki H. Case of paraneoplastic retinopathy with retinal ON-bipolar cell dysfunction and subsequent resolution of ERGs. Doc Ophthalmol, 2015; 130(1):71-76.
- Kuniyoshi K, Terasaki H, Arai M, Hirose T. Macular electroretinogram in stargardt's disease/fundus flavimaculatus. Ophthalmologica, 2015;233(2):113-114.
- Ogura Y, Terasaki H, Gomi F, Yuzawa M, Iida T, Honda M, Nishijo K, Sowade O, Komori T, Schmidt-Erfurth U, Simader C, Chong V; for the VIEW 2 Investigators. Efficacy and safety of intravitreal aflibercept injection in wet age-related macular degeneration: outcomes in the Japanese subgroup of the VIEW2 study. Br J Ophthalmol, 2015;99(1):92-97.
- Ye F, Kaneko H, Nagasaka Y, Ijima R, Nakamura K, Nagaya M, Takayama K, Kajiyama H, Senga T, Tanaka H, Mizuno M, Kikkawa F, Hori M, Terasaki H. Plasma-activated medium suppresses choroidal neovascularization in mice: a new therapeutic concept for age-related macular degeneration. Sci Rep, 2015;5:7705.
2014
- Ueno S, Ito Y, Maruko R, Kondo M, Terasaki H. Choroidal atrophy in a patient with paraneoplastic retinopathy and anti-TRPM1 antibody. Clin Ophthalmol, 2014;8:369-373.
- Kaneko H, Ye F, Ijima R, Kachi S, Kato S, Nagaya M, Higuchi A, Terasaki H. Histamine receptor h4 as a new therapeutic target for choroidal neovascularization in age-related macular degeneration. Br J Pharmacol, 2014; 171:3754-3763.
- Hirano Y, Yasuma T, Mizutani T, Fowler B, Tarallo V, Yasuma R, Kim Y, Carvalho AB, Kerur N, Gelfand B, He S, Zhang X, Nozaki M, Ijima R, Kaneko H, Ogura Y, Terasaki H, Nunez G, Ambati B, Hinton D, Nagai H, Haro I, Ambati J: IL18 is not therapeutic for neovascular age-related macular degeneration. Nat Med, 2014;20(12): 1372-1375.
- Korobelnik JF, Do DV, Schmidt-Erfurth U, Boyer DS, Holz FG, Heier JS, Midena E, Kaiser PK, Terasaki H, Marcus DM, Nguyen QD, Jaffe GJ, Slakter JS, Simader C, Soo Y, Schmelter T, Yancopoulos GD, Stahl N, Vitti R, Berliner AJ, Zeitz O, Metzig C, Brown DM. Intravitreal Aflibercept for Diabetic Macular Edema. Ophthalmology, 2014;121(11):2247-2254.
- Ijima R, Kaneko H, Ye F, Nagasaka Y, Takayama K, Kataoka K, Kachi S, Iwase T, Terasaki H. Interleukin-18 induces retinal pigment epithelium degeneration in mice. Invest Ophthalmol Vis Sci, 2014;55(10):6673-6678.
- Zhao Y, Hosono K, Suto K, Ishigami C, Arai Y, Hikoya A, Hirami Y, Ohtsubo M, Ueno S, Terasaki H, Sato M, Nakanishi H, Endo S, Mizuta K, Mineta H, Kondo M, Takahashi M, Minoshima S, Hotta Y. The first USH2A mutation analysis of Japanese autosomal recessive retinitis pigmentosa patients: a totally different mutation profile with the lack of frequent mutations found in Caucasian patients. J Hum Genet, 2014;59(9):521-528.
- Shen J, Choy DF, Yoshida T, Iwase T, Hafiz G, Xie B, Hackett SF, Arron JR, Campochiaro PA. Interleukin-18 has antipermeablity and antiangiogenic activities in the eye: reciprocal suppression with VEGF. J Cell Physiol, 2014;229(8):974-983.
- Asami T, Terasaki H. Development of caliper for scleral measurements during scleral buckling surgery. Retina, 2014;34(8):1713-1714.
- Iwase T, Oveson BC. Long-term outcome after vitrectomy for macular edema with retinal vein occlusion dividing into the occlusion site. J Ophthalmol, 2014:198782.
- Matsui Y, Matsubara H, Ueno S, Ito Y, Terasaki H, Kondo M. Changes in outer retinal microstructures during six month period in eyes with acute zonal occult outer retinopathy-complex. PLoS One, 2014; 9(10):e110592.
- Ogura Y, Roider J, Korobelnik JF, Holz FG, Simader C, Schmidt-Erfurth U, Vitti R, Berliner AJ, Hiemeyer F, Stemper B, Zeitz O, Sandbrink R; GALILEO Study Group;GALILEO Study Group. Intravitreal aflibercept for macular edema secondary to central retinal vein occlusion: 18-month results of the phase 3 GALILEO study. Am J Ophthalmol, 2014;158(5):1032-1038.e2.
- Iwase T, Oveson BC, Jo YJ. Clear corneal vitrectomy combined with phacoemulsification and foldable intraocular lens implantation. Clin Experiment Ophthalmol, 2014;42(5):452-458.
- Iguchi Y, Asami T, Ueno S, Ushida H, Maruko R, Oiwa K, Terasaki H. Changes in vitreous temperature during intravitreal surgery. Invest Ophthalmol Vis Sci, 2014;55(4):2344-2349.
MESSAGE
Call for graduate students
Please contact us through our web site (http://med-nagoya-ganka.jp/inquiry) if you are interested in our department.

